Mastectomy

On this page
Mastectomy is the surgical removal of all breast tissue. This procedure is used to treat breast cancer and sometimes to help prevent it in patients who are at high risk. It may be performed on one or both breasts. Other nearby tissues, such as lymph nodes, may also be removed to determine whether cancer cells have spread.
Some breast cancer patients can choose between a mastectomy and a lumpectomy, where the surgeon removes only the tumor and a small amount of surrounding tissue, preserving as much healthy breast tissue as possible. Lumpectomy is typically followed by radiation therapy.
You'll be advised to choose a mastectomy if:
- You have several tumors in different parts of your breast
- Your tumor is large
- You're not a good candidate for radiation therapy
Mastectomy options
There are different types of mastectomies. You and your surgeon will discuss your options in detail.
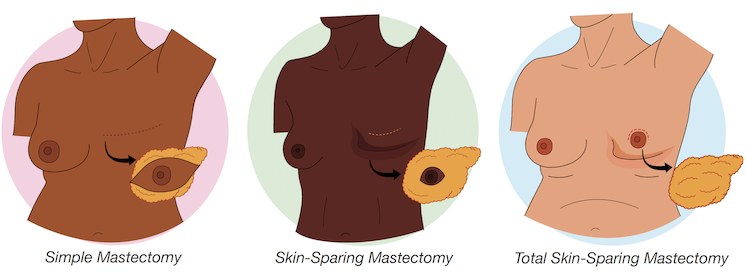
Simple mastectomy (no reconstruction)
In a simple, or traditional, mastectomy, much of the breast skin is removed. This leaves permanent scars on the chest.
Following a simple mastectomy, patients generally need four to six weeks before the chest wall is healed and discomfort has decreased enough to get fitted for a breast prosthesis (a breast form that fits into the cup of your bra). There is also a cotton camisole available with built-in breast prostheses.
Most insurance plans cover four post-mastectomy bras and a prosthesis each year. It's important to be properly fitted by someone who is trained in this. You can schedule a fitting at the Friend to Friend Specialty Shops at our Mission Bay or Mount Zion campus. The stores also carry bathing suits and other clothing made to use with breast prostheses.
Skin-sparing mastectomy
A skin-sparing mastectomy preserves the breast skin but not the skin of the nipple and areola. The procedure leaves a scar across the center of the breast. You may consider having an additional surgery at a later date to recreate the nipple. A 3D nipple tattoo by a professional tattoo artist is another option.
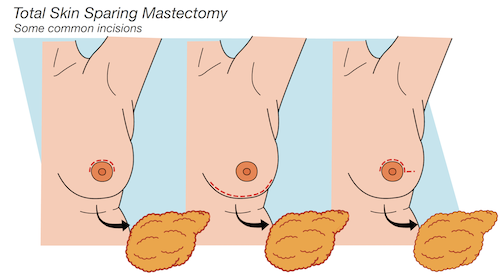
Total skin-sparing mastectomy
A total skin-sparing mastectomy preserves the skin of the breast, nipple and areola by removing only the breast tissues below. This procedure is not an option if you:
- Have breast cancer in or near the nipple
- Have extensive disease
- Have large, pendulous breasts
- Are a smoker
Breast reconstruction
While going over mastectomy options with your surgeon, you'll also discuss the possibility of breast reconstruction. If you choose to have it, you can start the process during your mastectomy procedure or at a later date. If you're interested in reconstructive surgery, you should know that the type of mastectomy you choose, among other factors, will determine your reconstruction options.
For more information, please visit our breast reconstruction page.
Preparation
Before your mastectomy, you'll meet with your surgeon to discuss your medical history and details of the operation. You'll also receive specific instructions on how to prepare.
You'll need to arrange to have a responsible adult drive you home from the hospital. We cannot allow patients to use taxis or other car services to return home unless they're accompanied by someone they know.
Procedure
A mastectomy takes about one to three hours. You will be under general anesthesia (completely asleep) throughout the procedure.
The surgeon makes an incision in your breast to remove the tissue, which will be analyzed by a pathologist. If you've chosen to have breast reconstruction at the same time as your mastectomy, a reconstructive surgeon will perform that procedure after your breast tissue has been removed.
Once the procedure is complete, the surgeon closes all incisions with stitches that will either dissolve on their own or be removed later by a doctor. You're then moved to a recovery room and monitored while you wake up from the anesthesia.
When you wake up, you will most likely have tubes in the surgical area that allow fluid from the wound to drain. Tubes are removed one to two weeks after surgery.
Most patients stay overnight in the hospital after a mastectomy. If you have breast reconstruction at the same time, you may stay an additional one to two nights.
Recovery
You'll likely experience soreness in your chest and underarm, tenderness at the incision site, and numbness where the scar is healing. If lymph nodes were removed, you may also feel numb or a burning sensation in your armpit and the area below.
Before you're discharged from the hospital, your medical team will give you detailed instructions for your recovery at home, including how to manage pain, bathe, and care for your incision, including use of surgical dressings and drainage tubes.
You'll return for a post-op appointment eight to 14 days after your mastectomy. At this visit, we'll discuss the pathology results from your surgery. We'll also remove the drain tubes during this appointment.
Recovery after a mastectomy typically takes about four weeks. Most patients return to work within three to six weeks, depending on the physical demands of their job. Please discuss the timing with your medical team.
You may have an array of physical and emotional responses to the changes in your body after surgery. Most patients experience a significant change in breast sensation. Please ask your care team what changes in sensation are typical with the type of mastectomy you plan to have.
If you have any questions or concerns once you return home, please call the Breast Care Center.
Related services & conditions
Specialties
Conditions
Patient education

Preparing for a Lumpectomy or Mastectomy
Here’s how to prepare for a lumpectomy or mastectomy, including arrangements you should make before surgery, what to eat and items to bring to the hospital.
Types of Autologous (Free Flap) Breast Reconstruction
There are several breast reconstruction options after breast cancer treatment. Understand the free flap procedures your surgeon may recommend.
Related services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.





