Ventricular Assist Device (VAD)
On this page
Ventricular Assist Device (VAD)
What is a ventricular assist device (VAD)?
A ventricular assist device (VAD) is a mechanical pump that helps the heart function in patients with severe heart failure. It can serve as either a temporary or permanent support for your heart and often acts as a bridge for patients waiting for a heart transplant.
A VAD is implanted into the chest using open heart surgery. Once implanted, it pumps blood from the heart's lower chambers to the rest of the body. This pumping reduces your heart's workload, which can help prolong your life and improve symptoms like fatigue and breathlessness.
In some cases, the VAD may help return the heart to its normal functions. If this happens, the device can be removed.
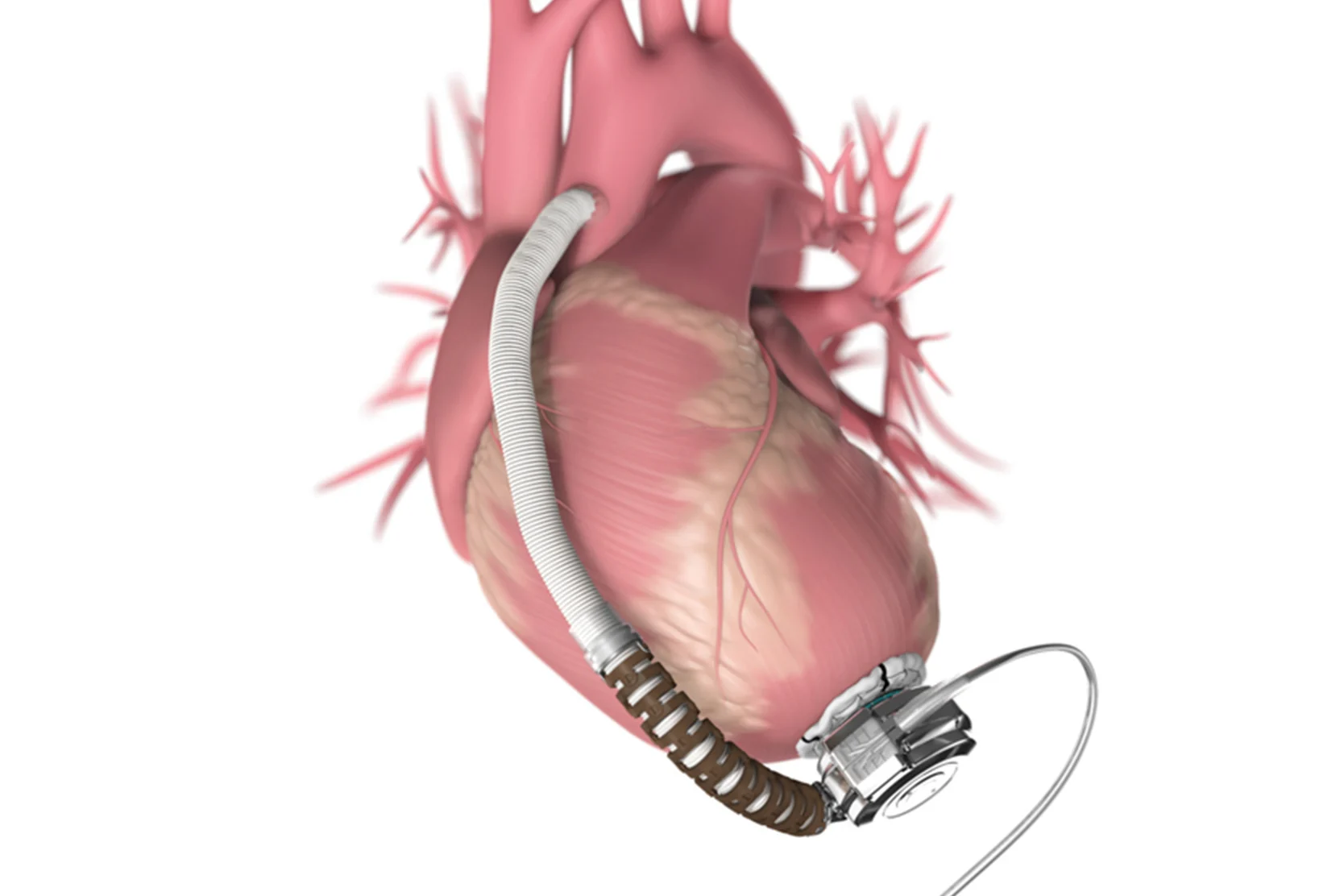
All VADs consist of several parts. A small tube is connected to the heart and carries blood to the pump, which may be worn outside the body or implanted in the abdomen or chest. Another tube carries blood from the pump back to your aorta, the main artery in the body. There's also a control system and a battery pack, which are worn outside the body. The VAD's external parts are connected to the internal parts via a tube through the side of your abdomen.
Our approach to ventricular assist devices (VAD)
UCSF uses several different types of ventricular assist devices (VAD). The most common type, known as an LVAD, supports the left ventricle of the heart. Other types support the right ventricle (known as an RVAD) or both chambers (a biventricular assist device, or BiVAD). Our team will determine the best option for your specific situation.Evaluation for a VAD
Our team will evaluate your case to determine if you might benefit from a ventricular assist device (VAD).
During the evaluation we will discuss the various types of VADs, and which is best for your condition. We'll also answer any questions you have about the device and the implantation procedure.
Your doctor may recommend a VAD if:
- You're waiting for a heart transplant. The VAD will be implanted temporarily, and you can return home while you wait for a donor heart to become available. When you receive your new heart, the VAD will be removed. This temporary use of a VAD is called bridge therapy.
- You're not a good candidate for a heart transplant. A VAD can be a long-term solution to help your heart function when medication isn't helping, but you're not eligible for a transplant. In this case, the VAD is permanently implanted, which can significantly improve your quality of life. This treatment is known as destination therapy.
- Your heart's function can become normal again. If you're recovering from heart surgery or a heart attack, a VAD can help your heart rest while you heal. It is removed once your heart is healthy enough to pump blood on its own again. In this case, you may only need the VAD for a few weeks or months.
Risks of a VAD
VADs do come with risks, including the risks associated with any major surgery, as well as the risk of stroke, bleeding or infection at the incision or in the heart. There's also an ongoing risk of infection at the wound site where tubing connects the internal pump to the external power source.
Procedure for a VAD
Before getting a ventricular assist device, you will undergo tests to assess the function of your heart and your overall condition. These tests ensure you are healthy enough to have the surgery.
These tests may include:
- Blood tests. During these tests, blood is drawn from your arm. You may need to fast for 12 hours prior to having blood tests.
- Chest x-ray. This test checks for calcium deposits and gives information about the size and shape of the heart and lungs.
- Echocardiogram. This test uses sound waves to produce pictures of your heart that can then be diagnosed.
- Electrocardiogram (EKG). This test records electrical activity in your heart and registers any irregularities. You may be asked to wear a portable EKG device that monitors your heart 24 hours a day for up to 14 days.
- Cardiac catheterization. This procedure involves threading a thin tube into the heart to gather information on its function.
Surgery for a VAD
Implanting the VAD requires open-heart surgery under general anesthesia. You will be asleep for the procedure and won't feel anything. The surgery takes about four to six hours. Afterward, you will be transferred to the intensive care unit for recovery. You will be on a respirator, or breathing machine, until you're awake and able to breathe on your own.
Maintaining your VAD
During your hospital stay we will teach you and your designated caregiver about the device. This will include giving you instructions for maintaining and protecting it and what to do in case of emergency. By the time you leave the hospital, you and your caregiver will be comfortable with your VAD.
We will also communicate with your primary care doctor and your local emergency services – such as the ambulance service or fire department – to alert them that you have a VAD and to explain what this means for your care.
It's possible to damage your VAD by touching certain electronic equipment, so your health care team will instruct you about handling electronic equipment before you leave the hospital.
Ongoing VAD maintenance and routine
Once you are home, there are things you will need to do to ensure your ventricular assisted device continues to work properly.
- Check it daily. All you need to do is press a button, which will start the device’s self-test. The test takes just a few seconds.
- Change the dressing. Your caregiver will need to change the dressing covering the site where the device exits your body. This takes 15 to 30 minutes.
- Take a blood thinner. Depending on the type of VAD you have, you may need to take a blood thinner medication.
- Take a shower. You can’t swim or take baths after receiving a VAD, but once the exit site has healed, you'll be able to shower using a special covering that protects the device from getting wet.
Help with your VAD
When you're discharged, we will give you contact information for the Mechanical Circulatory Support Program team. If you have any problems with your VAD, you will be able to reach your support person 24 hours a day, seven days a week.
Recommended reading

FAQ: Living with a Ventricular Assist Device (VAD)
Get answers to common questions about living with a ventricular assist device (VAD), including taking medication, daily routines, exercise and more.
What to Expect: Getting a VAD Implanted
Learn how we use minimally invasive techniques to implant ventricular assist devices (VADs) and what to expect after VAD implant surgery.
FAQ: Heart Transplant
Find answers to commonly asked questions about receiving a heart transplant, including waiting list times, surgery expectations and recovery.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
