This small pump can make a big difference in fighting cancer in the liver

About 3 inches in diameter, the disk resembles a shiny hockey puck when held in the palm of a hand. Before implanting this disease-fighting device in a patient, doctors fill its hollow titanium body with one ounce of liquid: a deadly cocktail for cancer cells invading the liver.
The disk is a hepatic arterial infusion (HAI) pump – a medical device that can be surgically placed in a patient's abdomen to continuously administer chemotherapy directly into the hepatic artery, which delivers blood to the liver. In other words, it fights cancer cells in the liver, where the cells are located, instead of the drugs traveling the 12,000 miles of blood vessels in an adult patient's body to reach their target, as with traditional chemotherapy.
"This treatment is a powerful option for patients with cancer that has spread to the liver from the colon and, when used with regular chemotherapy, it may help shrink the tumors and lower the chances of the cancer coming back," said Dr. Ajay Maker, chief of surgical oncology and surgeon-in-chief of the UCSF Helen Diller Family Comprehensive Cancer Center.
Only about 1% of medical centers in the U.S. offer the HAI pump as a treatment for cancer. UCSF is the sole hospital in the Bay Area, and one of just a few on the West Coast, to provide this targeted approach as an option for patients with inoperable colon cancer that has spread to the liver. Maker leads the hospital's surgical HAI pump program, which is one of the country's highest-volume HAI pump programs.
"This type of specialized care is only possible through a true team-based approach at UCSF that combines cutting-edge surgical teams with world-class medical oncology experts," he said.
Secondary liver cancer – cancer that has spread to the liver from other parts of the body, such as the colon – is the second leading cause of cancer-related death in the world. The surgery to implant the pump in the hepatic artery requires extensive training and expertise due to the liver's intricate network of blood vessels and bile ducts.
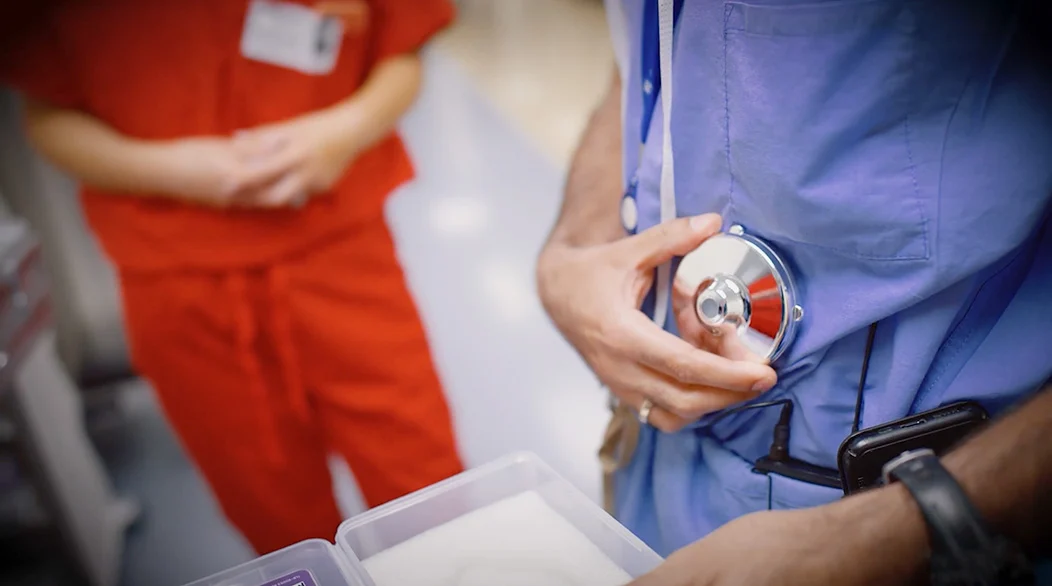
Dr. Ajay Maker shows where the hepatic arterial infusion (HAI) pump is implanted in the abdomen to continuously administer chemotherapy to the liver.
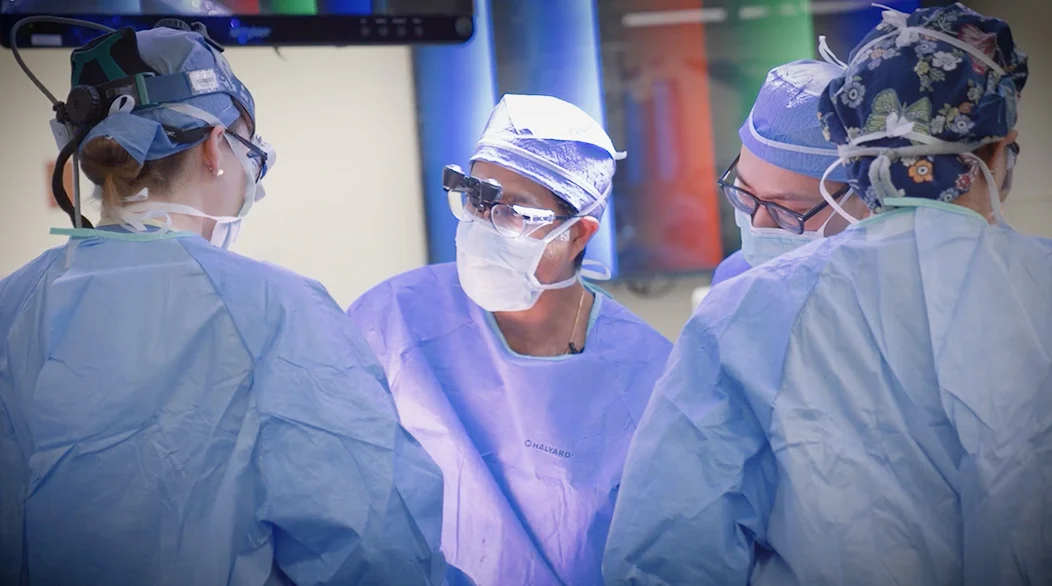
During the operation to surgically implant the HAI pump and attach it to the hepatic artery, doctors will remove metastatic liver tumors.

Dr. Maker collaborates with his laboratory research team to improve treatments for patients with cancer and transform their lives.
This treatment is a powerful option for patients with cancer that has spread to the liver from the colon.
In this operation, the team secures the chemotherapy-filled pump in a subcutaneous pocket below the ribs in the patient's lower abdomen. They may also remove the metastatic liver tumors. Using a catheter (a thin, flexible tube), the pump is attached to the hepatic artery, which sends high doses of the medication to the liver. A full pump has enough medication to last up to two weeks, and when the amount remaining gets low, the pump can be refilled without the need for further surgery. Though the HAI pump causes fewer whole-body side effects than standard chemo, the drugs can still cause problems in the liver, so patients are closely monitored.
Maker noted that the best results have been recorded when the HAI pump is initially used in conjunction with regular systemic chemotherapy.
One patient's success story
Following surgery and chemotherapy for colon cancer, Tess Zarate became one of Maker's first HAI patients at UCSF. In 2021, after learning that her cancer had spread to her liver, she jumped at the chance to receive chemotherapy with the HAI pump.
"Dr. Maker said I was a perfect candidate for the HAI procedure," Zarate said. The main reasons for this were that her liver lesions were small, she had experienced a negative reaction to intravenous chemotherapy in the past, and she was willing to try something different. Her pump became her lifeline, and she named it "Hope."
"I knew the only way to know if it would work was to do the surgery," Zarate said. "I had a drive and determination to see this through. It never occurred to me to say no."
For her six months of chemo with the pump, Zarate made sure her body temperature did not fluctuate to extremes and that she stayed hydrated and got plenty of sleep.
"Tess had the right combination of responsive tumor biology; we were able to remove all the liver tumors during the surgery; and with Dr. [Chloe] Atreya, her oncologist, she was expertly managed to safely tolerate HAI chemotherapy," Maker said.
Zarate planned vacations around her pump refills, and only once in the six-month treatment period did she hear the alarm indicating that her medication supply was low. "'Hope' was screaming," Zarate joked. "She was thirsty."
Five years after her diagnosis, Zarate was declared cancer-free.
"I wanted the HAI pump to work, not just for me but for others," she said. "'Hope' gave me only a few side effects. However, I'm not out of the woods. I have been given a gift, and I don't take it lightly."
Zarate still has "Hope" inside her abdomen. She plans to have it removed eventually but knows it will be an emotional decision after a long treatment journey in which the HAI pump played a pivotal role.
"It wasn't easy," she said. "But it was so worth it."
Images by Tom Seawell
Caring for patients using the HAI pump

A Day in the Life: Dr. Ajay Maker
Related treatments
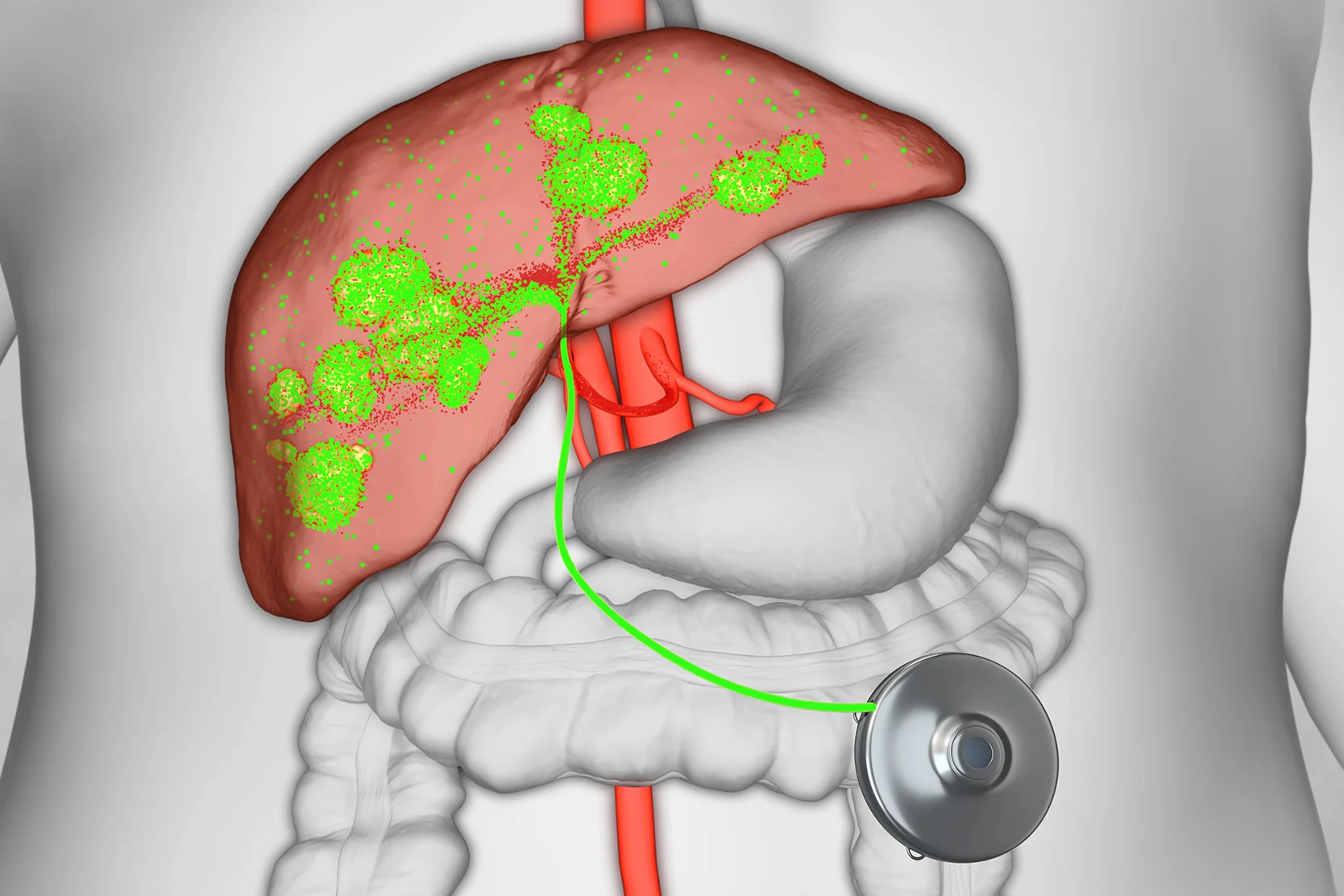
Hepatic Artery Infusion Pump
This implanted pump delivers chemotherapy directly to liver tumors, providing an effective treatment option for metastatic colon or bile duct cancer.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
