Liver Transplant
On this page
Liver Transplant
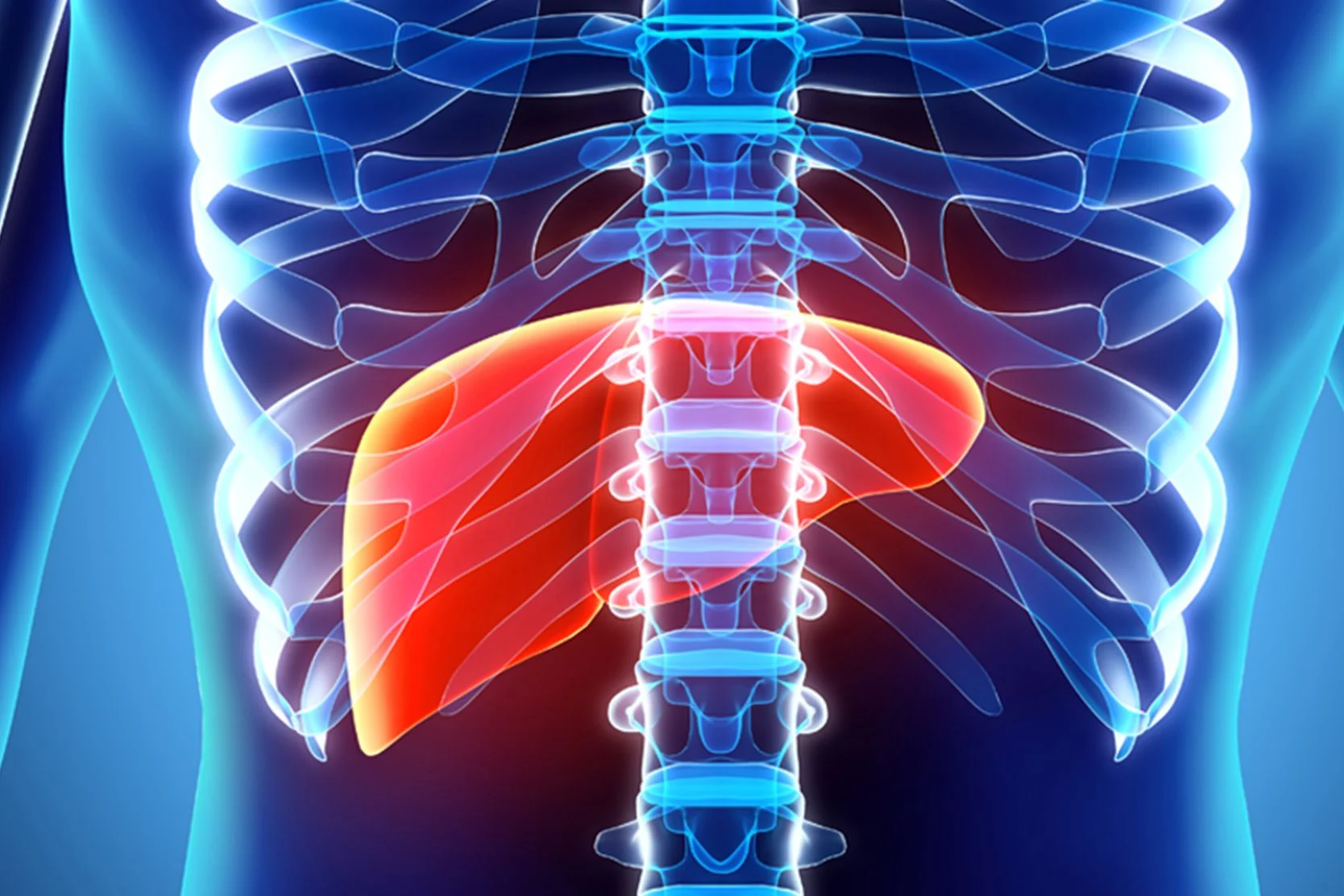
The liver is the largest organ in the body. It's located in the upper right portion of the abdomen, on top of the stomach. Its many functions include:
- Processing proteins, fats and carbohydrates
- Breaking down toxic substances such as drugs and alcohol
- Making the chemical components that help your blood clot
- Excreting a yellow digestive juice called bile
If your liver stops working properly, you lose the ability to clot blood after an injury and to process the nutrients needed for life. Bile may accumulate, causing jaundiced (yellow) eyes and itchy skin.
Certain medications help treat liver failure symptoms, but there are no drugs that can cure it. Successful liver transplantation offers people with end-stage liver failure the chance to lead a longer, more active life.
Eligibility
A liver transplant may not be recommended if you have an infection outside the liver, a medical condition that poses a problem or if you are an active substance abuser. Please contact us for more information on UCSF Health's policy regarding liver transplants for patients with alcoholic liver disease.
Patients with a history of drug or alcohol dependency must remain drug- and alcohol-free for six months before transplant and agree to random screening tests.
People with certain types of cancer, such as metastatic carcinoma or cholangiocarcinoma (cancer of the bile ducts), or specific heart or lung conditions aren't candidates for liver transplantation.
Evaluation
The preliminary evaluation, called a phase I evaluation, is the first step in determining if transplantation is an appropriate treatment option for you. During the evaluation, the transplant team also assesses the medical factors related to your liver failure.
The appointment takes a full day, from about 7 a.m. to 4 p.m., and can be very tiring. We ask that you bring at least one family member or other support person to help you process the significant amount of information you'll receive about the transplant process.
To prepare for the tests you'll undergo, do not eat or drink anything after midnight the day before your appointment. Please bring these items to your appointment:
- A snack
- Any medications you take
- Two forms of identification
- Your health insurance information
- Your medical records if you have them
Tests
You'll undergo a series of tests during your evaluation, including:
- Blood tests to determine how well your liver and kidneys are working
- Ultrasound scan to view the blood flow to and from your liver and to look for any abnormal masses in the liver
- Chest X-ray to look for lung infection and to assess the status of your bones
- Electrocardiogram to look for any changes in your heart rhythm
- Pulmonary function test to measure your lung capacity
You'll also be evaluated by a liver specialist, called a hepatologist, and a surgeon. The hepatologist will perform a full exam, review your health history and discuss the transplantation process.
You can discuss your test results with the hepatologist and surgeon and ask any questions you have. Many patients find it helpful to write down a list of questions before the appointment.
You will also meet with a financial counselor to review your insurance information.
Living and deceased donors
Liver transplantation can be performed using a portion of liver taken from either a deceased or a living donor. After a living donor liver transplant, both the donor's remaining liver lobe and the transplanted lobe grow to full size.
Living donors allow patients to receive a transplant without the sometimes lengthy wait for a liver from a deceased donor to become available.
During the transplant evaluation, living donor transplantation will be discussed. Donors must be in good health, have a compatible blood type and want to donate for altruistic reasons. If you have a potential living donor, their evaluation will begin after you've completed all your testing. If the transplant team determines that the donation would work, a surgery date will be scheduled for both you and your donor. This process takes up to six months.
If you will receive a liver from a deceased donor, you'll be placed on a national waiting list until an organ becomes available. This can occur at any time, day or night. The wait for a new liver can take up to three years and you may need to repeat certain tests before your transplant.
If a liver transplant isn't in your best interest, a transplant team member will call you to discuss other options.
Social work support
Before your operation, a social worker will talk to you to about adjusting after the surgery. Social workers lead weekly support groups for current and former transplant recipients and their families to address a wide range of issues, and one-on-one counseling is also available during your hospital stay. If needed, a social worker can arrange follow-up services and answer questions about disability.
Procedure
Liver transplant surgery lasts about four to 12 hours depending on the patient's condition. Surgery often takes longer if the patient's had previous surgeries, due to scar tissue.
During surgery, your damaged liver and gallbladder will be removed and replaced with the donor liver. Your gallbladder isn't necessary and won't be replaced.
Recovery
After the transplant, you will be taken directly to the intensive care unit (ICU). Most patients need only a brief stay in the ICU.
During surgery, a breathing tube is inserted to help you breathe. In most cases the tube can be removed shortly after surgery. Many monitoring lines are attached during surgery; these, too, will be removed as you become more stable. When you're ready to leave the ICU, you will be cared for in our transplant unit.
Everyone recuperates from liver transplantation differently. Patients typically spend five to 10 days in the hospital. The length of your stay will depend on a number of factors, including how sick you are at the time of transplant, the complexity of your operation and if you experience any complications.
You should have a caregiver available both during your hospital stay and after discharge until you recover.
Follow-up care
Once you're discharged from the hospital, you'll initially have weekly follow-up visits at the Liver Transplant Clinic. As you recover, you'll need to be seen less frequently. If you live outside the San Francisco area, you'll likely need to find temporary lodging close to UCSF for the first month after discharge.
You'll have blood tests twice a week following transplantation. Gradually, these will become less frequent.
You'll be notified about any adjustments you need to make to your medications.
Complications and risks
Complications can occur with any surgery, and patients who've had an organ transplant may face additional risks. Possible complications of a liver transplant include:
- Hemorrhage
One of the liver's jobs is to make clotting factors that help stop bleeding after an injury. When the liver fails, the ability to produce clotting factors is impaired. To correct this problem, you'll receive blood products before and after surgery. It is expected that your new liver will start working very quickly to help prevent any excessive bleeding, but it is possible that you may be returned to surgery to control the bleeding, particularly if it occurs within 48 hours after the transplant. - Thrombosis
If a blood clot forms in a vessel leading to or from your liver, it can injure your new liver. This is a serious complication that may require a second transplant. You may receive special anticoagulation medication to prevent thrombosis. - Rejection
Your body's immune system protects you from invading organisms. Unfortunately, it also views your new liver as foreign and will try to destroy it to protect you. This is known as rejection. To prevent this, you must take special immunosuppressive medication for the rest of your life. - Recurrent disease
Some liver diseases can come back after a transplant. Your provider will discuss this with you if it's relevant to your case.
Immunosuppressive medications
Immunosuppressive medications, also known as anti-rejection medications, help prevent and treat rejection. You will need to take these medications for the rest of your life. Immediately after surgery, the dosages will be high since the probability of rejection is greatest at this time. We will lower your dosage quickly if there are no signs of rejection.
These medications have side effects, some of which are dose-related. Patients typically experience the most side effects right after transplantation, when the dosage is highest. As your dosage is lowered, the side effects will probably lessen. Side effects may occur in some patients and not in others.
Be aware that anti-rejection medications also impair your body's ability to fight off infections. You'll be given medication to help prevent infections, but you'll need to use caution and avoid contact with people with infections, especially during the first three to six months after transplant.
Recommended reading
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.