Ross Procedure
On this page
The Ross procedure is a surgical treatment for a diseased aortic valve. One of the heart's four valves, the aortic valve controls the flow of oxygen-rich blood out to the body. If the valve becomes narrowed, a condition known as aortic stenosis, the heart has to work harder to pump, causing the muscle to thicken and potentially leading to heart failure. If the aortic valve becomes leaky, a condition known as valve regurgitation, blood can back up into the heart, which also can eventually cause heart failure.
The standard treatment for either condition is to replace the faulty valve with a prosthetic one that is either mechanical (made from a durable material, such as titanium) or made from animal tissue. But neither is a perfect solution. Tissue valves wear out and have to be replaced, while mechanical valves are prone to blood clots, which means patients with them have to take blood-thinning medications for the rest of their lives.
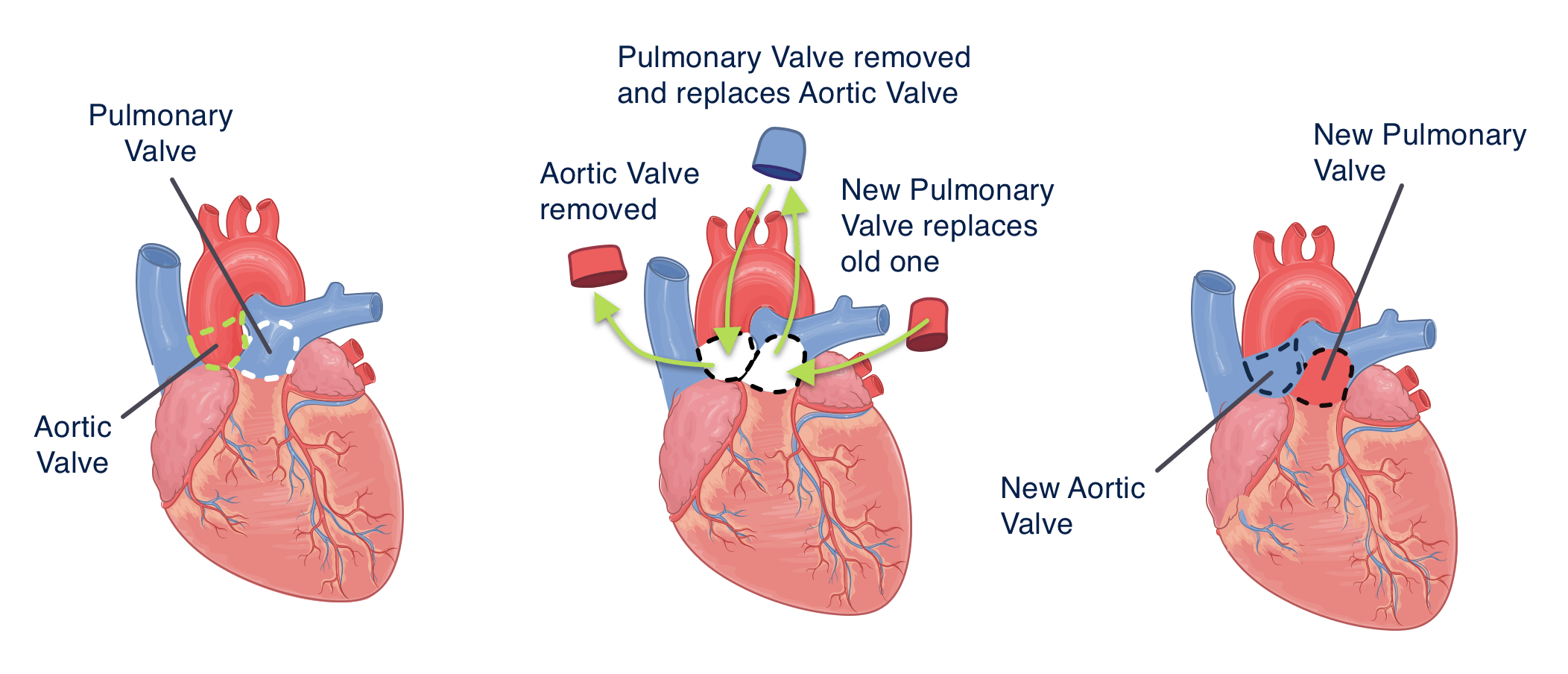
The Ross procedure provides another option. The surgeon replaces the diseased valve with another of the patient's own heart valves, the pulmonary valve. The swap works because the pulmonary valve is similarly shaped and can become thick and strong enough to function like an aortic valve. The pulmonary valve, in turn, is replaced with a valve from a cadaver donor.
For certain patients, the Ross procedure offers many advantages over standard valve replacements. Although it's a more complicated surgery, the procedure has a lower risk of infection, bleeding, clotting and stroke. There's no risk of the valve not fitting the patient's anatomy – a common problem with prosthetic valves. Also, the valves are more durable than animal tissue prosthetics and don't require the patient to take blood-thinning drugs.
These advantages are most meaningful for younger patients. Elderly patients (those over 70) generally fare well with prosthetic valve replacements; the treatment nearly restores their normal life expectancy. In patients 60 and under, however, life expectancy is reduced with the standard valve replacements. The Ross procedure is the only type of aortic valve replacement to restore normal life expectancy in younger patients.
Who may benefit
The Ross procedure is for younger patients with aortic valve disease but no other major medical problems, such as significant liver, kidney or lung disease. We generally perform the procedure only in those around age 60 and under.
Others who may benefit from the procedure include:
- Women who plan to have children
- Patients who are experiencing a failed valve from a previous aortic valve replacement
- Those with a very small aortic valve in need of replacement (often women and children)
The treatment isn't an option for patients over 70 or people with Marfan syndrome; pulmonary valve disease; autoimmune disorders, such as lupus; or significant kidney, liver, lung, coronary artery or mitral valve disease.
Advantages
The Ross procedure's advantages over standard valve replacements include:
- The valve lasts longer than an animal tissue valve.
- Compared to a tissue valve, the relocated valve has a lower risk of postoperative deterioration from calcification (tissue hardening caused by calcium deposits).
- No need to take blood thinners (unlike with mechanical valves).
- Decreased risk of valve infection, bleeding or stroke.
- Decreased chance that the body will reject the valve.
- Easier blood flow regulation.
- Restores normal life expectancy to patients under 60.
Evaluation
To determine whether you're a candidate for the Ross procedure, your doctor will assess the condition of your aortic valve and your overall cardiovascular health, generally with the help of one or more of the following tests:
- Echocardiogram. Also called a heart ultrasound, this noninvasive test uses sound waves to produce detailed images of your heart, allowing doctors to assess the structure of its chambers and valves and observe blood flow. In a transthoracic echocardiogram, the images are captured by placing a transducer (the device emitting sound waves) in various spots on the chest and abdomen. In a transesophageal echocardiogram, a thin tube conveys a transducer down the esophagus, allowing doctors to obtain images from inside the body.
- Coronary CT angiogram. This noninvasive test uses X-rays to create images of the blood vessels in the chest, including the aorta and the pulmonary artery.
- Coronary angiogram. A catheter (a thin, flexible tube) is threaded through a blood vessel in your wrist or groin to an artery in your heart, and a harmless dye that shows up well on X-rays is injected into the catheter. The test provides detailed images that reveal how well the coronary arteries are functioning and also allows doctors to measure the pressure inside the heart chambers.
Procedure
The Ross procedure is open-heart surgery, requiring general anesthesia (you're completely asleep). The surgeon cuts through the breastbone to access your heart. Because your heart must be temporarily stopped, you are placed on a heart-lung bypass machine, which keeps the blood circulating through your body. The surgeon inspects and removes the diseased aortic valve, then examines the pulmonary valve to check that it's a healthy and suitable replacement. If it is, the valve is removed and implanted in place of the aortic valve. The surgeon then implants a donor pulmonary valve. The operation typically takes four to five hours.
Recovery
Expect to spend five to seven days in the hospital, the first two or three of those in intensive care. We encourage you to be up and walking within 24 hours of the surgery; most patients are able to do so. During your post-op stay, follow-up tests are performed to determine that your heart valves are functioning properly. These may include chest X-rays, blood tests, an electrocardiogram (EKG) and an echocardiogram.
Before you go home, your heart care team will talk with you about how to care for yourself, providing instructions on diet, exercise, care of your incision site, and use of current or new medications.
We recommend six weeks of restricted activity while you recover from the surgery. For part of that time, we may also prescribe certain medications, including:
- Diuretics (drugs that increase urination), so you won't retain water
- Pain medicine, in gradually decreasing amounts
- Beta-blockers to help keep your blood pressure low while your pulmonary valve "learns" how to be an aortic valve
- ACE (angiotensin-converting enzyme) inhibitors, for additional blood pressure control or if you had severe valve regurgitation with a dilated left ventricle
Risks
Though the Ross procedure's results hold up well over time, there is about a 1% per year chance of needing another procedure to fix issues with the aortic or pulmonary valve. (That's better than treatment with tissue valves but more frequent than with mechanical valves.) About half the time, we can address the problem without open-heart surgery, and half the time, patients need another open-heart surgery. However, of the four main complications that can occur after aortic valve surgery – namely, reoperation (having another surgery), bleeding, infection and stroke – reoperation has the lowest risk.
Related services & conditions
Specialties
Conditions
- Aortic Valve Disease
- Aortic Regurgitation
- Aortic Stenosis
Treatments
- Aortic Valve Replacement
- Aortic Valve Surgery
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
