ACL Injury
On this page
Overview
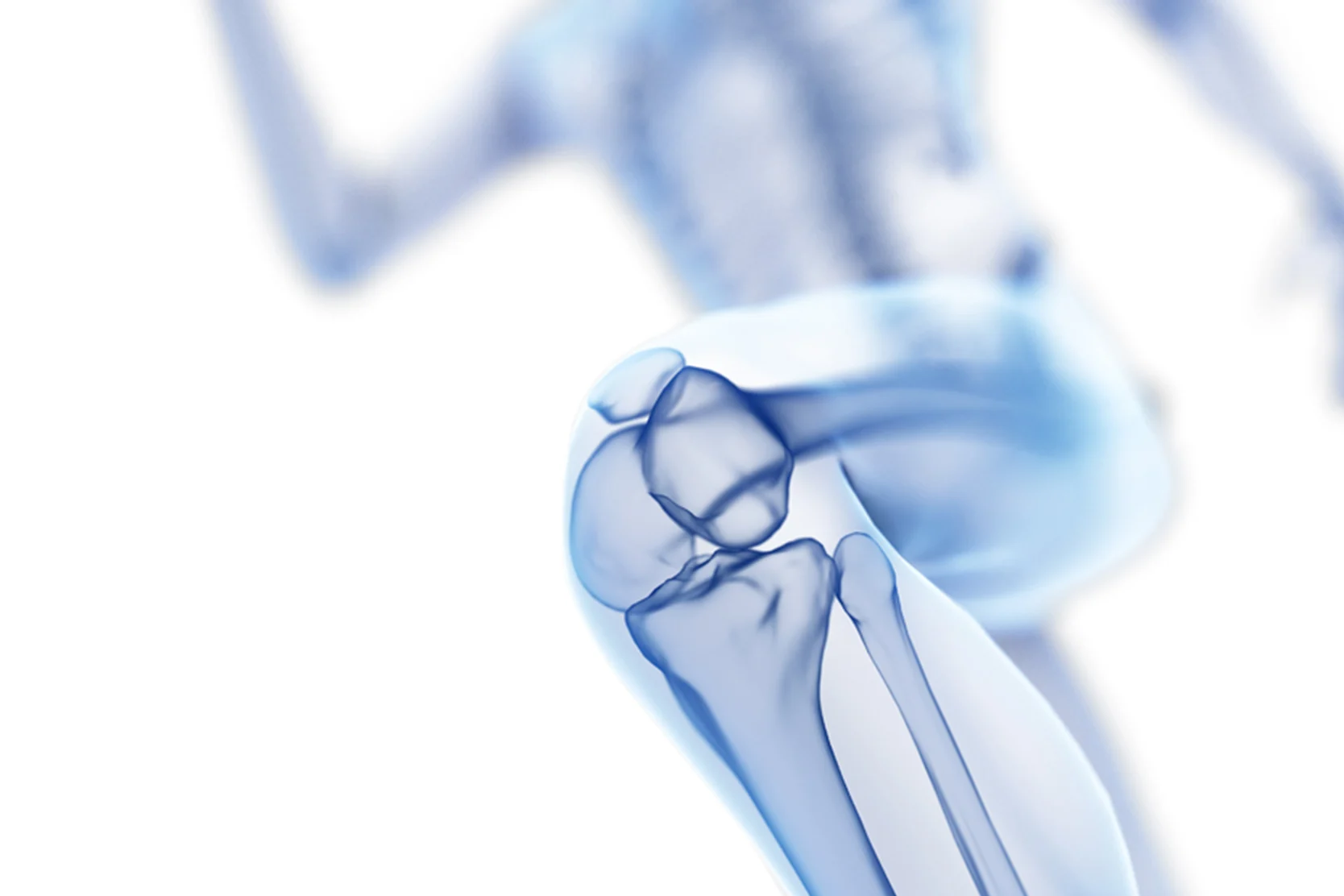
The anterior cruciate ligament (ACL) is one of the knee joint's four major ligaments, which work together to coordinate function and promote stability. A ligament connects one bone to another. Running from the back of the femur (thighbone) to the front of the tibia (the larger long bone of the calf), the ACL prevents forward movement of the tibia and provides rotational stability to the knee.
ACL injuries commonly occur during exercise or sports, most often during a noncontact event, such as a quick change of direction in soccer. A smaller percentage of ACL injuries result from direct contact with another player or object. Several studies have shown that females have a higher incidence of this injury than males, especially in certain sports. It's been proposed that this is because of differences in physical conditioning, muscular strength, neuromuscular control and bone alignment, as well as women's looser ligaments and the effects of estrogen on ligament properties.
The classic ACL injury occurs when decelerating, stopping suddenly, twisting or jumping. People often hear or feel a pop at the moment of injury and sometimes experience a brief hyperextension of the knee joint. Immediately afterward, some people are able to continue their activity, but most are not. A few hours later, the knee will be considerably swollen.
Our approach to ACL tears
UCSF is committed to helping patients with ACL tears return to the highest level of activity possible, whether that means a daily walk or reporting for practice with the NFL. Our team includes orthopedic surgeons, primary care sports medicine doctors, physical therapists and athletic trainers. These specialists work together to tailor a treatment plan that supports each patient's needs and goals.
Signs & symptoms
Patients with ACL tears often:
- Hear or feel a pop at the moment of injury
- Experience immediate swelling
- Feel as though their knee will give out or is unstable, especially when turning, pivoting, sidestepping and going downstairs
- Experience lingering instability of the knee
Diagnosis
To detect an ACL injury, doctors examine the knee for range of motion, swelling, stability and ligament integrity, and assess lower body strength. X-rays may be used to check for injuries to bone, and an MRI scan can help with assessing the injury's severity and detecting associated problems, such as sprains of other knee ligaments, meniscus tears or articular cartilage damage.
Treatments
Most ACL tears are treated with reconstructive surgery, but depending on the patient's age, degree of injury, activity level and recovery goals, a nonsurgical approach is sometimes chosen. Patients choosing between these options will benefit from a collaborative decision-making process with their doctors and physical therapists.
For patients who aren't very physically active or don't participate in sports that involve quick changes in direction, a physical therapy treatment plan (instead of ACL reconstruction surgery) is a reasonable option, as the injury may not interfere with their daily activities. The regimen takes six to 10 months and can restore knee stability to a point where it's close to the pre-injury state. Using a hinged knee brace (ACL functional brace) can help prevent episodes of instability during this period and support a safe return to low-stress sporting activities.
Unfortunately, many people who decide against surgery may experience a secondary injury to the knee due to repetitive instability episodes and altered biomechanics. Patients who have had an ACL tear that do not have ACL reconstruction surgery may be at a higher risk of further injury to the meniscus and cartilage. Rarely, some people with an ACL tear are able to participate in sports without symptoms of instability. This variability is related to the severity of the original knee injury, as well as to the specific activities an individual usually engages in.
Preparing for surgery
The decisions you make and actions you take before your surgery can be as important as the procedure itself in ensuring a healthy recovery.
Prepare. Make sure you understand the potential risks and benefits of the surgery you'll be having. Ask your surgeon any questions you have. Talking with someone who has undergone the procedure can also be helpful.
Talk to your surgeon. Tell your surgeon about your health problems – everything from a recent fever or infection to a chronic condition such as asthma or sleep apnea – and about any medications you take. Your surgeon will review your health history at your pre-op appointment.
Follow instructions. You'll be instructed not to eat or drink after midnight on the night before your surgery. This reduces the risk of vomiting while under general anesthesia, which can lead to complications. Don't drink alcohol, smoke or take recreational drugs prior to surgery.
Arrange transportation. You'll need someone you know to drive you home a few hours after your surgery, since the anesthetic and pain medications will make you drowsy. You won't be allowed to leave the hospital on your own.
Practice using crutches. Learn to use crutches before you actually need them. Your physical therapist or the athletic trainer on your care team can instruct you on proper technique at your pre-op appointment.
Dress comfortably. On surgery day, wear loose pants or other clothing that will fit comfortably over your knee bandages and post-op brace.
Relax. Keeping a good frame of mind can ease any anxiety you have about undergoing surgery. Distractions such as reading, listening to music or podcasts, or practicing mindfulness mediation can help.
Take care of your knees
Although knee ligament injuries are common, you can take steps to reduce your risk:
- Manage your weight. Every pound in excess of your normal weight puts 3 or 4 additional pounds of pressure on your knee with every step.
- Keep your legs strong. The hamstrings (the muscles of the back of the thigh) and the quadriceps (those at the front) are crucial shock absorbers. Keeping these muscles strong and flexible protects the surfaces of your knee joints.
- Stretch your muscles. Stretching before exercise should be a regular part of your warm-up. However, it's also important not to overstretch. Never use your hands to push or pull beyond what's comfortable, and avoid squatting during your warm-up, which can stress your knee joint.
- Wear proper shoes. Well-fitting athletic shoes with suitable cushioning or support can reduce the impact on your knees.
- Ease into shape. If you want to take up activities that require twisting and turning – such as racket sports, skiing, soccer or basketball – don't assume you can play yourself into shape. Develop your fitness and strength before you get active in sports that are hard on knees.
Frequently asked questions
Awards & recognition

Best in Northern California and No. 6 in the nation for orthopedic care
Recommended reading
Helpful resources
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.