Mitral Transcatheter Edge-to-Edge Repair (TEER)

On this page
Mitral Transcatheter Edge-to-Edge Repair (TEER)
Updated March 15, 2023
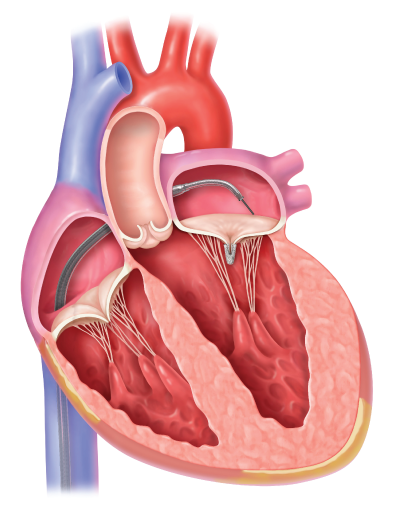
Mitral transcatheter edge-to-edge repair (TEER) is a minimally invasive procedure for treating mitral valve regurgitation, a condition in which the valve between the heart's left chambers doesn't close properly. In a healthy heart, valves open and shut tightly during each heartbeat, controlling blood flow through the heart and out to the rest of the body. When the mitral valve doesn't close well, blood leaks backward and the heart is forced to work harder. Pressure may build in the lungs, and people may feel tired or short of breath.
Without treatment, the regurgitation (backflow) can become more severe over time, with new or worsening symptoms. In TEER, using either the Abbott MitraClip or Pascal Precision system, a small device is implanted in the valve to help it close more fully and restore normal blood flow. These devices work by pulling the valve's flaps into a more natural alignment. They're inserted through an artery by means of a long, thin tube called a catheter, so the procedure requires only a small incision.
TEER can help the heart function better, which can relieve shortness of breath, chest pain and other symptoms, and improve quality of life. Patients commonly feel less anxious, and their risk of future hospitalization for heart failure is reduced.
Evaluation
To assess the condition of your mitral valve and determine whether you are a candidate for TEER, your doctor may request one or more of the following diagnostic tests:
- Coronary angiogram. A catheter is threaded through a blood vessel in your wrist or groin to an artery in your heart, and a harmless dye that shows up well on X-rays is injected into the catheter. The test provides detailed images that reveal how well the coronary arteries are functioning. The cardiac catheterization for this test also allows doctors to measure the pressure inside the heart chambers.
- Echocardiogram. This test uses sound waves to produce detailed images of your heart, allowing doctors to assess the structure of chambers and valves and to observe blood flow. In a transthoracic echocardiogram, the images are captured by placing an ultrasound transducer (the device emitting sound waves) in various spots on the chest and abdomen. In a transesophageal echocardiogram, a thin tube conveys a transducer down the esophagus, enabling doctors to obtain clearer heart images from inside the body.
- Vascular ultrasound. This imaging test uses sound waves to let doctors see how blood moves through veins and arteries.
- Blood tests. Analyzing a blood sample helps doctors assess a variety of health-related factors. Tests may quantify red blood cells and levels of electrolytes (elements such as sodium and potassium). Blood tests can also indicate how well the kidneys, liver and thyroid are functioning. In some instances, blood tests can point to the cause of a heart problem.
When your evaluation is complete, our team of specialists – which includes general cardiologists, interventional cardiologists, heart surgeons and imaging specialists – meets to discuss your case and determine whether TEER is an appropriate option for you.
Procedure
TEER is performed in the UCSF cardiac catheterization lab rather than a standard operating room. The procedure usually takes two to three hours, and patients are under general anesthesia (completely asleep).
To begin, the doctor makes a small incision in the groin area to access the femoral vein and – guided by X-ray and ultrasound imaging – threads a catheter through this blood vessel up to the heart. A tool on the catheter tip makes a tiny hole in the thin layer of muscle dividing the heart's chambers, so that the catheter can pass through and be guided to the mitral valve. The MitraClip or Pascal device is inserted through the catheter and brings the valve flaps closer together, facilitating better closure when the heart beats and reducing the backflow of blood. Once the device is in place and working, the doctor removes the catheter.
Recovery
Following the procedure, patients are monitored in either the post-anesthesia care unit or intensive care unit, depending on the level of care needed. Patients are generally encouraged to be up and walking within 24 hours, and most are able to do so. You will likely spend one to two nights in the hospital. During your post-op stay, your care team will conduct follow-up tests to ensure the device is functioning properly. These may include chest X-rays, blood tests, an electrocardiogram (EKG) and an echocardiogram (heart ultrasound).
Before you go home, your heart team will talk with you about how to care for yourself, providing instructions on diet, exercise, care of your incision site, and use of current or new medications. You will likely receive guidance about blood thinners.
Follow-up
After your discharge, you need to have regular checkups with your primary care provider and local cardiologist. You'll see your UCSF heart team as needed. These checkups are important to ensuring the device is functioning properly and to detecting any potential problems early.
Your doctor may recommend a cardiac rehabilitation program. In cardiac rehab, a team of health care professionals provides education and support to assist your recovery and prevent future heart problems.
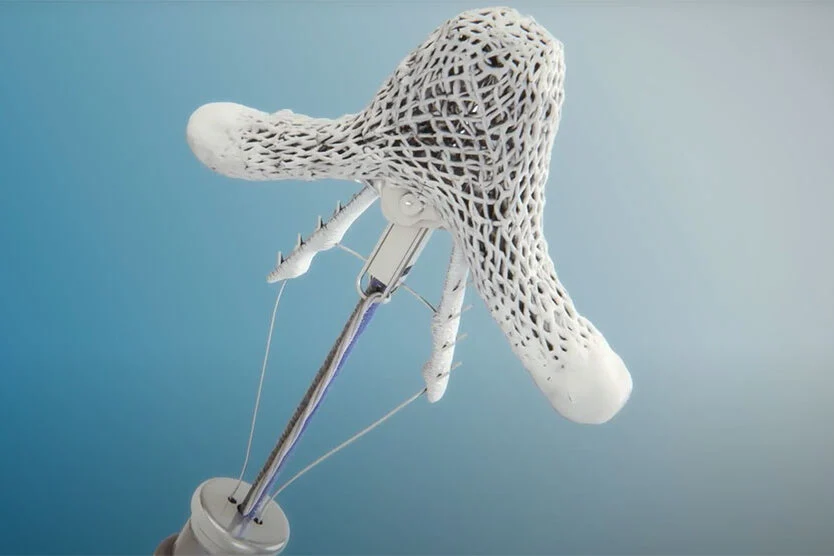
See how mitral valve regurgitation can be repaired with the MitraClip.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
Abbott, Abbott ‘A’, and MitraClip are trademarks of Abbott or its related companies. Reproduced with permission of Abbott, © 2021. All rights reserved.
