Pacemaker
On this page
What is a pacemaker?
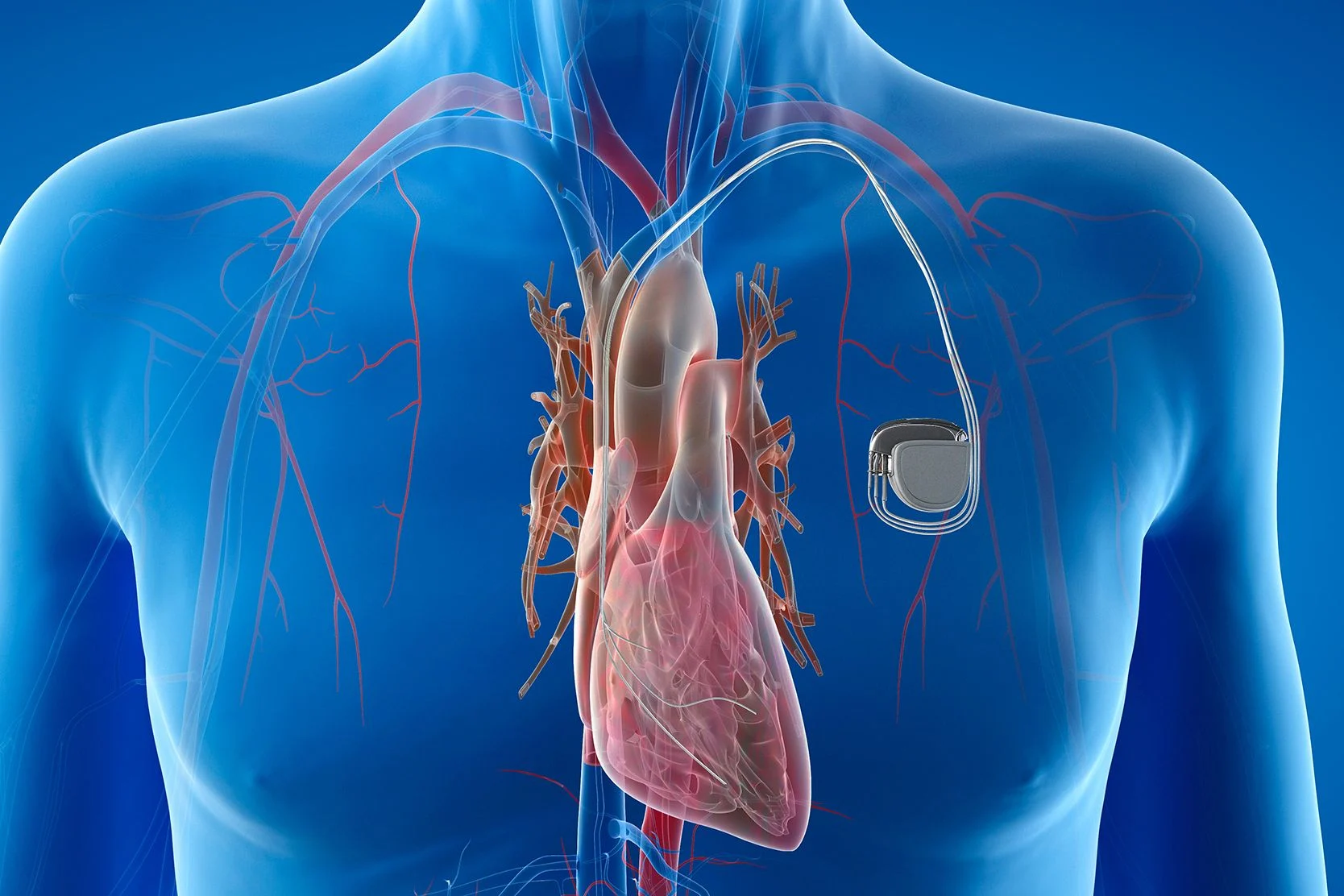
A pacemaker is a small device implanted in the chest to help control your heartbeat. It's used when the heart beats too quickly, too slowly or irregularly due to a heart attack, heart failure or other problem that has damaged the heart's natural electrical system. A pacemaker mimics that system by sending out painless electrical signals that stimulate heart muscle contraction – the first part of the heart's pumping action.
What are the benefits of a pacemaker?
A pacemaker can relieve the symptoms of a slow or unsteady heartbeat, such as:
- Dizziness
- Fainting episodes
- Shortness of breath
For people with certain heart rhythm irregularities, pacemakers can be lifesaving.
How does a pacemaker work?
A pacemaker is battery powered. Most have two parts, the pulse generator and the lead. The pulse generator is a matchbox-sized metal container that holds the battery and electronics. The lead is a thin wire that conducts electrical signals.
Most pacemakers are placed under the skin of the chest and connected to the heart via one, two or three leads. But there are also leadless pacemakers, which are placed directly in the heart.
Pacemakers are usually implanted permanently. But, they're sometimes used as a temporary measure to stabilize heart rhythms in people recovering from a heart attack, heart surgery or a medication overdose that slowed their heart rate.
Awards & recognition

Rated high-performing hospital for pacemaker implantation

One of the nation's best for heart & vascular care
Evaluation for pacemaker surgery
To determine whether a pacemaker is appropriate for your condition, the doctor will check for certain health issues that may have damaged your heart's electrical system. These include:
- Age-related changes in your heart
- Coronary artery disease
- Previous heart attack
- Heart block (also called atrioventricular or AV block)
As part of your evaluation, you may have the following tests:
- Electrocardiogram (ECG). This is a painless test that records the electrical activity of your heart and detects abnormal rhythms.
- Echocardiogram. Using sound waves to create images of your heart, this test can show blocked blood flow.
- Stress test. This test monitors your heart's ability to function during exercise.
- Holter monitor. This portable ECG is worn for 24 to 48 hours to continuously record how your heart functions during your daily activities.
- Zio patch. Another type of portable monitor that can record your heart's rhythm for up to two weeks.
Based on your test results and symptoms, your doctor will determine whether a pacemaker is right for you and, if so, which type.
Types of pacemakers
There are several types of pacemakers, each designed to treat a category of heart condition. Our heart team is experienced in implanting every type.
- Single-chamber pacemaker. This pacemaker has a single lead that connects to the heart's lower right chamber (ventricle) or upper right chamber (atrium).
- Dual-chamber pacemaker. Two leads connect to both the upper and lower chambers on the heart's right side. This device helps control the timing of contractions between the chambers.
- Biventricular pacemaker. Three leads connect to both chambers on the heart's right side plus the heart's lower left ventricle. This type of pacemaker can regulate the heartbeat of some people with advanced heart failure.
- Pacemaker plus an implantable cardioverter-defibrillator (ICD). An ICD can shock your heart back to a normal rhythm if it becomes dangerously irregular.
- Leadless pacemaker. This pacemaker is implanted inside the heart through a minimally invasive procedure.
Your doctor will recommend the best type for you based on your symptoms and specific heart condition.
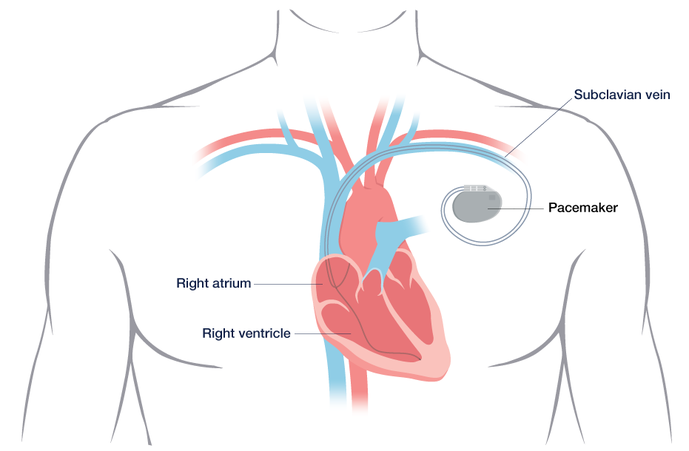
Pacemaker implantation procedure
The procedure to implant a pacemaker depends on which type is used.
Implanting a pacemaker with leads
This is a one- to three-hour surgery that requires general anesthesia. The surgeon makes a small incision just below your collarbone, then inserts the lead through the incision and into a nearby vein. Guided by X-ray images, the surgeon threads the lead to your heart and secures it at one end with a tiny screw; they attach the other end of the lead to the pacemaker.
Your doctor then programs the pulse generator and places it under the skin of your chest, near the collarbone. You may see a bump under the skin where the device is located.
Implanting a leadless pacemaker
A leadless pacemaker implantation is a minimally invasive procedure, in which the surgeon uses a thin, flexible tube called a catheter to access the heart.
After giving an injection to numb the area, the surgeon inserts a catheter containing the pacemaker into a blood vessel in your groin. Then, they thread the catheter through this vessel to the lower right chamber of your heart, release the pacemaker and attach it to heart tissue. Once it's in place, they remove the catheter.
Recovery from pacemaker surgery
Immediately after your procedure, you'll be briefly monitored in a post-op area.
Most people spend the night in the hospital, but some patients can go home the day of the procedure. Before you leave, your doctor will make sure the pacemaker is programmed properly for your needs.
For the next month, you should avoid exercising intensely and lifting anything heavier than 10 pounds. If you experience discomfort, you may need to take over-the-counter medications. Ask your doctors which pain relievers are safe for you.
You will be scheduled for a one-week checkup to make sure your incision is healing well. This visit may be in person or via video. About one month after the procedure, you'll have a follow-up visit with your doctor.
You will be monitored by our device clinic or your local doctor. We'll provide you with special equipment to connect your pacemaker to a phone line for remote testing to make sure everything is functioning properly and monitor for abnormal heart rhythms. The pacemaker can be reprogrammed as needed.
Complications from pacemakers
In general, any complications from a pacemaker are from the surgery to place it. Most are temporary, and serious complications are rare. Complications may include:
- Allergic reaction to anesthesia
- Bleeding
- Bruising
- Damaged nerves or blood vessels
- Infection at the incision site
- Collapsed lung (very rare)
- Punctured heart (very rare)
Electrical interference with your pacemaker
Modern pacemakers are less sensitive to other electrical devices than older models, but certain appliances or machinery can still cause interference. For example, you should avoid:
- Keeping a phone in a pocket over your pacemaker
- Prolonged standing near appliances, such as microwave ovens
- Prolonged exposure to a metal detector
- High-voltage transformers
Your doctor will give you thorough instructions on how to avoid electrical interference with your pacemaker.
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
