Robotic Whipple Surgery
On this page
The robotic Whipple procedure is a minimally invasive version of the Whipple procedure or pancreatoduodenectomy, a complex surgery used to treat pancreatic cancer and other disorders that may require removal of the pancreas or bile duct. The operation involves removing parts of the pancreas, small intestine gallbladder, bile duct, lymph nodes, and sometimes also the end of the stomach, and then reconnecting the organs so that food can be properly digested.
The only medical center in the Bay Area that is performing the total robotic Whipple is UCSF.
Robotic Whipple vs. traditional Whipple
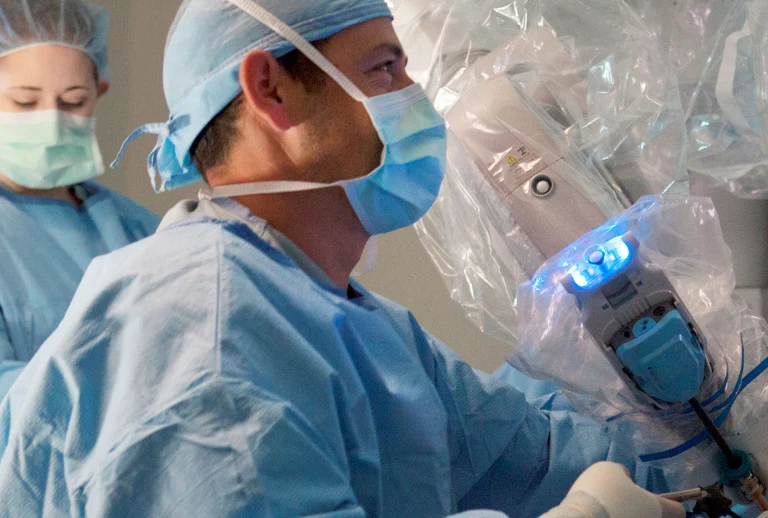
In the traditional Whipple, the surgeon makes an abdominal incision to remove and reconstruct affected organs and tissues. For the robotic Whipple, the surgeon operates through several small incisions, using robotic arms equipped with special instruments and a tiny camera. The robotic arms can move precisely and with a wide range of motion like a surgeon's hands, while the camera provides a complete 3D view of the abdominal interior. Because the procedure is less invasive, patients may experience fewer complications and recover more quickly.
Why choose UCSF for Whipple surgery?
The Whipple is considered one of the most complicated and difficult gastrointestinal surgeries, requiring a high level of training and experience. Thanks to our expert gastrointestinal surgical oncology team and state-of-the-art robotic surgery program, UCSF is the only medical center in the Bay Area that provides both versions (traditional and robotic) of the procedure. We also offer robotic approaches to numerous other surgeries, including treatments for various cancers, uterine fibroids and endometriosis; repairs of female pelvic organ prolapse, heart valve problems and hernias; and bariatric surgery.
Who can get Whipple surgery?
The robotic Whipple is for select patients diagnosed with pancreatic cancer or other disorders of the pancreas or bile duct requiring removal of part of the pancreas.
Advantages of robotic Whipple
The robotic procedure is minimally invasive, and the surgeon uses a da Vinci surgical system. These differences may confer a number of potential advantages, including:
- Smaller incisions (and therefore, smaller scars)
- Less blood loss
- Less postoperative pain
- Faster recovery
Patient stories

Tackling cancer with the Whipple procedure
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
