Heart Transplant
On this page
Heart Transplant
What is a heart transplant?
A heart transplant is the most advanced treatment for end-stage heart disease. When there is no other effective medical or surgical treatment available, a heart transplant is the final option for treating the disease. This complex procedure involves many steps, including evaluation and testing, patient education and support, donor matching, transplant surgery, and long-term follow-up care.
Heart transplantation is only available to patients who have gone through a comprehensive assessment process to confirm their eligibility.
How does a heart transplant work?
Prior to the transplant, we will need to locate a donor heart. Once a compatible heart is found, you will have surgery to replace your heart with the donor heart. Following your transplant, your doctor will monitor your heart muscle cells and arteries to see how your body is adapting to the new heart.
After the transplant, you'll also need to take immunosuppressive drugs to prevent your body from rejecting the new heart. Your doctor will balance these medications to minimize the risk of side effects they can cause, including infection or cancer.
In some cases, the body will not adapt to the new heart. If this happens, your doctor will discuss next steps with you.
How do I know if I need a heart transplant?
A heart transplant may be necessary when your heart is no longer able to pump blood effectively throughout your body and no other treatments are able to fix the problem. A number of conditions can damage your heart to the point where other treatments are unsuccessful and a transplant offers the best chance of a cure. They include:
- Congenital heart disease
- Coronary artery disease
- Heart failure
- Pulmonary hypertension
- Valvular heart disease
- Heart arrhythmias
- Failure of a previous heart transplant
Evaluation for a heart transplant
If your cardiologist believes that your heart disease is so advanced that there are no other treatment options, they may ask to have you evaluated for a heart transplant. This evaluation will determine if you are a good candidate for this surgery.
You might not be eligible for a heart transplant if you have certain conditions, including:
- Irreversible pulmonary hypertension
- Cancer
- HIV
- Active drug or alcohol addiction
- Acute mental incompetence
- Severe muscle loss due to malnutrition, called cardiac cachexia
A number of other conditions are evaluated on an individual basis to determine if a transplant is right for you.
Initial assessment
Using information from your referring doctor, our staff will determine if you are generally a good fit for transplantation. After this initial assessment, they will do a more thorough evaluation. Our approach to this is flexible, although we do insist that every potential candidate and their family visit UCSF at least once before the transplant.
All candidates are seen by UCSF's transplant team. This team includes a cardiologist, surgeon, transplant coordinator and social worker. If you live far from San Francisco, the team can work with your doctor to complete portions of the assessment closer to your home.
This pre-transplant evaluation includes an assessment of your heart as well as the rest of your body. Stable patients can usually complete the standard pre-transplant selection testing without being admitted to a hospital.
Heart-related medical tests
One of the most important parts of the evaluation for a heart transplant is examining your pulmonary vascular health. If you have pulmonary hypertension, we need to determine how severe it is and if it can be treated. The tests for this are done in the hospital through right heart catheterization and continuous hemodynamic monitoring, which measures your circulatory function over time. These tests often take place over six to 12 hours. Because the results of these tests are critical in determining suitability for a heart transplant, we prefer to perform them at UCSF.
Additional tests during your cardiac assessment may include:
- Non-invasive studies. Exams such as echocardiography and radionuclide scans evaluate the function of the heart muscle.
- Perfusion scans. These assess breathing and circulation in all parts of the lungs.
- Oxygen measurement. This evaluation includes exercise tests to measure your maximal oxygen uptake.
Some patients also may need formal cardiac catheterization, which could include coronary angiography and ventriculography, myocardial biopsy and electrophysiologic studies.
Non-heart-related medical tests
There are also some non-heart-related tests and assessments that are part of the pre-transplant evaluation, including:
- Pulmonary function testing, including spirometry and arterial blood gases
- Lab tests for kidney and liver function
- Interviews with a social worker, transplant coordinator and psychiatrist
- Interviews with the hospital administration about financial security
- Infectious disease screening, including serology and skin testing
- Immunogenetics, including assessment of your blood and tissue types as well as checking your human leukocyte antigen level using a histocompatibility antigen test
- Cancer screening that includes chest X-rays and stool samples
- Mammograms, breast and pelvic exams for women
- Prostate-specific antigen (PSA) and prostate exams for men
Depending on your specific situation, we may run additional tests during the initial screening.
Health and lifestyle assessments
As part of the evaluation process, your doctor will look at any health and lifestyle factors that could impact your eligibility for a heart transplant. Your medical team will assess potentially reversible conditions such as:
- Smoking
- Drug addiction
- Obesity
- Mental distress
- Financial problems
Confirmation of eligibility for heart transplantation
Patients are selected for heart transplantation based on a recommendation from the USCF multidisciplinary heart transplant team. This team is made up of representatives from various departments including surgery, internal medicine, nursing, psychiatry, social work, pathology and hospital administration.
After you complete the interview process and all pre-transplant testing, your case will be presented and discussed at our weekly transplant meeting.
After this discussion, the transplant team will decide to do one of the following:
- Accept you for transplantation.
- Provisionally accept you, pending resolution of one or more minor issues.
- Not accept you at the present time but recommend that you may be considered at a future date.
- Categorically not accept you.
All decisions of the committee are based on group consensus. In difficult cases, UCSF's ethics committee is available to offer their expertise.
Once we determine that you would benefit from transplant surgery, your name will be placed on a waiting list to receive a donor heart. There are currently not enough donor hearts available for the people who need them. Under national regulations, hearts must go to the sickest patients first in a given area.
Waiting for a donor heart
If you are accepted for transplantation, you are listed nationally with the California Transplant Donor Network. The listing is made according to the organ(s) you require – just a heart or both heart and lung – as well as your blood group and acceptable donor height range.
Allocation of donor hearts is done at the local and regional level strictly according to national policy. The two main features of this policy include:
- Patients who require combined heart and lung transplantation are given priority over those requiring an isolated heart transplant.
- Heart transplant recipients are prioritized according to how long they have been "actively" on the waiting list.
While they wait, most patients continue to receive medical care from doctors in their local community. A few choose to transfer their care to UCSF. In either case, we maintain close contact with your referring doctor.
All patients on the waiting list are seen at least every three months in the outpatient clinic by our transplant cardiologist and transplant coordinator. Depending on your condition, you may need additional visits. During these visits, we will reassess your continued candidacy for transplantation and, if necessary, you will have more consultations.
These visits usually take place around the same time as the monthly meetings of our Transplant Program's support group. Patients on the waiting list are encouraged to attend these meetings.
New medical conditions and heart transplantation
If you experience a new medical condition that could affect your transplantation eligibility, your local doctor will immediately inform the transplant team. If your condition warrants, you may be temporarily or permanently removed from the "active" waiting list.
Patients whose clinical condition deteriorates while on the waiting list are either admitted directly or transferred to UCSF from their community hospital once their condition has stabilized.
Additional heart transplant support
The USCF Heart Transplant Program has access to a variety of medications and devices, including pacemakers, defibrillators and ventricular assist devices (VADs). These treatments can support patients with severe heart conditions until they receive their new heart.
UCSF is part of the United Network for Organ Sharing (UNOS). We helped start the California Transplant Donor Network (CTDN), an independent group that works with transplant centers in this region. The CTDN has connections with over 150 hospitals in Northern and Central California and Northern Nevada. It helps find potential donors, manage donor processes, and provide education about organ donation and transplants.
Procedure for a heart transplant
Heart transplant surgery involves removing most of your diseased heart and inserting one from a person who has died. You will be called to come to the hospital immediately once you have been assigned a donor heart. When you arrive, you will go to the Cardiac Critical Care Unit for a physical exam and more tests, including blood and urine samples.
You will be prepared for surgery, which includes inserting intravenous lines and a catheter in your neck to measure the pressure in your heart.
You will be given anesthesia so that you will sleep through the surgery. You will also receive immunosuppressive drugs before and during the procedure. These drugs help to prevent your body from rejecting the new heart.
A typical heart transplant surgery takes about four to six hours and involves:
- A major incision down your chest. Your breastbone is split in half.
- Your main arteries are connected to a heart-lung bypass machine to pump your blood. A ventilator will help you breathe.
- Most heart transplants are done using orthotopic surgery. This is a method where most of your heart is removed but the back halves of both upper chambers, called the atria, are left in place. Then the front half of the donor heart is sewn to the back half of the old heart.
- The donor's aorta and pulmonary arteries are connected to yours. The bypass machine is then disconnected, and your new heart begins the work of pumping blood.
- Your incisions are closed.
This surgery is considered less complicated than most heart bypass surgeries, including coronary artery bypass graft (CABG).
Recovery from a heart transplant
After your surgery, you will wake up in a special sterile room to ensure that you aren't exposed to infection. Staff and visitors must take measures to make sure that they do not bring in germs by scrubbing their hands and wearing protective masks and gowns.
Once you can breathe on your own, the ventilator will be removed. However, you will remain connected to various monitors and catheters. When you are stronger, you may be moved to a general hospital room.
You will have to take precautions to prevent your exposure to infection for the rest of your life. Much of the rest of your hospital recovery will include education and training related to taking care of yourself. This includes learning about the anti-rejection medications you will need to take, how to follow a heart-healthy low-fat diet and other changes.
If you don't have any complications, you will be in the hospital for about 10 days.
After the hospital
Once you leave the hospital, you will need regular follow-up visits to monitor your progress. For the first two months after the transplant, you will need to see your doctor every one to two weeks.
If everything goes well, after six months the visits will decrease to one- or two-month intervals. After a year, these visits may be decreased to three- to six-month intervals. Follow-up care is tracked on a quarterly basis; we monitor both routine and crisis visits for all patients.
You will be able to return to your normal activities gradually. You may resume driving a car when your sternum, or breastbone, is fully healed, which takes approximately six weeks. You may return to work two to three months after the transplant surgery. It generally takes three to six months to fully recover from heart transplant surgery. However, age and previous medical history problems may cause the recovery period to take longer.
Awards & recognition

One of the nation's best for heart & vascular care
Explore what we do
UCSF's 35 years of heart transplant experience
Recommended reading

FAQ: Heart Transplant
Find answers to commonly asked questions about receiving a heart transplant, including waiting list times, surgery expectations and recovery.
More treatment info
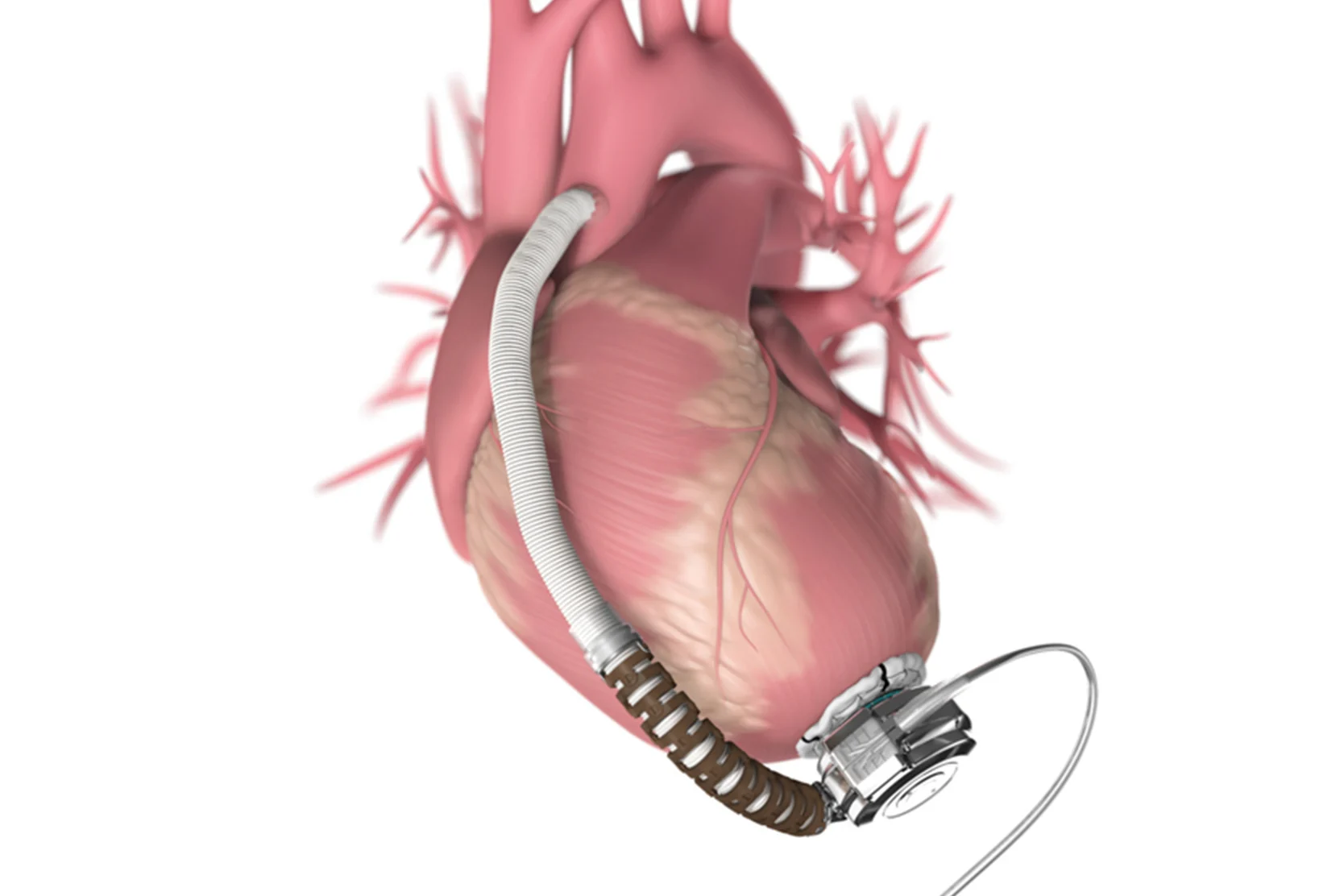
Ventricular Assist Device (VAD)
Learn about the ventricular assist device, or VAD, a mechanical pump used to support heart function and blood flow in people with weak or failing hearts.
Helpful resources
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.








