Diabetes in Pregnancy
Gestational diabetes refers to diabetes that is diagnosed during pregnancy. Gestational diabetes occurs in about 7 percent of all pregnancies, usually in the second half of the pregnancy. It almost always goes away as soon as your baby is born. However, if gestational diabetes is not treated during your pregnancy, you may experience some complications.
Causes
Pregnancy hormones cause the body to be resistant to the action of insulin, a hormone made by your pancreas that helps your body use the fuels supplied by food.
The carbohydrates you eat provide your body with a fuel called glucose, the sugar in the blood that nourishes your brain, heart, tissues and muscles. Glucose is also an important fuel for your developing baby. In gestational diabetes, insulin fails to effectively move glucose into the cells that need it. As a result, glucose accumulates in the blood, causing blood sugar levels to rise.
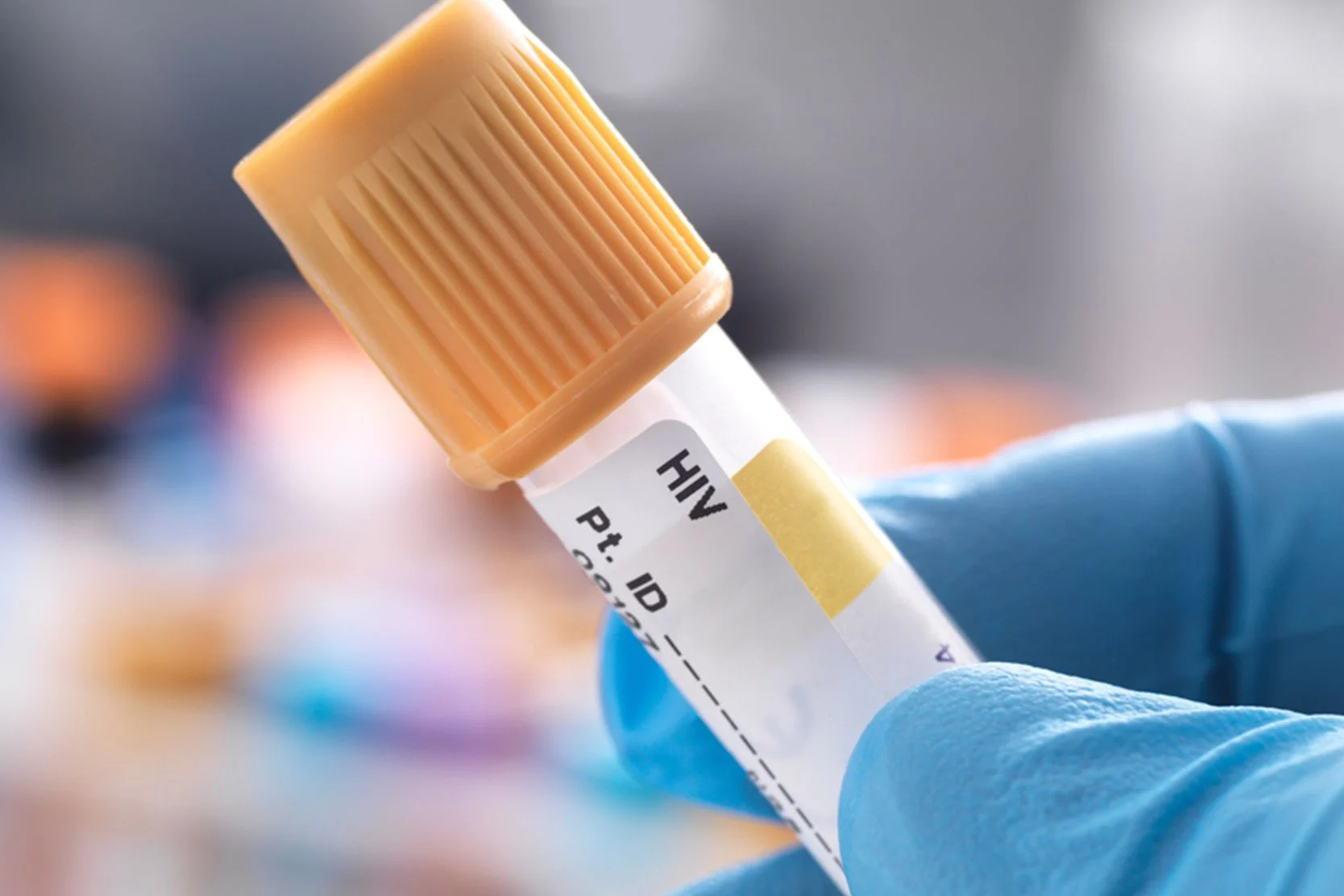
Diagnosis
Gestational diabetes is diagnosed with a blood test. Your blood glucose level is measured after you drink a sweet beverage. If your blood sugar is too high, you have gestational diabetes. Sometimes one test is all that's needed to make a definitive diagnosis. More often, an initial screening test is done, followed by a longer evaluation.
Gestational diabetes usually usually doesn't happen until later in pregnancy, when the placenta is producing more of the hormones that interfere with the mother's insulin. Screening for gestational diabetes usually takes place at 24 to 28 weeks, but women at high risk are likely to be screened in the first trimester.
Risk Factors
A number of risk factors are associated with gestational diabetes, including:
- Being overweight
- Giving birth to a baby that weighed more than 9 pounds
- Having a parent or sibling with diabetes
- Having had gestational diabetes in the past
- Having glucose in your urine
In addition, gestational diabetes occurs more often in African Americans, Native Americans, Latinas and women with a family history of diabetes.
Gestational Diabetes and Your Baby
Gestational diabetes can affect your developing baby in a couple of ways:
- High birth weight Exposure to higher sugar levels from the maternal bloodstream can result in a larger baby and a high birth weight. The baby's pancreas produces extra insulin in response to the higher glucose, which results in the baby storing extra fat and growing larger. A larger baby can make delivery more complicated for both mother and baby.
- Low blood sugar If your blood sugar has been elevated during the pregnancy, your baby may have low blood sugar, called hypoglycemia, shortly after birth. The extra insulin that your baby produces when your blood sugar is high continues to bring their blood sugar down for a short time after birth. Without the continued supply of sugar from maternal blood, your baby's blood sugar level may fall too low.
This is temporary, though, and the nurses and doctors caring for your newborn will monitor your baby carefully and treat any episodes of low blood sugar that may occur.
Avoiding Complications
The complications of gestational diabetes can be prevented by keeping your blood sugar under control during your pregnancy. The goal of treatment is to keep your blood sugar in the normal range. Most women with well-controlled blood sugar deliver healthy babies without any complications.
Treatment
Diet
The first step in treating gestational diabetes is to modify your diet to help keep your blood sugar level in the normal range. It's a good idea to meet with a registered dietitian to develop a customized eating plan to help you manage your blood sugar. You can also read up on Dietary Recommendations for Gestational Diabetes.
The main dietary principles:
- Avoid high-sugar foods. For the remainder of your pregnancy, avoid desserts, sweets, candy, cookies, soft drinks and fruit juice. You should eat fruit, but because fruit is high in natural sugar, limit it to one small serving at a time.
- Eat reasonable portions of high-carbohydrate foods. Carbohydrates are found in breads, cereals, rice, pasta, potatoes, beans, fruits, milk, yogurt and some vegetables. Carbohydrate foods break down into glucose during digestion. They are important because they contain nutrients that are necessary for both you and your developing baby. It's important to eat carbohydrate foods at each meal, but don't overeat.
- Eat smaller, more frequent meals. Space out the carbohydrate foods you consume throughout the day. Cutting down on the portion size of carbohydrate foods eaten at one sitting means that you need to eat more often to meet your pregnancy nutrient needs. Eating three smaller meals and three or four snacks between meals can help you meet your pregnancy diet goals without elevating your blood sugar.
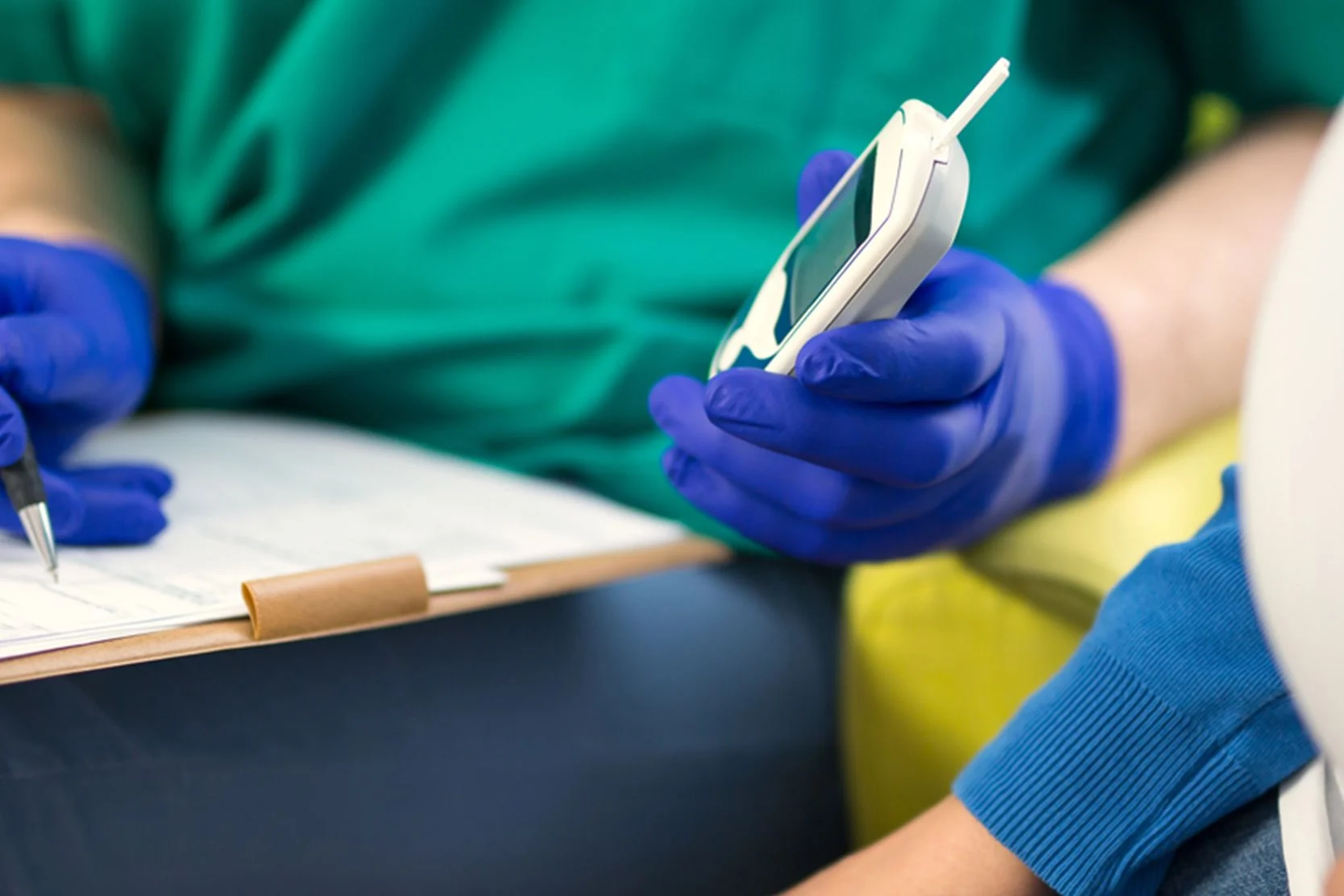
Blood Sugar Monitoring
The only way to know that your gestational diabetes is being properly controlled is to check your blood sugar frequently. You'll be instructed on the use of a home blood sugar monitor. You should check your blood sugar at least four times a day, or as directed by your doctor. Check your fasting blood sugar first thing in the morning, before having anything to eat or drink. Also check your blood sugar one hour after starting to eat your three main meals: breakfast, lunch and dinner. Check with your doctor for target blood sugar levels.
Other Treatments
Most women with gestational diabetes are able to control their blood sugar simply by modifying their diet. You'll need to follow the diet guidelines until your baby is born. After delivery, most women are able to resume their normal eating habits. Gestational diabetes does not interfere with your ability to breastfeed your baby.
For about 30 percent of women who develop gestational diabetes, following a diet is not enough to control their blood sugar, and they need to take insulin. Insulin is safe during pregnancy. If you're taking insulin, you'll still need to continue with the prescribed diet and monitor your blood sugar levels.
After Delivery
After your baby is born, your blood sugar will be checked to make sure it's normal. Fortunately, gestational diabetes almost always goes away after your baby is born. If your blood sugar doesn't return to normal, it may mean that you had diabetes before you became pregnant.
The most important thing to remember is to check your blood sugar before getting pregnant again. Women who've had gestational diabetes have a higher risk of developing type 2 diabetes. Women who had diabetes before getting pregnant have a higher risk of pregnancy complications. Elevated maternal blood sugar during the first 12 weeks of pregnancy, when the major organ systems are developing, increases risks to the fetus. Women with diabetes can help improve their chances of having a healthy baby by normalizing their blood sugar before pregnancy.
Recommended reading
Support services

Great Expectations Pregnancy Classes
Get ready for the baby! Choose from a variety of classes that prepare moms and partners for pregnancy, birth, baby care, breastfeeding and parenting.
Lactation Consultant Support
Get support for all your breastfeeding needs. Troubleshoot with a lactation consultant, find equipment and supplies, join a support group and more.
Women's Health Resource Center
Access free health resources here, from classes and webinars to support groups and medical referrals, plus pregnancy, birth and breastfeeding services.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.