Percutaneous Coronary Intervention (PCI)
On this page
What is percutaneous coronary intervention (PCI)?
Percutaneous coronary intervention (PCI) is a minimally invasive procedure used to open blocked coronary (heart) arteries that are narrowed or clogged by fatty deposits known as plaque. Different methods are used. By restoring blood flow, the treatment can improve symptoms of blocked arteries, such as chest pain or shortness of breath.
In a PCI, the doctor reaches a blocked vessel by making a small incision in the wrist or groin and then threading a catheter, a thin, flexible tube, through an artery that leads to the heart. Using X-ray images of the heart as a guide to locate the blockage or narrowed area, the doctor then uses the most appropriate PCI techniques to open the vessel.
Our approach to PCI
UCSF interventional cardiologists are highly skilled and experienced in the latest PCI techniques and devices. They're able to use PCIs to fix the most complex coronary artery blockages, even chronic total occlusions, when the coronary artery is completely blocked for three months or longer.
Treatment with PCI
We offer a range of percutaneous coronary interventions, tailoring them to meet individual needs and optimize outcomes. All PCIs are performed in our cardiac catheterization labs, which are equipped with state-of-the-art technologies and equipment.
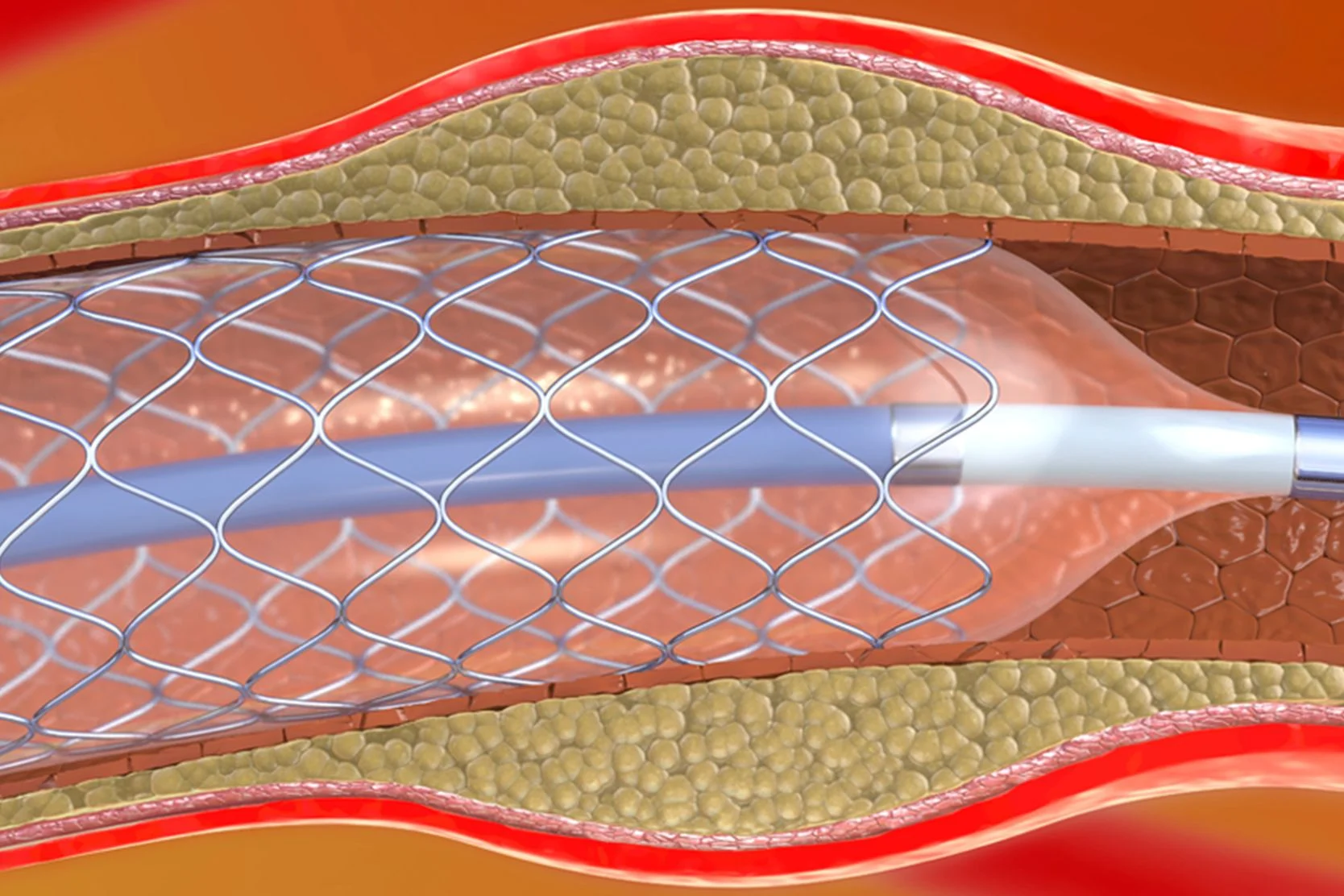
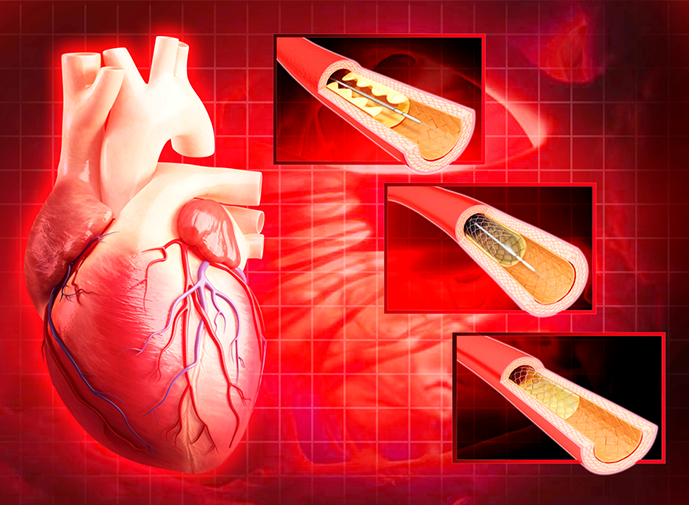
- Balloon angioplasty. This is the basic PCI procedure. A catheter with a tiny, folded balloon on its tip is threaded through a blood vessel until it reaches the site of the blockage. The balloon is then inflated to compress the plaque against the walls of the artery. This widens the passageway, restoring blood flow to the heart. The balloon is then deflated and removed.
- Angioplasty with stent. Generally, as part of the balloon angioplasty treatment, we place a stent (a tiny mesh tube) in the problem area to keep the artery open after the balloon is removed. Most stents are coated with special slow-release drugs that prevent the growth of scar tissue in the artery, further ensuring good blood flow.
- Rotational atherectomy. For those who have particularly tough blockages, our doctors use a special catheter-based tool to drill out calcified plaque deposits.
- Impella-supported PCI. This is for people at high risk of complications or those with severe heart disease. We insert a tiny device called the Impella heart pump into the heart to help it pump during the PCI procedure.
Preparing for the PCI procedure
Shortly before your percutaneous coronary intervention procedure, we may do the following:
- Give you a sedative to help you relax. For most PCIs, patients are sedated but not asleep.
- Clip your hair in the area where we'll insert the catheter, such as the upper leg or wrist
- Put an intravenous (IV) line in place to give you medications quickly, if necessary
- Place electrodes on your body to monitor your heart
- Clip a small device called a pulse oximeter on your finger or ear to track the oxygen level in your blood
Procedure for PCI
A PCI may take anywhere from one hour to three hours, depending on the complexity.
During the procedure, you will lie on your back on a procedure table. We will inject a numbing medication at the site where we will make a small incision and insert the catheter.
When the catheter reaches your heart, we'll inject a special dye that shows up well in medical imaging so that doctors can clearly see the vessel's narrowed area on an X-ray. This process is called a coronary angiography. The doctors will then perform the type of PCI that is best for your condition.
Once the procedure is finished, the doctor will withdraw the catheter and apply pressure to the insertion site to stop the bleeding.
Recovery from PCI
Post PCI, we'll take you to a recovery room for several hours of observation. You'll need to stay in bed for two to six hours, depending on your condition and the type of PCI you had. Some people need to stay in the hospital overnight.
If the catheter was inserted through your groin, you'll need to stay flat on your back and keep your leg straight for several hours. If the catheter was inserted in your wrist, your arm will be elevated on pillows and kept straight with a stabilizing board.
You may experience mild pain or an ache in your chest. If the discomfort is too much, we can give you pain medication. You may also be prescribed blood thinners to help prevent blood clots.
You'll be encouraged to drink water and other fluids to help flush the contrast dye from your body.
If you go home the same day, you'll need someone to drive you. You should not operate a car for 24 hours after the procedure.
Follow up after PCI
When you return home, keep an eye on the insertion site. A small bruise is normal, but contact your doctor for advice if you experience any of the following:
- Increased pain
- Redness
- Swelling
- Bleeding or discharge from the insertion site
- Fever or chills
You may shower 24 to 48 hours after the procedure. During this time, you should also avoid any strenuous exercise, sports, household chores and demanding physical tasks.
If the catheter was inserted into your wrist, you should also avoid activities that involve pulling or lifting with that wrist for five days after your PCI.
A week after your procedure, you can resume activities of moderate intensity. In fact, moderate physical activity (such as walking, swimming or using a stationary bike) at least five days a week is recommended to strengthen your heart. You may want to ask your doctor whether cardiac rehabilitation – a customized exercise and education program for improving your health – is an option for you.
Related services & conditions
Specialties
Conditions
- Coronary Artery Disease
- Atherosclerosis
- Cardiac Angina
- Chronic Total Occlusion
- Heart Failure (HF)
Treatments
- Coronary Artery Stent Placement
- Atherectomy
- Impella Insertion
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
