Melanoma

Overview
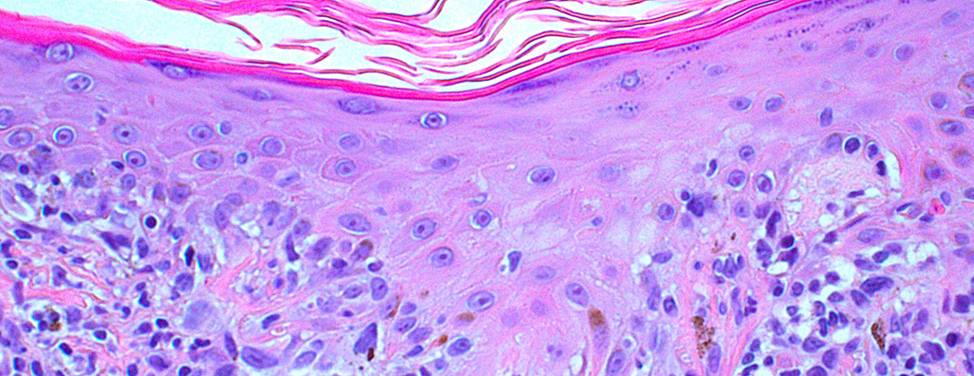
Melanoma is cancer that arises from the pigment-producing cells in the uppermost layer of the skin. These cells are called melanocytes.
Melanoma that originates in the skin is called cutaneous melanoma. It also may occur in the eye, a condition called ocular melanoma or intraocular melanoma. In rare cases, melanoma may begin in the digestive tract called meninges, lymph nodes or other parts of the body where there are melanocytes.
Ultraviolet radiation, which is present in sunlight and in tanning beds, probably sets off many cases of melanoma by causing genetic damage in melanocytes. Children and adolescents are especially sensitive to the effects of ultraviolet light.
Melanoma is potentially life-threatening because it can travel from the skin to other parts of the body. With early diagnosis, however, survival rates are encouraging. The goal is to recgonize melanoma early. Often, the first signs of melanoma are changes in a mole or the appearance of a new colored spot on the skin.
When melanoma spreads, cancer cells are found in the lymphatic system. If the disease spreads to other parts of the body, it's called metastatic melanoma.
The chance of developing melanoma increases with age, but it affects people of all ages and is one of the most common cancers in young adults.
Our Approach to Melanoma
UCSF provides advanced care for patients with all stages of melanoma, from early lesions to advanced metastatic cancer. We also care for patients who are at higher risk of developing melanoma due to family history, genetic mutations or having many abnormal moles.
Our team includes dermatologists, medical and surgical oncologists, radiation oncologists, geneticists and dermatopathologists (subspecialists with advanced training in analyzing tissue microscopically). These experts work together to evaluate your case and personalize your treatment plan. We also offer access to clinical trials, which are studies to evaluate new treatments.
In addition, we provide a variety of resources to support you and your family while under our care at UCSF.
Awards & recognition
-

Among the top hospitals in the nation
-

Best in Northern California and No. 7 in the nation for cancer care
-

Designated comprehensive cancer center
-

melanoma patients seen each year
Signs & symptoms
Often, the first sign of melanoma is a change in the size, shape, color or feel of an existing mole. Most melanomas have a black or blue-black area. Melanoma also may appear as a new, black, abnormal or "ugly-looking" mole.
Rarely, melanoma is not pigmented and is more difficult to diagnose. It may appear as a non-healing ulcer or a new scar-like lump in the skin.
The warning signs are sometimes referred to as ABCDE:
- Asymmetry Two halves of a lesion that are not the same
- Border Borders of a lesion are irregular, scalloped or vague
- Color Color varies from one area to another, including shades of tan or brown as well as black, blue, red and white
- Diameter A lesion that is greater than 6 millimeters in diameter, about the size of a pencil eraser
- Evolution Lesions that change or evolve
The "ABCDE" rule is an easy guide to the usual signs of melanoma.
Some melanomas don't fit the ABCDE rule, so it's important to be aware of changes in skin markings or new spots.
Other warning signs are:
- A sore that doesn't heal
- A new growth
- Spread of pigment, or color, from the border of a spot to surrounding skin
- Redness or a new swelling beyond the border of a mole
- Change in sensation such as itchiness, tenderness or pain
- Change in a mole's surface such as scaling, oozing, bleeding or the appearance of a bump or nodule
Contact your primary care doctor or dermatologist if you find changes that match the ABCDE signs or these other warning signs.
Diagnosis
If your doctor suspects that a spot on the skin is melanoma, you will need a biopsy, which is the only way to make a definite diagnosis. In this procedure, your doctor tries to remove all of the suspicious-looking growth. If the growth is too large to be removed entirely, your doctor may remove a sample of the tissue.
A biopsy usually can be done in the doctor's office using a local anesthetic. A pathologist then examines the tissue under a microscope to check for cancer cells.
Often, the pathologist can easily tell whether these cells represent melanoma or a non-cancerous mole. Sometimes, however, the distinction can be tricky, and special stains or further diagnostic tests must be performed to make the diagnosis. Distinguishing between cancerous and non-cancerous tumors can make all the difference for a patient, as the treatment and outcomes can be very different.
A pathologist can identify many other characteristics of the melanoma to determine how likely the cancer can be successfully treated. If you've had a biopsy at another medical center, we will ask an experienced pathologist at UCSF to review them as well.
Melanoma Staging
- Stage 0 These melanomas are confined to the top most layer of the skin, called the epidermis. In most cases, patients can be cured with surgery to remove the cancer. However, these patients should be monitored for the small risk of melanoma recurrence as well as the development of a second, unrelated skin melanoma.
- Stage I Unlike stage 0 melanoma, these melanomas have invaded through the epidermis. They are considered to be the thinnest of the "invasive" melanomas. There is a small chance that some of these melanomas have spread microscopically to the lymph nodes. In cases with a substantial risk of lymph node involvement, a sentinel lymph node biopsy may be performed, usually at the same time as the surgical removal of the skin melanoma.
- Stage II These are thicker melanomas that have invaded deeper into the skin. As a melanoma becomes deeper, there is a greater possibility that it can spread to other sites in the body. Sentinel lymph node biopsies may be performed when the skin melanoma is surgically removed. In cases where there is a high risk of melanoma developing elsewhere in the body, adjuvant treatment — treatment that attempts to lower the risk of melanoma recurrence — may be offered after the surgery.
- Stage III These include melanomas that have spread to the local lymph nodes. These melanomas have a substantial risk of recurring, or manifesting in distant organs. Therefore adjuvant therapy — treatment that attempts to lower the risk of melanoma recurrence — is offered after the melanoma is surgically removed. Radiation treatment may be considered in certain patients.
- Stage IV In this stage, the cancer has spread to distant organs. In general, patients are treated with systemic therapy, or therapy that targets the entire body. Radiation treatment may be recommended, as well as experimental treatments as part of a clinical trial or study. At the UCSF Melanoma Center, each patient's case is assessed individually to find the best treatment options.
Genetic Mutations in Melanoma
All melanomas are not alike. Scientists have discovered that melanomas tend to have specific mutations in their DNA, depending on where they originated.
The UCSF Melanoma Center has the ability to analyze cancer cells to test for specific mutations, including the genes known as BRAF, NRAS and KIT. A mutation in one of the genes may cause the melanoma to be more responsive to certain treatments. We offer mutation testing to patients who are identified as most likely to benefit from this service.
Treatments
Surgery to remove melanoma is the standard initial treatment. It is necessary to remove not only the tumor but also some normal tissue around it, called the margin, to reduce the chance that any cancer remains. The width and depth of surrounding skin to be removed depends on the thickness of the melanoma and how deeply it has invaded the skin.
Chemotherapy
Chemotherapy is the use of drugs to kill cancer cells. It is generally a systemic therapy, meaning that it can affect cancer cells throughout the body. In chemotherapy, one or more anticancer drugs are given orally or by injection into a blood vessel.
Chemotherapy usually is given in cycles — a treatment period followed by a recovery period, then another treatment period, and so on. Chemotherapy can be administered in a clinic, doctor's office, hospital or at home. Depending on the drugs given and your general health, a short hospital stay may be needed.
Biological Therapy
Biological therapy, also called immunotherapy, is a form of treatment that uses the body's immune system, either directly or indirectly, to fight cancer or to lessen side effects caused by some cancer treatments. Biological therapy also is a systemic therapy and involves the use of substances called biological response modifiers (BRMs). The body normally produces these substances in small amounts in response to infection and disease. Using modern laboratory techniques, scientists can produce BRMs in large amounts for use in cancer treatment.
In some cases, biological therapy given after surgery can help prevent melanoma from recurring. For patients with metastatic melanoma or a high risk of recurrence, interferon-alfa and interleukin-2 may be recommended after surgery. Colony-stimulating factors and tumor vaccines are examples of other BRMs under study.
Radiation Therapy
In some cases, radiation therapy, also called radiotherapy, is used to relieve some of the symptoms caused by melanoma. Radiation therapy is the use of high-energy rays to kill cancer cells. Radiation therapy is a local therapy that affects cells only in the treated area. Radiation therapy is most commonly used to help control melanoma that has spread to the brain or bones, and other parts of the body.
Surgery
When the melanoma is very thin, the biopsy may remove all the cancerous tissue and no additional surgery may be necessary. For thick melanomas, it may be necessary to take out a larger margin of tissue. Deeper melanomas have a higher chance of spreading to the lymph nodes. For these cases, a sentinel lymph node biopsy may be performed to determine if the cancer has spread.
Surgery alone may not effectively control melanoma that has spread to other parts of the body. Your doctor may use other methods of treatment, such as chemotherapy, biological therapy or immunotherapy, radiation therapy or a combination of these methods.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
More treatment info
-
Hyperthermia (HT)
Heat is used to kill small cancer tumors and to enhance the effectiveness of radiation and chemotherapy.
Learn more -
Mohs Micrographic Surgery
A specialized technique to treat complex skin cancers has the highest rate of recovery while removing the smallest amount of healthy tissue.
Learn more
Recommended reading
Where to get care (2)
Related clinics (4)

Osher Center for Integrative Health
 2
2