Radical Prostatectomy
On this page
Radical Prostatectomy
A radical prostatectomy is surgery to remove the prostate gland and seminal vesicles (and sometimes nearby lymph nodes) after a prostate cancer diagnosis. It is one treatment option for patients with localized prostate cancer. Candidates for the surgery should be in good health and expected to live at least 10 more years.
Preparing for surgery
Before surgery, your doctor may order a variety of tests to determine the extent of your cancer. These include blood tests and imaging tests, such as MRI, CT, bone scan and PET. If you were diagnosed elsewhere, your UCSF surgeon may want to repeat some tests and review your biopsy slides.
In addition, we will make a "prepare" appointment to discuss your physical condition, medication use, relevant medical history and forthcoming anesthesia – either by phone or in person. One of the urology nurses, nurse practitioners or physician assistants will explain what you need to know to prepare for your surgery, providing instructions on eating and drinking as well as other details.
If you've ever experienced vomiting or nausea after surgery, be sure to let your anesthesiologist or surgeon know. Ask about taking a medication the night before to prevent post-op nausea or vomiting.
You could have an autologous blood donation (donate your own blood) prior to surgery, but this is rarely done for radical prostatectomies since there's little blood loss and the risk of needing a transfusion is low (less than 1%).
Plan on having these items for the hospital or ready for your return home:
- Your own pillow for comfort (hospital)
- Incontinence pads or adult diapers (home)
- Loose sweatpants, robe or shorts (home and hospital)
- Plenty of non-carbonated drinks (home)
- Regular tea or laxative tea, such as Smooth Move from Traditional Medicinals (home)
It may be possible to have a family member or friend stay overnight with you in the hospital. Please check with your nurse about current restrictions. You will not be in intensive care, but you will be closely monitored by nursing staff.
Make plans for your postoperative care:
- Identify a place at home where you can relax and take pressure off the healing area; this may be a sofa, comfortable chair or, ideally, recliner.
- Make sure someone can bring you home from the hospital, as you won't be allowed to leave on your own. It's also helpful to have someone with you at discharge to help track the instructions you get about medications, activities and catheter care.
- Try to have all post-op prescriptions filled before your admission to the hospital, so they will be waiting for you at home. The hospital does not provide medications to take with you. If you'd like Walgreens to deliver medications to you in the hospital before discharge ("Meds to Beds"), please have a credit card with you for any co-pay. Many patients choose this service to avoid having to stop at a pharmacy on the way home.
During surgery
You are placed under general anesthesia. After you are completely asleep, the surgeon makes several incisions in your lower belly to access your prostate gland and surrounding tissues and one larger incision above your belly button, through which the prostate gland is removed. (The exact number of incisions depends on the robotic system being used, the extent of your cancer and your surgeon's preference.)
Depending on your situation, the surgeon may remove just the prostate gland and seminal vesicles. If there's concern the cancer has spread to nearby lymph nodes, the surgeon may also remove them to be biopsied. The bladder, having been disconnected from the urethra by the prostate's removal, is reattached to the urethra. To facilitate healing, a catheter is left in the bladder to drain urine. (Care and removal of the catheter are discussed later.)
Your surgeon also may leave a temporary tube in the area where the prostate was removed to drain fluids that may accumulate. That tube is usually removed on the day you leave the hospital.
The entire operation, including anesthesia and set-up, takes about four hours.
Nerve-sparing radical prostatectomy
The neurovascular bundles (nerves and blood vessels), which allow the penis to become erect, run on either side of the prostate. Either or both of these bundles may be partially or completely spared during the surgery, preserving sexual function in some patients. The best results are achieved if both bundles can be spared. Younger patients who are sexually active and report having good erections are most likely to benefit from bundle preservation. Older patients and men who have been experiencing limited erections are less likely to benefit (however, nerve preservation may also improve urinary function). In some cases, bundle preservation may not be advised due to the cancer's location or extent. These nerves run very close to the prostate, so preserving the bundles may risk leaving cancer behind in some patients. Understanding that a change in sexual function is a common side effect of radical prostatectomy, you and your surgeon should discuss the risks and benefits of nerve-sparing surgery.
After surgery
When the procedure is finished, you are taken to recovery and then to your hospital room, where nurses monitor your condition. Most patients stay in the hospital for a day or two at most.
While in the hospital
It's important to your recovery to start moving as soon as possible. Most men are out of bed and walking around the unit on the same day as their surgery. Your nurse will assist you until you can manage on your own. When you first get up, raise the head of your bed, take a couple of deep breaths, and allow your body to adjust to the change in position. Dangle your feet over the side of the bed for a few minutes, then slowly stand up. Be careful because getting up too quickly can make you light-headed.
Get out of bed at least three times each day – preferably more. This helps prevent lung infections and blood clots. You may be prescribed an injectable blood thinner to further reduce the risk of blood clots. The more time you spend out of bed, the faster you will recover and the faster your bowel function will return to normal. Your nurse will also give you an oral stool softener and mild laxative to prevent constipation.
In addition to walking, you will be encouraged to do two other things that help prevent complications: Use an incentive spirometer (a small disposable device that promotes deep breathing), and wear compression stockings while in bed. Both will be provided and the nurses will instruct you on how to use them.
Postsurgical pain
You may experience different types of pain, all of which are normal. You may feel:
- Surgical pain – Pain along the incisions is to be expected but can be managed. Let your nurse know if you need pain medication, which may be oral or intravenous. Be mindful that taking narcotics can contribute to constipation or gas pain. Your nurse will give you an oral stool softener and mild laxative to prevent constipation.
- Bladder spasms – With a catheter in place, patients commonly experience intermittent episodes of pain just above the pubic bone and radiating down the penis, or intense urges to urinate or have a bowel movement. The spasms will resolve once the catheter is removed. Meanwhile, proper drainage of the catheter is essential and your nurse will assist you with this. To alleviate the spasms, your nurse will give you an oral medication called Ditropan (oxybutynin) or a belladonna and opium (B&O) suppository, or both. Oral Ditropan will also be prescribed for you at discharge.
- Gas pain – Unfortunately, no medication alleviates this. The best way to ease gas pain is to walk frequently, which helps gas move through your bowels. Also helpful for soothing the stomach are using a warm pack or heating pad on your abdomen and drinking hot herbal tea (chamomile, peppermint or a senna leaf–based tea, such as Smooth Move).
Leaving the hospital
Most patients are well enough to go home the day after surgery, typically by noon. Others stay two nights or more, and others may even leave on the same day as their surgery. If you have a drain where your prostate was removed, we will take this tube out before you go home. Your urinary catheter will still be in place, and your nurse will instruct you on its use and other home care. You'll also receive instructions regarding diet, exercise and rest. Take notes, if you're able. And if you are fortunate enough to have someone with you, have them takes notes, too. You will not, understandably, be at your sharpest for remembering all the information presented to you.
We recommend that you request a special cushion for easing pressure on the healing areas when you sit. You may also want to request an extra catheter leg fastener (used to secure the catheter to one of your legs) in case you need to move the attachment position when you get home. These items can be difficult to locate after leaving the hospital.
It's important to know that you will be required to have someone drive you home from the hospital.
Activity
It's normal to feel tired for several weeks after this surgery. Follow these post-op guidelines on certain activities:
- No driving while the urinary catheter is in place. Resume driving only after the catheter has been removed, you are no longer taking narcotic pain medication, and you can comfortably twist your torso quickly to look over your shoulder when driving.
- No moderate or heavy lifting or abdominal straining for three to four weeks.
- No exercises that stress your abdominal muscles or perineum (area between scrotum and anus) for four to six weeks. Examples of exercises to avoid are sit-ups, vigorous cardiovascular activity and upright bicycling. Once the urinary catheter is removed, you can start doing light exercises, such as swimming, walking, jogging and stretching. But if a particular activity seems to cause pain or blood in your urine, that's likely an activity to avoid. Cycling usually becomes safe at four weeks after surgery, but cyclists should take care to avoid excessive pressure on the perineum.
- Sexual activity can resume once the catheter is out, you feel well, and you have a reasonable level of urinary control.
Returning to work
How much time must pass before you can return to work depends on the nature of your job and your recovery progress. For office work, a period of two to three weeks after surgery is typical, assuming the same criteria described for driving have been met. For physically demanding work, a longer recovery time may be needed.
Dealing with discomfort
You may be given a prescription for oral pain medication to use at home. Bear in mind that some of these medications – such as Tramadol, Norco, Vicodin, oxycodone and Ditropan – commonly cause constipation. These medications are not often needed and are not routinely prescribed. If you do have a prescription, take this drug only as needed (not on a regular schedule), do not drive or operate machinery, and avoid alcohol.
Many patients find all they need to manage their pain is over-the-counter acetaminophen (Tylenol) and ibuprofen (Motrin or Advil). For the most effective pain management, alternate the two types. For example, take 500 to 1,000 mg oral acetaminophen; 3 hours later, take 200 to 400 mg oral ibuprofen; 3 hours later, take 500 to 1,000 mg acetaminophen; 3 hours later, take 200 to 400 mg ibuprofen. Continue to alternate the medications, taking the same doses at the same time intervals. Keep a log to ensure accuracy. Be careful to never take more than 4,000 mg acetaminophen or more than 2,400 mg ibuprofen in a 24-hour period.
Diet, fluids and bowel movements
Constipation is a common side effect of pain medications and surgery. You should have received prescriptions for an oral stool softener and a laxative. (If not, please contact your doctor.)
You should start drinking fluids as soon as you are comfortable after surgery, and you can resume your normal diet (solid food) the first day after surgery. But while waiting for normal bowel function to return, you should avoid large meals in favor of several small meals a day. To prevent constipation, we recommend drinking at least eight to 10 glasses of fluids each day and eating lots of fruits and vegetables. Avoid carbonated beverages and cruciferous vegetables – such as broccoli, cauliflower, brussels sprouts and cabbage – for approximately two weeks, as they frequently cause gassy discomfort and distention.
Take your stool softener and laxative as prescribed. Normal trajectory for return of bowel function is one to two days to pass gas, three to five days for the first bowel movement.
If you haven't had a bowel movement by day three after your surgery, take oral Miralax (dissolvable powder), an over-the-counter laxative. You can combine Miralax with the prescribed stool softener and laxative. Follow the instructions on the box. Do not use any enemas or take stronger laxatives, such as magnesium citrate. Contact the clinic if you still haven't had a bowel movement by day five.
It can take at least two weeks for normal bowel function to return. To avoid irritating the surgery site, do not strain when trying to defecate. Straining can lead to increased pain, bleeding and delayed recovery. Most patients require use of stool softeners and laxatives for two weeks or even a month after surgery.
Caring for the incision
You will be able to take a shower the second day after your surgery. You may continue to have some discharge at the drain site for three to five days. Once you leave the hospital, the key words on caring for the drain site and incisions are clean and dry. Showering once a day and gently patting the area with a clean towel should be sufficient.
Caring for the catheter
You will be discharged with a Foley catheter, a tube that continuously drains urine from your bladder into a bag and that you will use for seven to 10 days. Before you leave the hospital, your nurse will teach you how to empty and care for your catheter and drainage bag. The catheter works with gravity and should be draining urine at all times, so you have to keep the drainage bag below your bladder at all times, even when you shower. If your urine is not draining, lower the bag and check the connection for kinks or loops. Loops can cause an air lock that prevents drainage. You can also try emptying the bag. Then try briefly disconnecting the catheter from the clear plastic tubing to allow a little air into the system. Your nurse will show you how to do this before your discharge.
To prevent infection, you must keep your catheter clean. This section explains how to clean the catheter, the area around the catheter and the drainage bag. It also explains how to apply your leg bag and secure the catheter to your leg.
We will provide most of the supplies you need to care for your catheter. They include:
- Blue clamp
- Alcohol pads
- Clear plastic tape
- Skin protectant
- Leg bags
- StatLock Foley catheter securement device
- Shaving supplies
Twice a day (morning and evening), use soap, warm water and a clean washcloth to clean the skin around your urinary meatus (the opening on the penis where urine comes out). Wash gently in a circular motion, moving away from the meatus. Hold the end of the catheter tube to keep it from being tugged while cleaning. Wash around the catheter to remove any blood, crust or mucus, and also gently clean the catheter itself of any built-up fluid or crust. Always wash the area around your anus last. Rinse, then pat dry your genital area and catheter with a clean towel. If you are uncircumcised, retract your foreskin, clean around and under it, dry the area, and return the foreskin to its original position. Clean the skin around your meatus and catheter after every bowel movement.
You should empty the catheter bag when it's half full. This helps prevent air locks from developing in the tubing.
To apply the leg bag:
- Wash your hands with soap and water.
- Remove the tape at the joint of the catheter tube and bag.
- Swab all connecting areas with alcohol pads.
- Use the blue clamp to close off your catheter above the bag.
- Drain, then remove the big drainage bag.
- Attach the leg bag to the catheter and to your leg. To enable urinary drainage, make sure the leg bag is in the upright position, below your thigh.
- Remove the blue clamp.
- Position the leg bag for comfort, making sure the tubing isn't kinked and is always below the level of your bladder.
If you need to change the position of the catheter and re-secure it to your leg:
- Find a location on your leg to secure the catheter so it's comfortable in both a sitting and walking position and not liable to kink.
- If you have a lot of body hair, shave that patch of your skin.
- Apply skin protectant to this patch of clean, dry skin. Let it dry.
- Apply the securement device on the dry patch of skin where you want to secure the catheter.
- Secure the catheter to the catheter securement device (as your nurse demonstrated prior to your discharge from the hospital).
The catheter bag should be changed halfway through the time the catheter is in place. The smaller, more easily hidden leg bag is available should you need it, but you'll need to check and empty it more frequently than the larger bag. To minimize your risk of infection, it's best to use the larger drainage bag as much as possible.
Your catheter will be removed in the clinic seven to 10 days after your surgery. If you are taking Ditropan, make sure the final dose is at least 24 hours before your appointment, so as to avoid urinary retention after the catheter is removed. An hour before the catheter is removed, increase your fluid intake; this will help you to urinate on your own sooner. You are expected to urinate within four hours of catheter removal. Prior to catheter removal, you will typically be given an antibiotic to help prevent a urinary tract infection.
| Normal things to expect | Abnormal things |
|
For these concerns, call us immediately at (415) 353-7171. Someone is available 24/7. |
Dealing with incontinence
After radical prostatectomy, all patients experience some urinary incontinence. This can range from leaking a small amount of urine to having no sense of urge control. After the catheter is removed, you may experience leakage with coughing, straining, laughing, sneezing, standing up after sitting, and other activities that increase abdominal pressure. You may need to wear incontinence pads or disposable absorbent underwear for a period of time. You can purchase these at your local pharmacy. Typical time to recovery of continence is about three months, and your bladder control may continue to gradually improve for six to 12 months following your surgery. One way to help regain control of urination is by doing Kegel exercises, which work the pelvic floor muscles.
Pelvic floor exercises – The pelvic floor muscles wrap around the underside of the bladder and rectum. Doing exercises in which you contract and relax this muscle group strengthens the pelvic floor and may reduce urinary urgency and incontinence.
Do not start pelvic floor exercises while you have your Foley catheter in place. That can cause discomfort and trigger bladder spasms. Even after the catheter is removed, it's best to wait an additional two to three days. If your urine stream is weak, doing the pelvic floor exercises may increase inflammation and lead to urinary retention. It's important to have a strong urinary stream before starting Kegels.
How do you know if you're isolating the right muscles and doing Kegels properly? It's easy: If you're contracting the muscles correctly, you should see a slight lifting-up movement in the penis – the same movement you see if you abruptly stop urinating. You should not be tightening your buttocks or stomach. At first, you can try practicing the Kegel movement by interrupting your stream while urinating. But don't do that routinely, as it can lead to infection. A better way to practice Kegels is by standing sideways in front of a mirror to confirm you are doing them correctly. You may also wish to use a smartphone app for guided instructions.
Initially, the quality of your Kegel exercises is more important than the quantity. With each Kegel, hold the squeeze for 10 to 15 seconds and then relax the muscles for the same duration. Do this 15 to 20 times to complete one set of Kegels. We recommend doing three or four sets over the course of each day. But don't overdo: Excessive Kegel exercising can lead to muscle fatigue and urine leakage.
Becoming good at these exercises takes time, effort and practice. You should start to see benefits after a few weeks, though it often takes about eight weeks for most improvement to occur.
Postsurgical medications
- Colace (stool softener): 1 tablet twice a day (morning and night).
- Senna (laxative): 2 tablets twice a day (morning and night).
- If no bowel movement in a three-day period of time, Miralax: 1 packet dissolved into fluids in the morning (OK to combine with colace and senna).
- Acetaminophen (Tylenol): 500-1,000 mg every 6 hours for mild pain, alternating with ibuprofen. Take on a scheduled basis for three days after surgery, then as needed.
- Ibuprofen 200-400 mg every 6 hours for mild pain, alternating with acetaminophen.
- If prescribed narcotic pain medication (Tramadol, Vicodin, Norco, Percocet, oxycodone), follow the directions on your prescription at time of discharge.
- Lidocaine gel: Apply to tip of penis for irritation every hour, as needed. Use sparingly.
- Antibiotic, per your urologist's preference, for removal of Foley catheter.
- Cialis, Viagra or Levitra: one-half tablet initially (after removal of the Foley catheter). If no significant side effects, increase to 1 tablet. Continue until follow-up with your surgeon. (However, if you're experiencing any postsurgical discomfort, dizziness, flu-like symptoms, or generalized fatigue or weakness, do not start this medication.) You may want to explore discount pricing for your Cialis, Viagra or Levitra. UCSF has special pricing available through select Walgreens. If you have any questions, speak with your health care provider.
The table below shows the postsurgical medication schedule that patients generally follow. Please be aware that this is a generic document and each UCSF patient will receive specific, individualized discharge instructions. If there is disagreement between these two documents, follow your discharge instructions. The "as needed" medications are not included in the calendar below.
POD = postoperative day
| POD 0 | POD 1 | POD 2 | POD 3 | POD 4 | POD 5 | POD 6 |
| Surgery day | Discharged home | Start showering | ||||
| colace, senna, Tylenol, ibuprofen | colace, senna, Tylenol, ibuprofen | colace, senna, Tylenol, ibuprofen | colace, senna, Tylenol, ibuprofen | colace, senna | colace, senna | colace, senna |
12
| POD 7* | POD 8* | POD 9/10* | POD10/11* | POD 11 | POD 12 | POD 13 |
|
Day before Foley catheter removal |
Morning of Foley catheter removal |
Start Cialis/Levitra/Viagra (start day after Foley catheter removal) |
||||
|
Antibiotic as prescribed for catheter removal |
||||||
| colace, senna | colace, senna | colace, senna | colace, senna | colace, senna | colace, senna | colace, senna |
This schedule assumes that Foley catheter removal takes place on day 9 or 10. The timing should be adjusted if your catheter removal takes place on a different day.
*See medication instructions for POD 9 to POD 11 if having early removal of Foley catheter.
Postsurgical follow-up
You'll have a follow-up appointment with one of your your health care providers (urologist, nurse practitioner or physician assistant) eight to 10 weeks after your surgery. An ultrasensitive PSA blood test should be done one week before the appointment. You'll receive the lab slip ordering the test at either your discharge from the hospital or your catheter removal appointment. If you have your blood drawn at a non-UCSF lab, please verify that the lab will perform an ultrasensitive PSA assay and the results will be sent to UCSF. You should also bring a copy of the result with you to the visit.
Pathology results
Processing pathology results usually takes 10 to 14 business days following surgery. How the results are transmitted to you (by phone, in person or through MyChart) depends on your urologist's preference. If you haven't been contacted about your pathology results by the time of your Foley catheter removal, please ask your nurse at that time.
The pathologist's report will focus mainly on three important features:
- Cancer grade – The grade reflects how abnormal the cells look under magnification. The more abnormal the arrangement of cells, the more likely the tumor will grow aggressively. The most commonly used grading system, the Gleason system, uses a scale ranging from 3 (most like normal cells) through 5 (least like normal cells). Because prostate cancer cells can have a mixture of different grades, two grades are given. The first number is the most common cell type and the second is the second most common cell type (for example, Gleason 3+4 means the tumor is mostly pattern 3 with some pattern 4).
- Cancer stage – This measure defines the extent of a tumor. T2 cancers are those completely confined to the prostate. T3 cancers have spread beyond the prostate, either through the prostate capsule (T3a) or into the seminal vesicles (T3b). Patients with T3 cancers are at an increased risk of recurrence compared with those who have T2 cancers. T4 cancers are rare and include cancers that have invaded nearby organs, such as the bladder.
- Margins – The edges of the tissue removed in surgery are the margins. A positive margin means that the pathologist found cancer cells at the very edge of the tissue. The pathologist will note the number and location of any positive margins. Patients with positive surgical margins are at an increased risk of cancer recurrence since this can be an indication that some cancer may have been left in the body. Patients with more than one positive margin are more likely to have their cancer recur than those with a single positive margin. Patients with an extensive positive margin (a large area where the cancer is in contact with the edge of the specimen) are more likely to have a recurrence than those with a very small area (focal positive margins) where cancer just touches the edge. Most patients with focal positive margins (4mm or less) are cured by prostatectomy alone and don't require further treatment.
Depending on your postoperative PSA, your doctor may recommend radiation as an additional treatment to decrease the risk of recurrence. Patients with undetectable PSA values usually continue to be followed rather than having radiation.
Additional treatment
Many patients don't need additional treatment after a radical prostatectomy. You and your doctor will decide about this based on the pathology report, your postsurgical ultrasensitive PSA level, and in some cases, the results of genomic testing of the tumor. Our goal is for your ultrasensitive PSA to drop to undetectable levels after surgery. Undetectable doesn't mean your PSA level is at zero. Rather, it means your PSA is lower than the lowest number the lab is able to test for. (Currently, that's less than 0.015 ng/mL for the ultrasensitive test used at UCSF and less than 0.1 ng/mL with the regular PSA test used at some other institutions.)
Whether or not you need additional treatment, you should have regular checkups that include routine PSA blood tests (traditionally, every three to four months for the first year, every six months for the second and third year, and then annually). Patients with detectable or rising PSA levels may need more frequent tests. You may also need imaging tests, such as transrectal ultrasound, bone scan, CT, MRI, and (increasingly favored) PSMA PET/CT or MRI scans. PET scans utilizing PSMA or fluciclovine F 18 (Axumin) tracers are newer forms of imaging that are much more sensitive than standard CT, MRI or bone scans.
If prostate cancer recurs after surgery, many treatment options are available, such as radiation or hormone therapy. You and your doctor can discuss what is appropriate for you.
Erectile dysfunction
Erectile dysfunction (ED) is the consistent or recurrent inability to attain or maintain a penile erection. It is a common consequence of prostatectomy. The level of ED that occurs after surgery and level of sexual function recovery depend on many factors, including whether nerve bundles were preserved during surgery; the patient's age, medications and lifestyle; and the presence of other medical conditions, such as diabetes, high cholesterol, depression or anxiety. The return of unassisted sexual function may not begin until six or more months after surgery; however, it usually continues to improve over the next two to three years. Erection recovery sufficient for penetration may continue for 18 to 24 months or even longer, and in many cases the greatest recovery is in the second year. Your doctor can discuss available treatments for erectile dysfunction.
Treatment possibilities depend on whether your nerve bundles were spared. The following advice assumes you had both bundles spared. If you had just one or no bundles spared, talk to your doctor about your options.
You'll leave the hospital with a prescription for an erectile medication, such as Viagra or Cialis. The initial purpose is to get blood flowing to the penis and not necessarily to get erections. Don't be alarmed if after a month of taking the medication, you haven't had an erection. This is common after surgery, but you should still mention it at your follow-up appointment.
In the past, patients were advised to take these medications routinely to restore sexual function ("penile rehabilitation"), but there's no evidence this is more beneficial than taking the drugs as needed (when intercourse is desired). Talk to your doctor about which approach is best for you.
Most insurance plans don't fully cover ED medications, which means you will have to pay out of pocket. It's worth finding out before your surgery. In some cases, insurers will cover the medications if you get prior authorization. We can help expedite that; call us at (415) 353-7171. There are also generic alternatives which might be less expensive depending on your insurance.
At the time of orgasm (with or without an erection), some men notice that they leak urine (this is called climacturia). This problem usually resolves on its own, but emptying the bladder before sexual stimulation may help. If it persists and is of concern, mention it to your providers, as there are other remedies.
Keep in mind that pleasuring, cuddling, and other loving and stimulating activities can still take place, regardless of erectile issues.
ED treatment
At your follow-up visit, you will receive information on treatments that can help with regaining erectile function. These include oral medications but also other options that may be more effective and less expensive over time, such as intra-urethral suppository (Muse), penile injections, vacuum constriction devices, and penile prosthesis. For more information, see Managing Erectile Dysfunction – A Patient Guide.
Oral ED medications
These medications are not an option if you are taking nitrates or alpha-blockers (usually prescribed for chest pain). If you are able to use one, take your ED medication exactly as prescribed by your doctor. We almost always prescribe maximal doses and advise patients to start with half a pill to save a bit on cost. If you're on medication for high blood pressure, wait at least four hours after taking that before taking any ED medication since it can also lower blood pressure. Each type of ED medication comes in various doses, and each has specific considerations.
Check with your health care provider for additional information, and refer to your discharge instructions for dosing tailored to your situation.
Levitra (vardenafil)
- Levitra comes in 5 mg, 10 mg and 20 mg tablets.
- You can't use Levitra if you are taking nitrates or alpha-blockers.
- Start by taking half of one tablet.
- If by two to three months after the surgery, you're having no response and the side effects don't bother you, increase your dose to a full tablet.
- Levitra can be taken independently of food. Note that high-fat meals and alcohol can slow absorption. Take 30 minutes to one hour prior to sexual intercourse.
- Sexual arousal is needed for Levitra to be effective.
- The effects last approximately four hours.
- Common side effects include nasal congestion, facial flushing, headache and indigestion.
- Levitra can also cause cardiac abnormalities.
- Levitra interacts negatively with ketoconazole, itraconazole, ritonavir, indinavir and erythromycin.
- Your doctor may prescribe a reduced dose if you experience bothersome side effects or interactions.
- If the side effects bother you or your response isn't satisfactory, contact your provider using MyChart. Your doctor may consider switching you to a different medication.
Viagra (sildenafil):
- Viagra comes in 25 mg, 50 mg and 100 mg tablets. It's absorbed best on an empty stomach, so wait at least two hours after a meal before taking it.
- You can't use Viagra if you take nitrates or alpha-blockers.
- Avoid alcohol; it slows down absorption and reduces effectiveness.
- Take 30 minutes to one hour prior to sexual intercourse.
- Sexual arousal is needed for Viagra to work.
- The effects last approximately four hours.
- Common side effects include nasal congestion, facial flushing, headache, upset stomach and blue-tinted vision.
- Start by taking half of one tablet on an empty stomach.
- If by two to three months after the surgery, you're having no response and the side effects don't bother you, increase your dose to a full tablet.
- If the side effects bother you or your response isn't satisfactory, contact your provider using MyChart. Your doctor may consider switching you to a different medication.
Cialis (tadalafil)
- Cialis comes in 10 mg and 20 mg tablets.
- You can't use Cialis if you take nitrates or alpha-blockers (unless you're taking Flomax at a dosage of 0.4 mg daily).
- Start by taking half of one tablet.
- If by two to three months after the surgery, you're having no response and the side effects don't bother you, increase your dose to a full tablet twice a week.
- Cialis can be taken without food. Keep alcohol consumption in check as it can slow absorption.
- Take Cialis one to two hours prior to sexual intercourse.
- Sexual arousal is needed for Cialis to work effectively.
- The effects of Cialis can last up to 36 hours.
- Common side effects include headache, indigestion, back pain, flushing, nasal congestion and (especially) muscle aches. Though the medication's effects may last 36 hours, side effects usually resolve after two hours. You can take Tylenol (acetaminophen) or Prilosec (omeprazole) for bothersome side effects.
- If the side effects bother you or your response isn't satisfactory, contact your provider using MyChart. Your doctor may consider switching you to a different medication.
Troubleshooting
Contacting your provider – Minor problems or concerns can be relayed to your doctor during daytime office hours by calling (415) 353-7171, though you may get a faster response by contacting us through MyChart. For urgent issues, you can reach us at any hour, at the same number (415) 353-7171.
Blood in urine – Blood in urine is common and may be intermittent. While you have a catheter, rather than looking at the color of the urine in the collection bag, monitor the color of the urine in the tubing draining the catheter – this represents the urine you are actively making. Pink or light red urine is not concerning; it's just a signal to drink more fluids and decrease activity. Call your doctor about any of the following:
- If your urine is very bloody (like tomato soup or burgundy wine)
- If your catheter isn't draining urine even after you've resolved possible kinks, loops or air locks and checked that the bag is below your bladder
- If you have large blood clots that aren't passing through the Foley catheter tubing
- If your urine is bloody the day before or the day of the scheduled Foley catheter removal (We'll need to reschedule your removal appointment.)
Cloudy urine – This is common and will resolve once the catheter is removed and healing occurs. Nevertheless, you should drink enough fluids to produce clear urine.
Constipation – This is a common side effect of pain medications and surgery. During the time you're on pain medications, increase your fluid intake (drink at least eight glasses of water a day). Take your prescribed stool softeners and laxatives, and eat lots of fiber (whole grains, fruits and most vegetables – avoid cruciferous vegetables while waiting for bowel function to return).
Diarrhea – A change in bowel habits is common after surgery. Although severe diarrhea – defined as more than three loose bowel movements in a 24-hour period – is uncommon, it could indicate an infection. Consult your doctor if you have persistent diarrhea, especially if it's accompanied by increasing abdominal pain, swelling or fever. Diarrhea due to infection can be treated with oral antibiotics.
Diet – There is no specific diet following radical prostatectomy. Patients are able to drink liquids immediately and progress to solid foods within 24 hours in most cases. Patients are encouraged to eat a well-balanced diet. Many find that ingestion of small meals is satisfying after surgery. On occasion, iron is taken to replenish red blood cells. Ask your doctor whether this is necessary. Eat a diet that you find satisfying and palatable. Normal dietary habits will return as healing occurs and you resume normal physical activity. For healthy eating tips, refer to UCSF's Health and Wellness guides for men living with prostate cancer.
Erectile dysfunction – Return of sexual function (having erections) following surgery is dependent on many factors, including surgical technique (whether neurovascular bundles were saved), patient age, preoperative sexual function and overall health (presence of other conditions, such as diabetes and high cholesterol, or a history of smoking). See "Managing Erectile Dysfunction – A Patient Guide" for more information.
Exercise – Walking after the procedure is encouraged. Pain may limit how much you can walk for the first two or three days, but try to increase it thereafter, paying attention to any pain or fatigue. Most patients are walking a block or two within four to seven days. Increase your activity over time, especially once the catheter is removed. Lifting more than 10 pounds should be avoided for four weeks after surgery. Abdominal exercises (such as sit-ups) and cycling on an upright bicycle should be avoided for approximately six weeks. When resuming activities, let pain be your guide. If you overdo it, you may experience more blood in your urine or more incontinence. For more help, refer to "Moving Through Cancer: A Guide to Exercise for Cancer Survivors."
Excessive drain fluid – The drain placed where the prostate was removed is sometimes left in place after the procedure. It will have blood-tinged drainage, which will be tested for urine. If the result is normal or there is little drainage, the drain will be removed before you're discharged from the hospital. On rare occasions, we send patients home with the drain in place. If this is the case for you, we will ask you to record the drainage daily in a diary, which we will provide at the time of discharge.
Fever – A persistent temperature above 101 F (38 C) is not normal. If you have a fever, call your doctor. However, a short-lived temperature elevation may be a result of shallow breathing. If that is the case, use the incentive spirometer that was given to you at the hospital.
Leakage around the catheter – Passage of small amounts of blood, urine or thick secretions around the catheter is common and no cause for alarm. Wash the area with soap and water daily.
Pain – Pain along the incision is to be expected but should be effectively managed with pain medication. Call your doctor if your pain is not controlled. On occasion, patients with catheters in place may develop bladder spasms. These are characterized by intermittent episodes of pain just above the pubic bone, often radiating down the penis and often associated with passage of urine around the catheter. Spasms will resolve once the catheter is removed. If they occur frequently or are very painful, use Ditropan (prescribed to you at discharge) to control them. Remember to stop taking it 24 hours before your catheter is removed.
Poor urinary flow – The quality of the postsurgical urinary stream varies from patient to patient. For most, it is stronger than before the procedure. On occasion, it may appear weaker. Rarely, the anastomosis (area where the urethra was sutured together after prostate removal) will narrow, making urination difficult. If this occurs, you may need a procedure to dilate (gently stretch) the urethra. Call your doctor if the strength of your stream is intermittent or so weak that you must strain.
Redness along the incisions – Some degree of redness is expected during the healing process, but it shouldn't be excessive (extending beyond the incision more than a few millimeters) or expanding. Call your health care provider if you note increasing redness, especially if it's associated with fever, increasing pain in the area, or thick, purulent drainage (pus).
Swelling or bruising of the scrotum or penis – This is common after the procedure. It is usually limited and will resolve with time. Elevation of the scrotum with a rolled towel while in bed helps some patients, and you can apply an ice pack or a bag of frozen peas wrapped in a towel at the scrotum to reduce swelling. Wearing underwear with scrotal support can also help. While your catheter is in place, avoid sitting for periods longer than 30 to 45 minutes.
Swollen legs – Some patients notice mild swelling of the ankles after surgery due to the large amount of intravenous fluids that may be given during surgery. However, it's unusual for one calf or ankle to swell more than the other. If one side is more swollen than the other, contact your health care provider. Rarely, patients may develop blood clots in the legs after surgery. Walking and periodic elevation of your legs can help prevent this.
Urgent signs and symptoms
For emergencies that can't wait, call 911.
Call us immediately at (415) 353-7171 (staffed 24/7) if you experience any of the following:
- You have a persistent or recurring temperature greater than 101 F (38 C) or repeated chills.
- Your catheter stops draining urine despite adequate hydration (fluid intake) and no kinks in the tubing.
- Your urine in your Foley catheter is cloudy, foul smelling or persistently bloody (dark red or with large clots).
- You have no bowel movement by day five after surgery.
- You have an unexplained severe pain that you didn't experience while in the hospital.
- You are nauseated or vomiting.
- You have asymmetrical leg swelling (one leg more swollen than the other).
- You have worsening redness, swelling or drainage from your incisions.
More information
You can access our patient education library online or reach urologic surgical oncology at the UCSF Prostate Cancer Center by calling (415) 353-7171.
Important note:
Regarding the content of this document, all medical advice, instructions and information (including references to medications, rehabilitation techniques, time frames and products) are based on standards prevailing at the time of publication. The reader is cautioned to verify current applicability before acting.
The surgery can be done through an "open" incision made in the abdomen (a procedure called a radical retropubic prostatectomy) or through an incision in the perineum, the area between the scrotum and the anus (radical perineal prostatectomy). These approaches are no longer commonly used in most high-volume U.S. centers for prostate cancer care.
Alternatively, the surgery may be done as a laparoscopic radical prostatectomy. Laparoscopy is a minimally invasive technique in which surgery is performed by passing slender, specially designed telescopes and other fine instruments through very small incisions.
At UCSF, we perform laparoscopic radical prostatectomies using the da Vinci robotic-assisted surgical system, which features excellent magnification and surgical precision. In terms of cancer control and preservation of urinary and sexual function, outcomes for patients are as good as – and often better than – those obtained via open radical retropubic prostatectomy. The robotic approach appears to remove the cancer equally well and is associated with less blood loss and discomfort, fewer complications and an earlier return to normal activities. This approach also may be associated with an enhanced ability to spare the neurovascular bundles that control erectile function. Depending on age and other factors, patients may be candidates for a nerve-sparing radical prostatectomy, which helps maintain sexual function.
In addition to removing the prostate gland, we may remove the lymph nodes draining the prostate. Called pelvic lymph node dissection, this would be done to determine whether the cancer has spread to the lymph nodes. The risk of having cancer in the lymph nodes relates to the cancer's severity.
Major complications from the surgery are rare, but there are side effects. The most common ones are incontinence (leakage of urine, usually with stress or activity) and erectile dysfunction (inability to get or maintain an erection). The incontinence, though common early after surgery, usually goes away. Whether erectile function returns depends on whether the nerves surrounding the prostate can be spared at surgery, patient age and baseline function. Men who are older or already have erection problems are most likely to have erectile dysfunction afterward.
Compared with other treatment options, radical prostatectomy offers several advantages:
- Many patients – though not all – are cured by the surgery.
- Removal of the entire prostate gland allows the pathologist to more accurately assess the cancer's aggressiveness (stage and grade). This information can help determine a course of treatment if at some point additional treatment is recommended. Such information is also used to determine the frequency of prostate-specific antigen (PSA) testing after surgery.
- It quickly becomes clear whether the treatment was effective. Following surgery, the patient's serum PSA level is usually undetectable; so through regular PSA monitoring, any recurrence can be detected early. At UCSF, we use an ultrasensitive PSA test that can detect levels as low as 0.015 ng/mL, aiding in early detection. With radiation or other primary treatments, assessing effectiveness can take a considerable period of time.
- You still have the opportunity to consider salvage (follow-up) treatments with radiation or other modalities. While surgery does not preclude subsequent radiation therapy, surgery following radiation treatments may be difficult. Having this option of additional treatments later on is especially important for higher-risk cancers, where a combination of treatments may be necessary for long-term survival.
- There is a relatively limited risk of recurrence (beyond five years), which can be detected with appropriately timed PSA testing.
Nonetheless, radical prostatectomy is just one of many treatment options. You should discuss all options with your doctor or cancer care team.
(Article continues below.)
Recommended reading
Related treatments
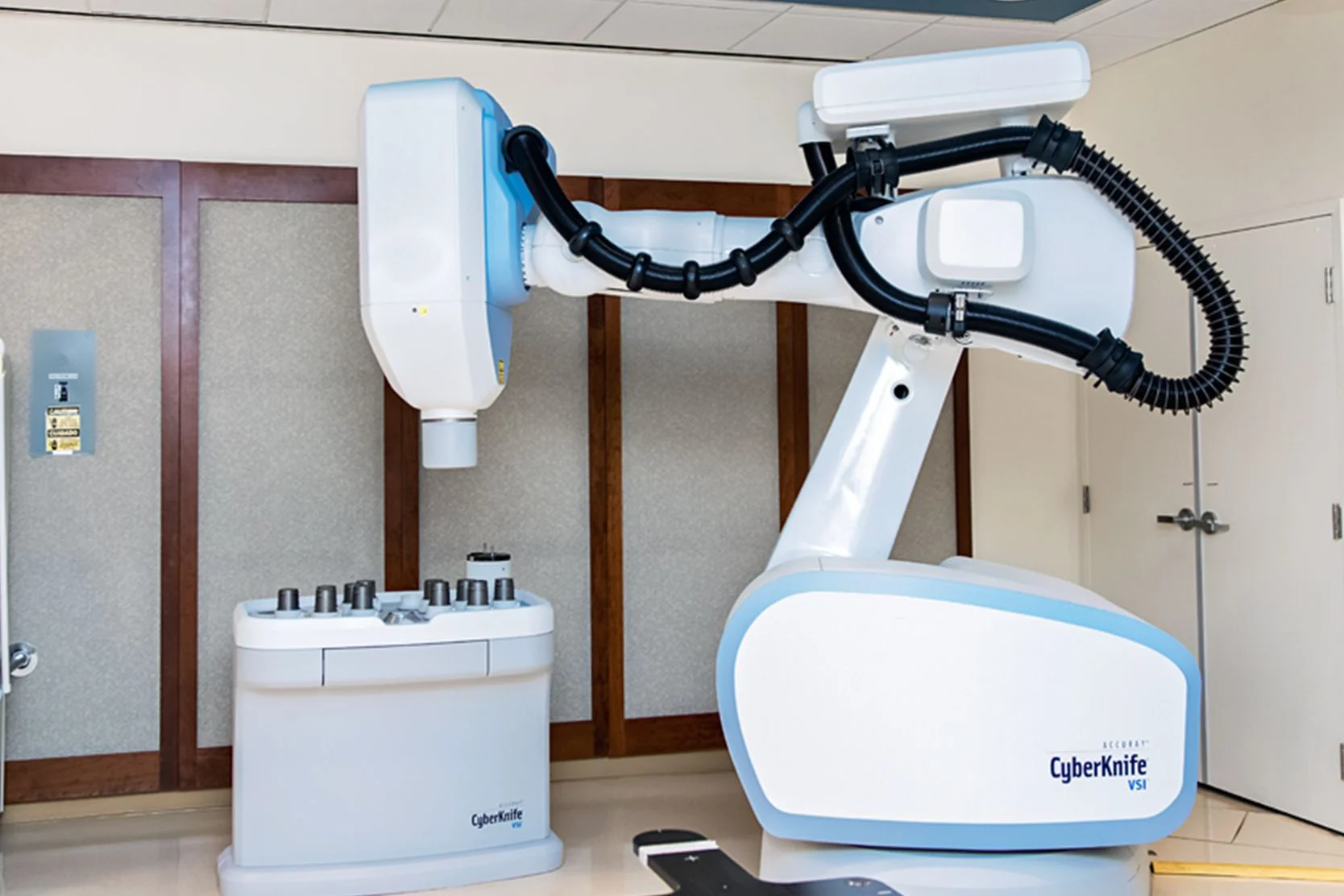
Cyberknife
The CyberKnife one of the most advanced forms of radiosurgery is a painless, non-invasive treatment that delivers high doses of precisely targeted radiation
Intensity Modulated Radiation Therapy
IMRT is the most advanced form of 3-D conformal RT, allowing for higher, more effective doses of radiation.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.




