Cholangiocarcinoma
On this page
Overview
Cholangiocarcinoma is a rare cancer found in the tissue of the bile ducts, occurring in approximately two out of 100,000 people. Men and women are equally affected and most cases occur in people over age 65. The bile duct is a small tube that connects the liver and gallbladder to the small intestine. The ducts carry bile – the liquid that helps break down fat in food during digestion – out of the liver.
Tumors can develop anywhere on the bile ducts and are typically slow growing. However, by the time a diagnosis usually is made, many of the tumors are too advanced to be surgically removed. Other conditions such as primary sclerosing cholangitis, bile duct cysts and chronic biliary irritation, are associated with an increased risk of cholangiocarcinoma.
Our approach to cholangiocarcinoma
UCSF provides state-of-the-art care for cholangiocarcinoma, also called bile duct cancer. In addition to hepatobiliary surgeons, who specialize in the liver, gallbladder and bile duct, our team includes transplant surgeons, diagnostic radiologists, interventional radiologists, medical oncologists, hepatologists, gastroenterologists and anesthesiologists.
For patients who need major surgery, our transplant surgeons apply their expertise in living donor liver transplantation to perform complex reconstruction of the hepatic artery, portal vein or bile duct. This allows us to remove tumors that other centers may have deemed inoperable because they involve major vessels.
Our physician-scientists are dedicated to discovering additional treatments for cholangiocarcinoma through research. Interested patients may have the option to participate in clinical trials, which evaluate potential new therapies.
Signs & symptoms
Cholangiocarcinoma is a rare cancer found in the tissue of the bile ducts. Tumors produce symptoms by blocking the bile ducts. Common symptoms may include:
- Clay colored stools
- Jaundice, which is a yellowing of the skin and eyes
- Itching
- Abdominal pain that may extend to the back
- Loss of appetite
- Unexplained weight loss
- Fever
- Chills
Diagnosis
Your doctor will first ask about your medical history and perform a physical examination. In addition, he or she may order the following tests:
- Computed tomography (CT) scan. An X-ray that uses a computer to provide an image of the inside of the abdomen.
- Magnetic resonance imaging (MRI) scan. This test uses magnetic waves to create an image.
- Ultrasound. This test uses high-frequency sound waves that echo off the body to create a picture.
- Endoscopic retrograde cholangiopancreatography (ERCP). During an ERCP, a flexible tube is inserted down the throat and into the stomach and small intestine. By injecting dye into the drainage tube of the pancreas, your doctor can see the area more clearly.
- Endoscopic ultrasound (EUS). EUS involves passing a thin, flexible tube called an endoscope through the mouth or the anus to exam the lining and walls of the upper and lower gastrointestinal tract and nearby organs such as the pancreas and gall bladder. The endoscope is equipped with a small ultrasound transducer that produces sounds waves that create a viewable image of the digestive track. When combined with fine needle aspiration, EUS becomes a state-of-the-art, minimally invasive alternative to exploratory surgery to remove tissue samples from abdominal and other organs. It also may be used to determine the cause of symptoms such as abdominal pain, to evaluate a growth, to diagnose diseases of the pancreas, bile duct and gall bladder when other tests are inconclusive and to determine the extent of certain cancers of the lungs or digestive tract.
- Percutaneous transhepatic cholangiography (PTC). By injecting dye into the bile duct through a thin needle inserted into the liver, blockages can be seen on X-ray.
- Bile duct biopsy and fine needle aspiration. A tiny sample of the bile duct fluid or tissue is removed and examined under a microscope.
Treatments
Surgery and radiation therapy are the two most common treatments for cholangiocarcinoma.
Surgery
If the cancer is small and has not spread beyond the bile duct, your doctor may remove the whole bile duct and make a new duct by connecting the duct openings in the liver to the intestine. Lymph nodes also will be removed and examined under the microscope to see if they contain cancer. If the cancer has spread and cannot be removed, your doctor may perform surgery to relieve symptoms.
If the cancer is blocking the small intestine and bile builds up in the gallbladder, surgery may be required. During this operation, called a biliary bypass, your doctor will cut the gallbladder or bile duct and sew it to the small intestine.
After complete removal of the tumor, 30 percent to 40 percent of patients survive for at least five years, with the possibility of being completely cured. If the tumor cannot be completely removed, it generally is not possible to cure the patient. In these cases, if you are not a candidate for surgery and have an obstruction, percutaneous transhepatic cholangiography (PTC) and endoscopic retrograde cholangiopancreatography (ERCP) can be used to place plastic or metal stents, which help to relieve obstructions.
Radiation therapy
Radiation therapy is the use of high-energy X-rays to kill cancer cells and shrink tumors. There are two main types of radiation therapy:
- External-beam radiation therapy. Radiation comes from a machine outside the body.
- Internal radiation therapy. Materials that produce radiation, called radioisotopes, are put into the area where the cancer cells are found through thin plastic tubes.
Experimental therapy
There are a couple types of therapy that are currently being studied in clinical trials for the treatment of cholangiocarcinoma, including:
- Chemotherapy. Uses drugs to kill cancer cells
- Biological therapy. Uses the body's immune system to fight cancer
- Photodynamic therapy. Uses a specific type of light and photosensitizing agent to kill cancer cells
Recommended reading
More treatment info
Advanced Endoscopic Procedures
In addition to standard endoscopic procedures, UCSF Medical Center's digestive disorder specialists also offer advanced endoscopic procedures.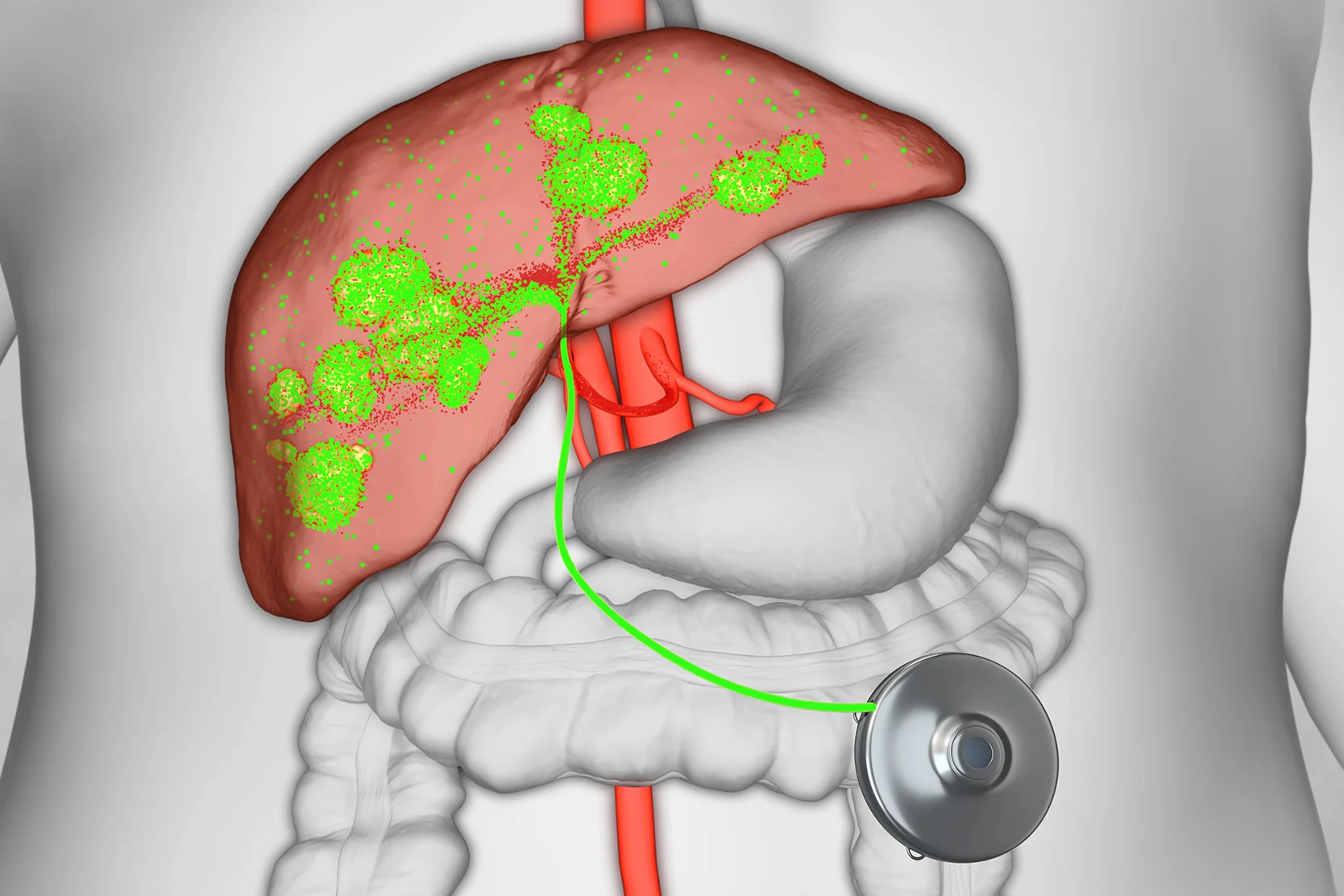
Hepatic Artery Infusion Pump
This implanted pump delivers chemotherapy directly to liver tumors, providing an effective treatment option for metastatic colon or bile duct cancer.
Awards & recognition

Best in California and No. 7 in the nation for cancer care

Best in Northern California for gastroenterology & GI surgery

Designated comprehensive cancer center
Related services & treatments
Specialties
- Hepatobiliary and Pancreatic Surgery
- Liver Transplant Surgery
- Hepatology
- Gastroenterology
- Medical Oncology
Treatments
- Hepatic Lobectomy
- Liver Transplant
- Anastomosis of Bile Duct
- Hepatic Artery Infusion Pump
- Cancer Chemotherapy
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.























