Amyloidosis
On this page
Overview
Amyloidosis is a group of diseases in which abnormal proteins, called amyloid proteins, accumulate in organs or organ systems such as the heart, kidneys, nervous system or gastrointestinal tract. There are different types of amyloidosis, dependent on the type of protein being deposited in tissues.
The most common form of amyloidosis in the United States is called primary amyloid. In primary amyloid, the protein being deposited is a part of the antibody protein called the light chain.
Primary amyloid is now a treatable disease. The mainstays of therapy are the same agents used to treat a related bone marrow cancer, called multiple myeloma. Treatment options include chemotherapy, corticosteroid medicines, biologic agents, and in some instances, autologous stem cell transplantation. The goal of therapy is to halt the buildup of amyloid protein in organs and to prolong life.
Fortunately, amyloidosis is rare, affecting about eight out of every 1 million people annually. The majority of those affected are more than 40 years of age and 60 percent are male, although the condition can affect anyone. The cause is unknown.
Types of amyloidosis
There are three main types of amyloidosis:
- Primary amyloid This is a plasma cell disorder originating in the bone marrow. Abnormal cells produce antibody proteins which deposit as amyloid. It is the most common type of amyloidosis in the United States, affecting 2,000 people each year.
This condition, which is usually treated with chemotherapy, is not considered to be a type of cancer. However, it may be associated with multiple myeloma, which is a type of bone cancer. The severity of the illness often depends on the number and extent of organ involvement. - Secondary amyloid This condition is caused by a chronic infection or inflammatory disease such as rheumatoid arthritis, familial Mediterranean fever (an intestinal disorder), osteomyelitis (infection of bone) or inflammatory disorders of the bowel. The amyloid deposits in this type of the disease are made up of a protein called the AA protein. Medical or surgical treatment of the underlying chronic infection or inflammatory disease can slow or stop the progression of this type of amyloid.
- Familial (or hereditary) amyloid This rare form of amyloid is the only type that is inherited. It affects families of nearly every ethnic background. The deposits in this type are most commonly made up of the transthyretin protein produced in the liver. The condition results from a mutation in this protein. Liver transplant is used to cure this form of amyloid.
Our approach to amyloidosis
UCSF is dedicated to delivering the most advanced treatment options for amyloidosis with care and compassion. There are several types of amyloidosis, and the best therapy depends on the type and severity of the patient's condition. Treatments range from medications such as antibiotics to stem cell or liver transplants.
We are also dedicated to discovering even better treatments for amyloidosis through research. Interested patients may have the option to participate in clinical trials, which evaluate potential new therapies.
Signs & symptoms
Symptoms of amyloidosis depend on the organs it affects. The wide range of symptoms often makes amyloidosis difficult to diagnose. Some people may not experience any symptoms and others may have many symptoms. Frequently described symptoms include:
- Weakness
- Weight loss
- Shortness of breath
- Numbness or tingling in the hands or feet
- Diarrhea
- Severe fatigue
- An enlarged tongue
- Feeling full after eating smaller amounts of food than usual
- Dizziness upon standing
- Swelling of the ankles or legs
- Fainting spells
- Palpitations of the heart
Based on the organs involved and the resulting symptoms, amyloidosis can cause particular groups of symptoms, referred to by doctors as syndromes. These include:
- Congestive heart failure, or the inability of the heart to pump enough blood to meet the body's needs.
- Nephrotic syndrome, the excess loss of protein through the kidneys
- Autonomic neuropathy, or nerve damage that affects involuntary body functions such as heart rate and perspiration.
- Peripheral neuropathy, or nerve damage that affects the peripheral nervous system (PNS). The PNS relays information between the brain and the spinal cord and the rest of the body.
- Malabsorption, or problems absorbing nutrients from food.
Diagnosis
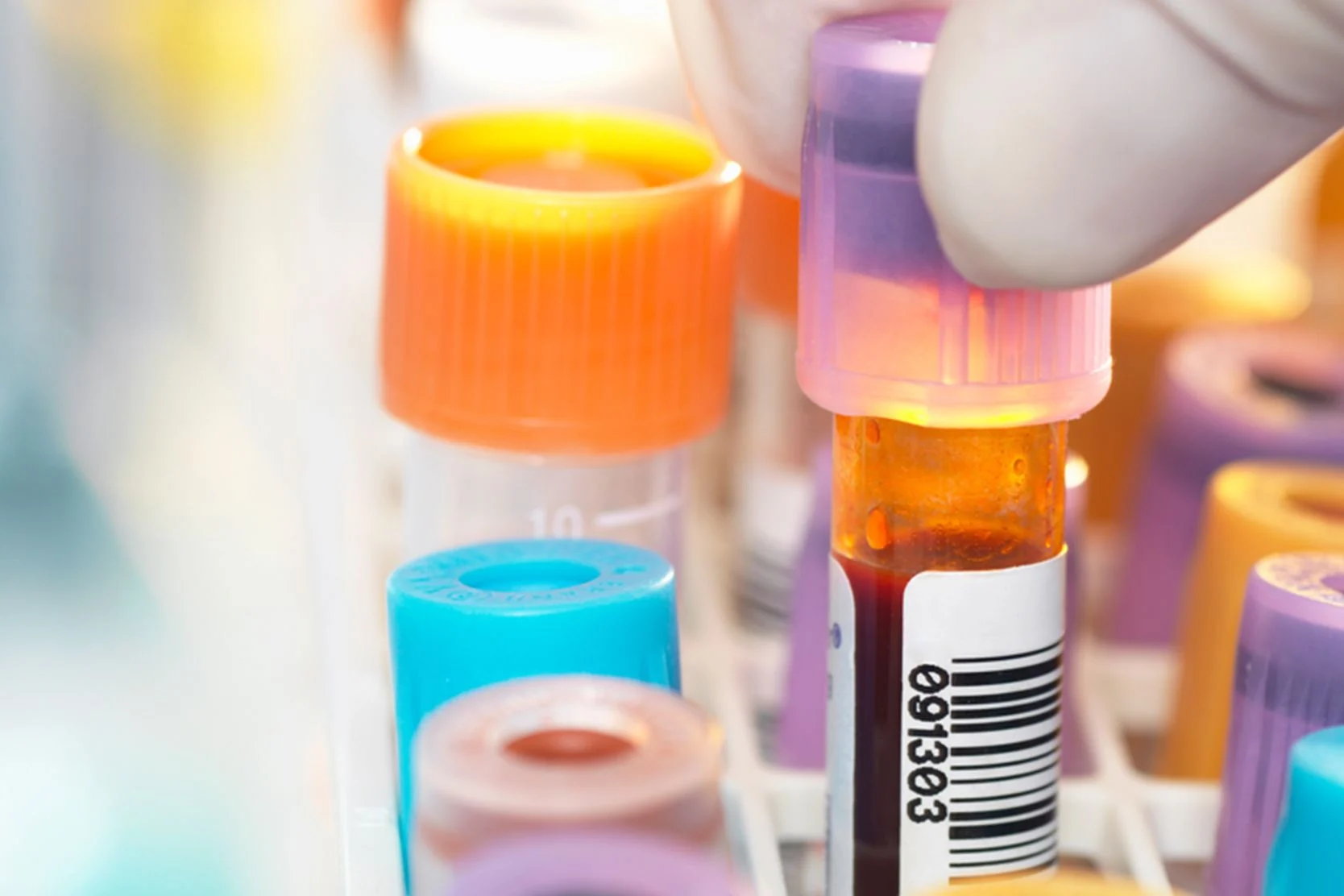
A complete medical history and physical examination is essential for diagnosing amyloidosis. Blood, urine and bone marrow tests also must be performed. Blood or urine tests can detect the amyloid proteins, but only bone marrow tests or other small samples of tissue — called biopsies — can positively establish the diagnosis of amyloidosis.
A small tissue sample, or biopsy, will often be taken from the abdominal fat, rectum, and/or bone marrow to confirm the diagnosis of amyloidosis. These biopsies are relatively minor procedures done in an outpatient clinic with a local anesthetic (numbing medication). Occasionally, samples need to be taken from damaged organs such as the liver, intestines, heart or kidney. The type of biopsy procedure required will vary from patient to patient.
Treatments
Treatment of amyloidosis is given to improve symptoms and extend life. Treatment can limit further production of amyloid proteins and, in some instances, promote the breakdown of amyloid proteins in affected organs. The type of treatment required varies depending on the type of amyloidosis and the patient's symptoms.
With secondary amyloid, the main goal of therapy is to treat the underlying condition — for example, taking an anti-inflammatory medication for rheumatoid arthritis or antibiotics for an infection.
In hereditary amyloid, liver transplantation has been the most effective therapy. The new liver does not produce the abnormal amyloid proteins and consequently the disease improves. Investigational drugs are also being evaluated to try and prevent this type of amyloid protein from depositing in organs.
For primary amyloid, treatments include the same agents used to treat multiple myeloma, such as chemotherapy, corticosteroid medicines (lenalidomide or thalidomide) and/or bortezomib (Velcade). These treatments slow organ deterioration and some have been shown to prolong life, but none provide a cure.
Because primary amyloid is such a difficult disease to treat and survival is limited, researchers have begun to investigate the use of high-dose chemotherapy with autologous stem cell transplantation as a means of prolonging survival. The initial results with autologous stem cell transplantation are encouraging.
Autologous stem cell transplantation
Patients with primary amyloid undergo an extensive work-up to evaluate organ function and the effects that amyloidosis has had on the body. Those with adequate heart, liver and lung function are encouraged to proceed to autologous stem cell transplantation.
High-dose melphalan chemotherapy is administered over one day. Then the patient's own stem cells (bone marrow) are re-administered two to three days later. An additional three to four weeks are spent in the hospital awaiting recovery and growth of the bone marrow.
The hope is that this therapy will delay progression of the disease, and in some cases, improve symptoms through removal of the abnormal proteins from the organs. However, this therapy is not a cure, and amyloidosis will return in everyone. That said, we have had patients who have been successfully treated with stem cell transplantation and when their disease progressed, have been able to receive another stem cell transplant.
Several new investigational agents are being evaluated in the treatment of multiple myeloma, another plasma cell disorder. The hope is that some of these agents also may be effective in treating amyloidosis. For patients who are not candidates for stem cell transplantation, these agents may prove to be the best available treatment.
Patients with hereditary amyloid should be referred to the Liver Transplant Clinic for evaluation.
Recommended reading
Autologous Transplant Guide
A blood and marrow transplant (BMT) can be challenging. This comprehensive guide can help you or a loved one prepare for the procedure.
Hematology and BMT Resource Guide
Learn about hematology conditions and bone marrow transplant (BMT), connect with support groups and find resources that can promote healing and well-being.
Related services & treatments
Specialties
Conditions
Treatments
- Autologous Stem Cell Transplant
- Liver Transplant
- Cancer Chemotherapy
- Biological Targeted Therapy
- Clinical Trials
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.




