Preventing Liver Disease and Cancer Among Asian Americans
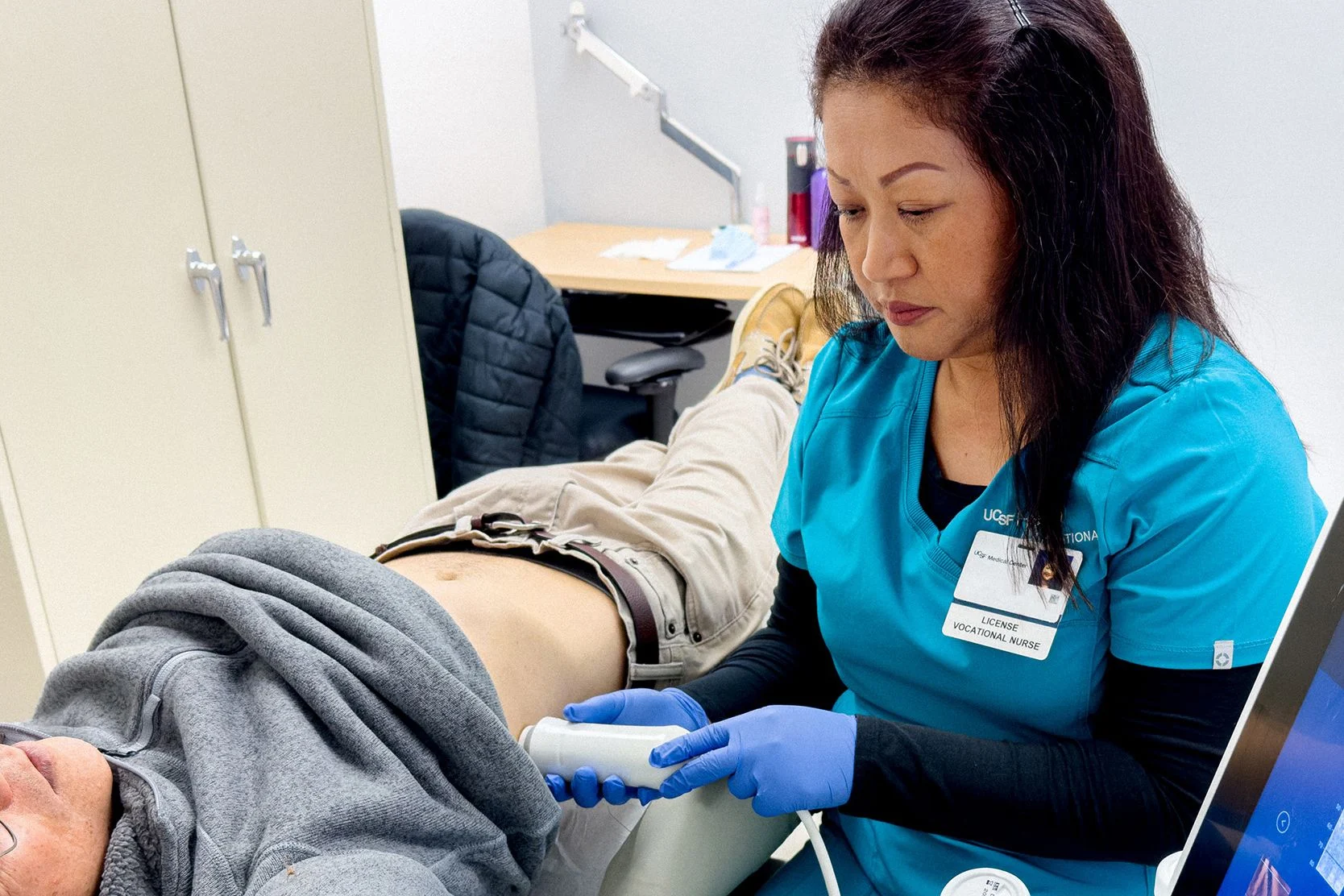
UCSF Health launched the Asian Liver Health Center, part of the Asian Health Institute and the Division of Gastroenterology, to tackle disparities around liver disease and liver cancer among Asian Americans. The population suffers from disproportionately high rates of hepatitis B infection, a leading risk factor for cirrhosis and liver cancer.
Liver disease is among the greatest health disparities for Asian Americans, who make up 6% of the population yet account for nearly 60% of liver cancer cases.
The center's co-directors, Dr. Francis Yao, medical director of UCSF's liver transplant program, and Dr. Elizabeth Zheng, explain why the risks of liver disease are higher in some Asian populations and how they hope their culturally and linguistically sensitive care can improve outcomes.

Dr. Francis Yao is co-director of the Asian Liver Health Center and medical director of the Liver Transplant Program at UCSF Health.

Sarah Pham serves as the research coordinator for the Asian Liver Health Center, which provides linguistically and culturally sensitive care.

Dr. Yao and his colleagues hope to improve health disparities around liver disease and liver cancer for Asian Americans.
A patient receives an ultrasound at the center, where providers hope to improve screening and treatment of hepatitis B.
What's behind the increased risk of liver disease in Asian communities?
Yao: Hepatitis. The prevalence of past or present hepatitis B is very high in many U.S. Asian populations – 10% of the population – and it's particularly high among Chinese and Vietnamese people. It's commonly spread from mother to child, and while newborns have been vaccinated in the U.S. since 1991, providing more than 90% protection, people born before 1991 haven't. Overall, the prevalence of chronic hepatitis B is 11 times higher among Asian Americans in the U.S. than among non-Hispanic white people.
How effective is vaccination at preventing mothers from transmitting hepatitis B to their newborns?
Yao: Vaccinating newborns protects the baby from catching the virus from the mother even if the mother is infected, but the protection is not 100%. Babies who are born to hepatitis B-positive mothers should also get immunoglobulin, and together, these provide about 90% protection. To reduce the risk of transmission even further, we have a strategy of treating mothers who have a high viral count with an antiviral agent in the third trimester of pregnancy.
What about hepatitis C, which is also a risk factor for liver cancer?
Yao: Hepatitis C is also common among Asians. Vietnamese populations have a higher rate of hepatitis C – about 5%, compared to about 1% in China. Hepatitis C is usually acquired from exposure to infected blood, such as [through] injection drug use while sharing needles or blood transfusion before 1990. You may also get hepatitis C from inadequately sterilized needles, for example with the practices of cupping and acupuncture. Hepatitis C is a risk factor for liver cancer when the liver disease progresses to cirrhosis.
At this early stage, what's the focus of the center's work?
Yao: We want to improve screening and treatment of hepatitis B among Asian Americans. Very often, patients are not aware that they have hepatitis B because they don't have any symptoms, so they don't get screened. Hepatitis B can be a silent disease for many years. I also think that some people do not want to check for liver disease due to stigma and misconceptions about liver disease – for example, the belief that all liver disease is the result of drinking alcohol.
It's the same with liver cancer, which may not cause symptoms at the early stage, and hepatitis B patients are at risk for developing liver cancer.
What's the advantage of early screening?
Zheng: There's no cure for hepatitis B, but there is medication that suppresses the virus to the point where we don't see complications, such as cirrhosis or liver failure. Once somebody is diagnosed with hepatitis B, they should continue to see a doctor regularly – not everyone needs medication right away, but at some point in their lives, they might need it. It's an important part of reducing disparities to make sure that patients are linked to care.
Yao: For my patients who have had hepatitis B, they routinely get blood tests and ultrasound for cancer screening every six months before seeing me, whether they are on treatment or not. Regular follow-up and monitoring are a long-term, very important part of care. It may be easier for the patient if the health care provider speaks the patient's language.
How does stigma in Asian communities influence patient care?
Zheng: Most of my patients who have hepatitis B are Chinese. And I will say I think many of them have this stigma against hepatitis B that has delayed treatment and prevented them from talking to their families about getting screened and vaccinated for hepatitis B.
I've been able to bond with many of my patients and their family members based on culture and my family's experience with hepatitis B. That's really helped to mitigate the barriers to starting treatment. And that's an aspect that patients can't find elsewhere: Patient education resonates more when you see a doctor who looks like you and has similar experiences.
What kinds of things are you doing to raise awareness?
Zheng: We recently did a community health fair in Chinatown, and next to us was the SF Hep B Free organization. They were providing free hepatitis B screening, and we were providing consultation and education.
Are there other liver diseases that deserve special attention in Asian populations?
Zheng: In the immediate term, we're focusing on hepatitis B education, mostly in East Asian populations. But our five-year and 10-year goals include incorporating other Asian American and Pacific Islander languages and cultures and other liver diseases. Another liver disease on the rise is fatty liver disease, which can lead to cirrhosis and liver cancer. Fatty liver is usually associated with alcohol use and obesity, but we are seeing it in non-obese Asian patients. As with hepatitis B, it often has no symptoms.
Why is this a rising issue now?
Zheng: Lifestyles have changed over the last 10 or 20 years. People are more sedentary, and that contributes to fatty liver across every culture.
Yao: The prevalence of fatty liver among Asians is rising. Asian patients with fatty liver often have lower body weight when compared to other populations. The diet among Asians may be changing and not as good as it used to be, making them susceptible to fatty liver. It's another area that needs more education.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
