Infertility in Men
On this page
Overview
As with female reproduction, male reproduction is hormonally driven, requiring a normally functioning hypothalamus and pituitary gland. As in women, gonadotropin releasing hormone, or GnRH, is released in a pulsatile fashion, stimulating the release of follicle stimulating hormone (FSH) and leutinizing hormone (LH). In men, LH primarily stimulates testosterone production, while FSH stimulates the production of sperm. The testes must be capable of response to this hormonal stimulus. In addition, there must be an intact ductal system to transport sperm to the urethra.
The male external genitals consist of the scrotum, which houses the testes and associated ductal systems (the epididymis and vas deferens), and the penis. The testes are covered by a tough fibrous layer called the tunica albuginea, which divides the testes into lobules. Each of the 200 to 300 lobules contains one to three long and tightly coiled seminiferous tubules, within which sperm production occurs.
In contrast to female eggs, sperm are continually produced throughout a man's lifetime. During spermatogenesis and transport through the male reproductive tract, the male spermatozoa are transformed into a highly specialized cell with its own motility and enzymatic capacity to penetrate the egg. Epididymal function must be normal and the accessory glands must be functional to produce normal seminal plasma. An intact nervous system is also required to permit penile erection and normal ejaculation.
Our Approach to Infertility in Men
UCSF is a leader in reproductive health, achieving consistently high pregnancy rates, and we offer a comprehensive array of evaluation and treatment options for men with fertility concerns. We recognize that the process of resolving infertility can be difficult, and we are committed to caring for each patient with knowledge, understanding and respect.
Treatment for male infertility depends on the underlying condition. Anatomical problems can often be addressed effectively with surgery. Medications can be used to treat certain disorders or to enhance sperm production. If neither surgical nor medical therapy is appropriate, we offer the latest assisted reproductive technologies. These include sperm extraction procedures and intracytoplasmic sperm injection, a revolutionary technique developed at UCSF that has helped many couples with male fertility problems achieve pregnancy.
Causes
Male infertility can be divided into:
- Problems with ejaculation or erection
- Problems within the fine, small reproductive tract ducts
- Problems with sperm production
Problems with sperm production is by far the most common of the three, and can be detected during semen analysis. There are many causes of abnormal sperm production, including:
- Varicocele (varicose veins)
- Genetic problems
- Infections
- Exposures to heat or toxic chemicals
- Drugs and medications
- Hormonal imbalance
Ejaculation Failure (Anejaculation)
Ejaculatory failure is the inability to ejaculate. It has a variety of causes, including pelvic nerve damage from diabetes mellitus, multiple sclerosis or abdominal-pelvic surgery and spinal cord injury.
It is important to distinguish ejaculatory failure from the inability to achieve an erection, premature ejaculation and retrograde ejaculation (ejaculating into the bladder and not into the penis).
Rectal probe electroejaculation is a commonly performed technique that may enable patients to produce an ejaculate capable of achieving a pregnancy. With rectal probe, the doctor electrically stimulates the pelvic sympathetic nerves to induce a reflex ejaculation from which semen is collected.
Ejaculatory Duct Obstruction
Ejaculatory duct obstruction is diagnosed in approximately 10 percent of men without sperm in the ejaculate. Usually caused by stones, cysts or scar tissue blocking the prostate ducts, the condition is treated with a simple outpatient procedure that involves removing portions of the ducts. Significant improvements in semen quality occur in 70 percent of patients, which are associated with a 20 percent to 30 percent pregnancy rate.
Varicocele
The varicocele is defined as dilated and twisted veins within the scrotum, similar to varicose veins in the legs, and is basically a consequence of upright posture. A varicocele can be found in 42 percent of infertile men and has an unquestioned statistical association with infertility. However, 15 percent of normal, fertile men also have a varicocele.
Varicocele surgery to bind off the twisted veins will improve semen quality in roughly 67 percent of patients, with improvement most likely to be an increase in the sperms' ability to move spontaneously rather than sperm quantity. The pregnancy rate following varicocele repair is approximately 40 percent, with pregnancy occurring an average of nine months after surgery.
The varicocele remains the most correctable factor when poor semen quality is discovered, but since it is very common, the operation should be considered only if other infertility risk factors are absent.
Environment, Lifestyle and Fertility
Over the last several decades, concern has risen about the impact of industrialization on reproductive health. This concern stems largely from reports showing that semen quality of men in Europe and the United States has decreased over the latter half of the 20th century.
The environmental toxins most often cited as potential contributors to infertility can be organized into physical, chemical, occupational and lifestyle factors:
- Physical Factors Hyperthermia (increased temperature), radiation and electromagnetic fields, for example, are several physical factors that have been linked to infertility in men.
- Chemical Factors Cigarette smoking, excessive alcohol consumption, marijuana and cocaine use as well as caffeine intake may contribute to chemical causes of infertility.
- Occupational Factors Occupational hazards such as some pesticides, industrial toxins like dioxin and polychlorinated biphenyls (PCBs), and exposure to heavy metals also may be linked to infertility.
- Lifestyle Factors Finally, stress, nutrition and other lifestyle factors also can play a role.
Diagnosis
An initial male fertility examination includes a medical history, physical examination, general hormone tests and one or more semen analyses, which measure semen volume as well as sperm number, ability to move spontaneously and quality of motion.
Medical History
Initial questions may include:
- A review of past medical history, prior surgeries and medications used
- A discussion of family history of infertility or birth defects
- A careful review of social history and occupational hazards to evaluate potential exposure to hazardous substances that could impact fertility
Physical Exam
Next, you will receive a thorough physical examination to evaluate the pelvic organs — the penis, testes, prostate and scrotum.
Laboratory Tests
Laboratory tests may include:
- Urinalysis These can indicate the presence of an infection.
- Semen Evaluation The evaluation assesses sperm motility or movement, the shape and maturity of the sperm, the volume of the ejaculate, the actual sperm count and the liquidity of the ejaculate.
- Hormonal Tests Hormonal tests evaluate levels of testosterone and FSH (follicle-stimulating hormone) to determine the overall balance of the hormonal system and specific state of sperm production. Serum LH and prolactin are other hormonal tests that may be done if initial testing indicates the need for them.
If a diagnosis is not obvious after the initial evaluation, further testing may be required. One or more of the following tests may be recommended:
- Seminal Fructose Test To identify if fructose is being added properly to the semen by the seminal vesicles
- Post-ejaculate Urinalysis To determine if obstruction or retrograde ejaculation exists
- Semen Leukocyte Analysis To identify if there are white blood cells in the semen
- Kruger and World Health Organization (WHO) Morphology To examine sperm shape and features more closely
- Anti-sperm Antibodies Test To identify the presence of antibodies that may contribute to infertility
- Sperm Penetration Assay (SPA) To confirm the sperm's ability to fertilize
- Ultrasound To detect varicoceles (varicose veins) or duct obstructions in the prostate, scrotum, seminal vesicles and ejaculatory ducts
- Testicular Biopsy To determine if sperm production is impaired or a blockage exists
- Vasography To check the structure of the duct system and identify any obstructions
- Genetic Testing To rule out underlying mutations in one or more gene regions of the Y chromosome, or to test for cystic fibrosis in men missing the vas deferens
After the diagnostic evaluation is completed, treatment may involve medical or endocrinologic treatment, surgical correction or a decision to manipulate or process sperm to achieve a pregnancy.
Treatments
Any fertility treatment may be expected to have an effect on semen quality roughly three months after it is started, as this is the length of time required for a single cycle of spermatogenesis, or sperm production. If neither surgical nor medical therapy is appropriate, assisted reproductive technologies are possible.
In choosing a treatment plan, consideration should be given to each couple's long-term goals, financial constraints, and the results of the female partner's evaluation in addition to male factor findings.
Specific Therapy
The most successful medical therapy for male infertility involves reversing chemical, infectious or endocrine imbalances. This is called specific therapy, and it is usually successful because treatment is based on the correction of well-defined problems.
Examples of this include:
- Treatment for acute prostatitis, epididymitis or varicocele
- The replacement of the pituitary hormones — follicle stimulating hormone (FSH) and leutinizing hormone (LH) — for radiation or surgically induced pituitary disease
- The administration of testosterone in men with hypoandrogenic hypogonadism
Empiric Therapy
Another kind of treatment, called empiric therapy, attempts to correct rather ill-defined conditions. The use of clomiphene citrate, tamoxifen or ProXeed for low sperm density or motility are examples of this form of therapy.
These treatments often have limited success because the generally intact mechanisms within the body tend to counteract the intended effect. In other words, hormonal treatments based on the principle that "if some hormone is good, then more is better" are destined to failure and should be avoided.
Assisted Reproductive Technology
Treating specific illnesses may or may not treat the fertility problem. At least 10 percent of infertility problems are due to unknown causes and another 30 percent are due to problems in both the male and female partners.
In addition to medication and surgical infertility treatments to treat specific health conditions in men and women, a new class of treatments — called assisted reproductive technologies, or ART — has been developed. The most common ART is in vitro fertilization, or IVF, but new procedures can enhance the IVF process or address other infertility conditions. These procedures for men include:
- Intracytoplasmic sperm injection (ICSI)
- Vasal aspiration
- Epididymal aspiration
- Testicular sperm extraction
- "Mapping" the failing testes
- Ovum donors and embryo or semen freezing
Intracytoplasmic Sperm Injection (ICSI)
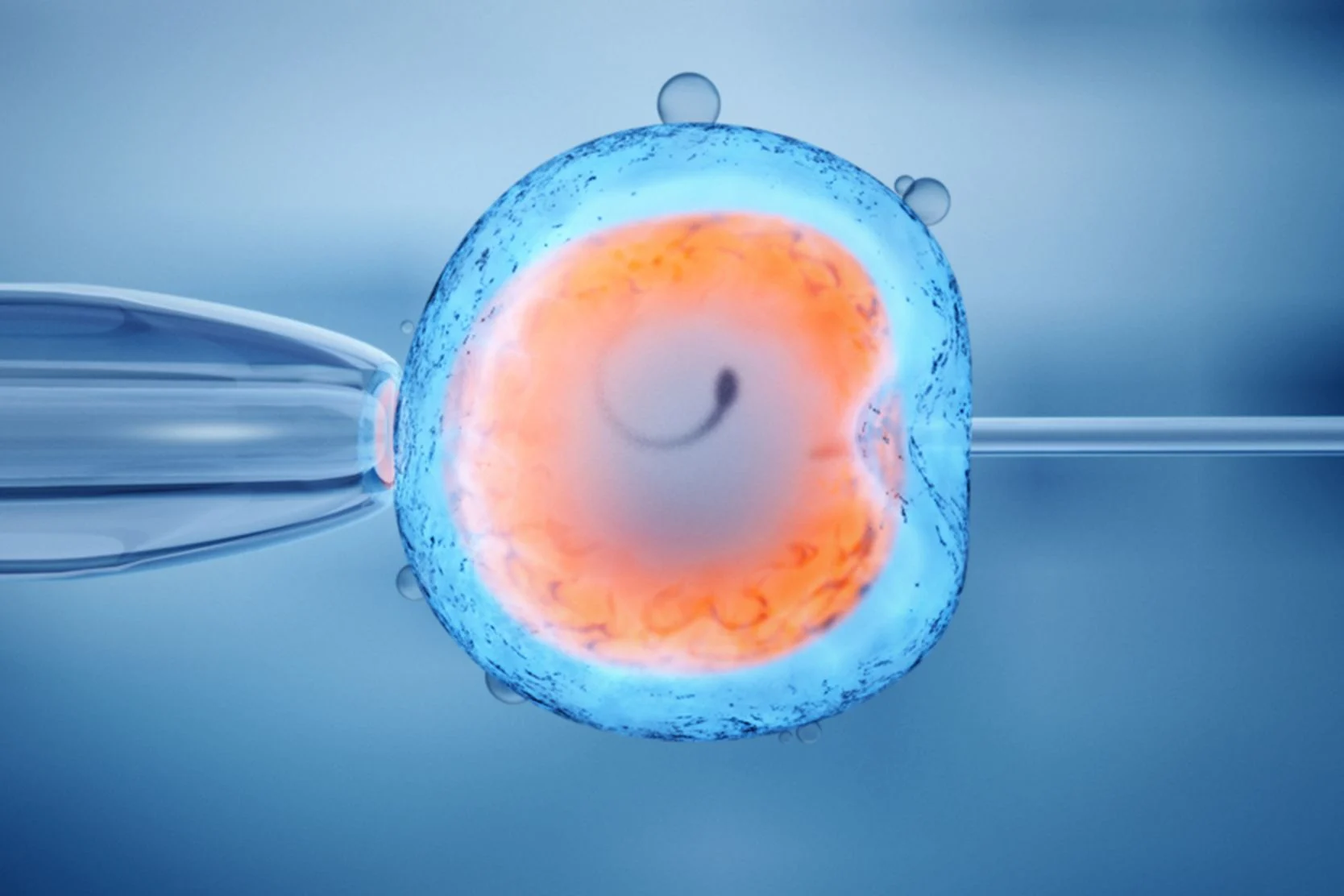
Intracytoplasmic sperm injection, or ICSI, is a technique developed to help achieve fertilization for couples with severe male factor infertility or couples who have had failure to fertilize in a previous in vitro fertilization attempt. The procedure overcomes many of the barriers to fertilization and allows couples with little hope of achieving successful pregnancy to obtain fertilized embryos.
The procedure was first used at UCSF Medical Center in 1994 and the first successful birth achieved with ICSI assistance was in February 1995. UCSF Medical Center was the first San Francisco Bay Area program to achieve a pregnancy and birth with this "miracle" procedure.
The technique involves very precise maneuvers to pick up a single live sperm and inject it directly into the center of a human egg. The procedure requires that the female partner undergo ovarian stimulation with fertility medications so that several mature eggs develop. These eggs are then suctioned through the vagina, using vaginal ultrasound, and incubated under precise conditions in the embryology laboratory. The semen sample is prepared by spinning the sperm cells through a special medium. This solution separates live sperm from debris and most of the dead sperm. The specialist picks up the single live sperm in a glass needle and injects it directly into the egg.
Through the ICSI procedure, many couples with difficult male factor infertility problems have achieved pregnancy. Fertilization rates of 70 percent to 80 percent of all eggs injected are currently being achieved, and pregnancy rates are comparable to those seen with IVF in couples with no male factor infertility.
Please read FAQ: Intracytoplasmic Sperm Injection for more information about this procedure.
Sperm Extraction Procedures
Intracytoplasmic sperm injection has revolutionized the treatment of male infertility. The sperm requirement for egg fertilization has dropped from hundreds of thousands for in vitro fertilization (IVF), to one viable sperm required for ICSI when combined with IVF.
This has led to the recent development of aggressive new surgical techniques to provide viable sperm for egg fertilization from men with low or no sperm count. This also has pushed urologists beyond the ejaculate and into the male reproductive tract to find sperm. Presently, sources of sperm in otherwise azoospermic patients, or those with no ejaculated sperm, include the vas deferens, epididymis and testicle, using sperm aspiration techniques in which the sperm is suctioned from the organ.
Sperm aspiration techniques involve the use of minor surgical procedures to collect sperm from organs within the genital tract. These techniques are indicated for men in whom the transport of sperm is not possible because the ductal system that normally carries sperm to the ejaculate is absent, such as with the congenital absence of the vas deferens, or unable to be reconstructed.
Most recently, sperm has been fairly reliably extracted — 60 percent to 70 percent of the time — from the testes of men with sperm production problems of such severity that no sperm is found in the ejaculatory ducts.
It is important to realize, however, that IVF technology is required to achieve a pregnancy with the vast majority of these extraction procedures, and success rates are intimately tied to a complex and complementary program of assisted reproduction for both partners.
Sperm Extraction: Vasal Aspiration
Patients who have congenital or acquired obstruction of the ductal system at the level of the prostate or in the abdominal or pelvic portions of the vas deferens may be candidates for this technique. Patients who have undergone a vasectomy less than five years before also may be candidates.
Vasal aspiration is a brief, same-day operation under local anesthesia. It can be done through a small scrotal incision or through incisionless techniques. Either way, the vas deferens is entered and a syringe is used to suction leaking sperm into a nourishing fluid. More sperm are brought to the opening by gently massaging the epididymis and vas deferens. The recovery period is 24 hours. Aspirated sperm are specially processed and prepared for insemination or IVF.
Of the three extraction procedures, vasal aspiration provides the most "mature" sperm, as they have already passed through the epididymis, where maturation processes occur during normal sperm development. Often, ICSI is not required to achieve a pregnancy. A big benefit of vasal sperm is that it is basically equivalent to ejaculated sperm and thus it can be frozen at the time of surgery to avoid further procedures in the male.
Sperm Extraction: Epididymal Aspiration
Epididymal sperm aspiration can be performed in situations in which the vas deferens is either absent or is scarred from prior surgery, trauma or infection. Sperm are directly collected from a single, isolated epididymal tubule (MESA) or by blind needle puncture (PESA) in much the same manner as the vasal procedure. Depending on the length of the epididymis that is available for aspiration, multiple, separate aspiration attempts can be made from one or both testicles.
When 10 to 20 million sperm are obtained, the sperm are processed for fertilization of the partner's eggs. Epididymal sperm are not as "mature" as sperm that have traversed the entire length of the epididymis and reside in the vas deferens and, as a consequence, epididymal sperm require ICSI to fertilize eggs.
Egg fertilization rates of 60 percent to 80 percent and pregnancy rates of approximately 45 percent to 55 percent have been reported with epididymal sperm. Obviously, the results will vary among individuals because of differences in sperm and egg quality as well as the technical proficiency of the lab. Like vasal sperm, these sperm can be frozen at the time of surgery to eliminate future surgical sperm retrieval procedures.
Sperm Extraction: Testicular Sperm Extraction (TESE); Testicular Sperm Aspiration (TESA)
The newest of the aspiration techniques is testicular sperm retrieval. In this procedure, a small amount of testis tissue is taken by biopsy under local anesthesia. It is a breakthrough in that it demonstrates that sperm do not have to "mature" and pass through the epididymis in order to fertilize an egg. Because of their immaturity, however, testicular sperm need ICSI.
Testicular sperm extraction is indicated for patients in whom there is a blockage in the epididymis very near the testis that is either from prior surgery, infection or from birth, or a blockage within the ducts of the testes, called efferent ductules.
It also is used for men with extremely poor sperm production, in which so few sperm are produced that they cannot reach the ejaculate. Pregnancies are now routine in cases of poor sperm production, but there is some concern with the use of this sperm because in most cases the underlying condition causing the poor sperm production is still unknown. Therefore, in these cases, it must be realized that the condition which may have caused the infertility may be transmitted to the progeny.
Recently, even spermatids — round cells that eventually becomes sperm with tails — have been used to achieve pregnancies with ICSI. However, this has raised much speculation and concern about the use of genetic material from a still-evolving germ cell for clinical purposes before the system has been appropriately investigated and its genetic stability examined in animal models. Spermatid injections are currently considered experimental procedures.
One drawback of testis sperm is that is does not freeze as readily as epididymal or vasal sperm, so it is more likely that the male partner will need to undergo repeated procedures for each IVF attempt.
Sperm Extraction: "Mapping" the Failing Testes
First proposed in 1997, this concept addressed the issue of how to detect where ICSI-compatible, mature sperm exist within failing or atrophic testes. It was based on prior observations that sperm production can be "patchy" or "focal" within the failing testis. This led to the idea that the more sites that are sampled within the testis to look for sperm, the higher the chances of usable sperm.
Information derived from "mapping" can be used as follows:
- To help infertile couples decide whether or not to proceed to IVF and ICSI
- To locate and find sperm for ICSI within atrophic testes
Awards & recognition

Best in Northern California for urology
#1
in NIH funding for urology research
Recommended reading
More treatment info
Related services & treatments
Specialties
Treatments
- In Vitro Fertilization
- Testicular Biopsy
- Male Genitourinary Reconstruction
- Intrauterine Insemination
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.