Breast Cancer
On this page
Overview
What is breast cancer?
Breast cancer is the second most common cancer among women, with more than 200,000 new cases diagnosed each year nationwide. While known primarily as a women’s disease, men can also get breast cancer.
Breast cancer begins with abnormal cells developing in breast tissue. The cancer may be confined to the breast or spread to other parts of the body. The most common type begins in the ducts that carry milk to the nipple. But cancer also may occur in the small sacs that produce milk, called lobules, or in other breast tissue. Because breast cancer varies widely, treatment depends on the type and stage as well as the individual patient's needs.
Our approach to breast cancer
Breast cancer survival rates today are higher than ever due to advances in diagnosis and treatment. At the UCSF Carol Franc Buck Breast Care Center, we specialize in screening to enable early detection, providing more effective and less toxic therapies, educating patients and pursuing cutting-edge research. We are committed to discovering new and better ways to prevent and treat breast cancer.
UCSF offers the highest quality breast cancer care in a respectful and supportive environment. To serve each of our patients, our surgeons, oncologists, radiologists, psychologists and nutritionists work as a team to heal the whole person, both physically and emotionally.
Types of breast cancer
Breast cancer may be found in several forms, depending on where the cancer started and how far it has progressed.
Breast cancer in situ, DCIS and LCIS
When breast cancer is found early, usually through a mammogram, it's called breast cancer in situ (meaning in its original position) or noninvasive cancer. However, it can develop into invasive breast cancer.
Two types of breast disease in situ are:
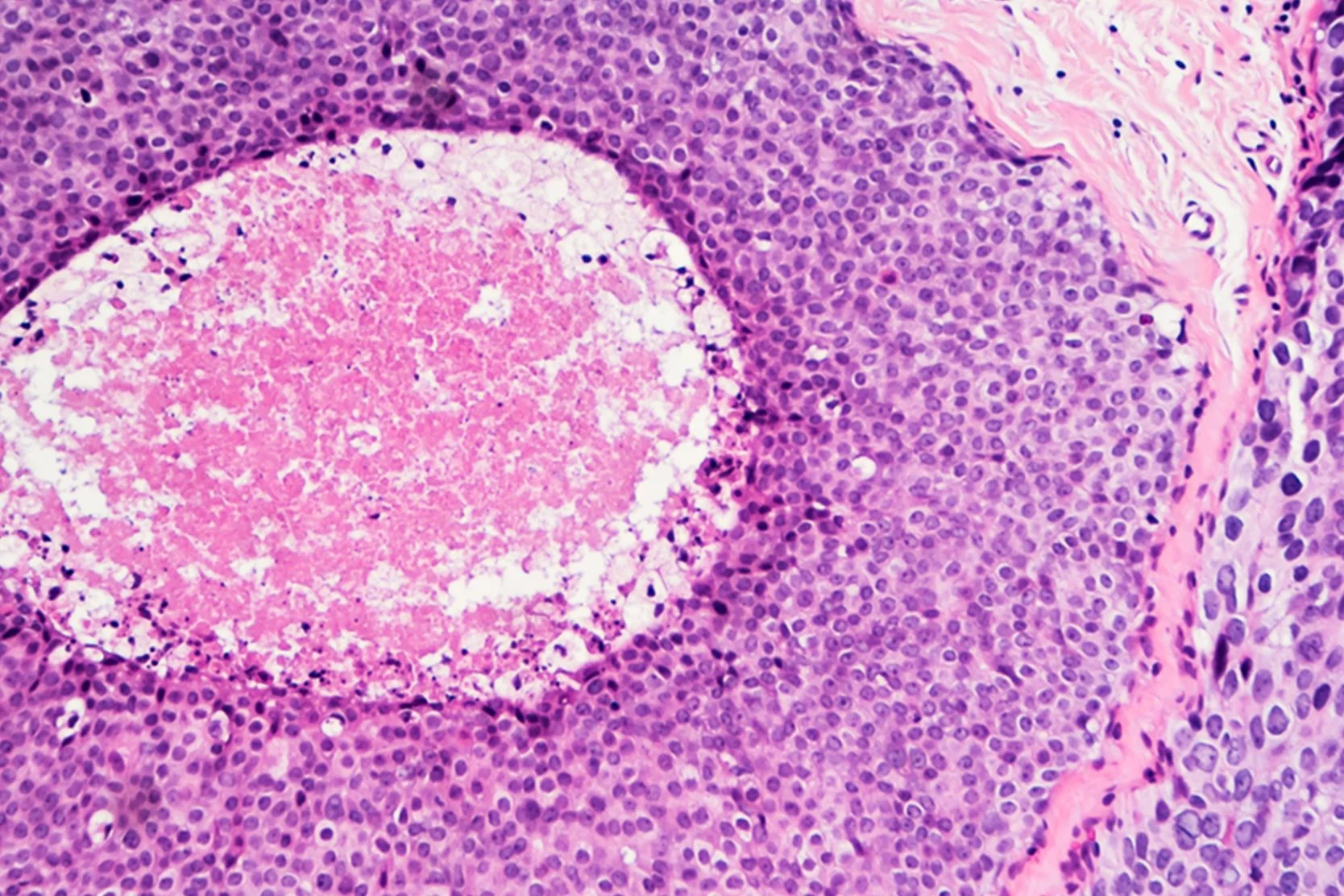
- DCIS (ductal carcinoma in situ). Abnormal cells are only in the lining of a milk duct (they haven't spread beyond the duct). If these cells aren't removed, some may change over time and become invasive cancers. DCIS is sometimes called intraductal carcinoma.
- LCIS (lobular carcinoma in situ). Abnormal cells are found only in the lining of a milk lobule. LCIS is noninvasive and not considered breast cancer. However, it signals an increased risk of developing invasive cancer. LCIS is sometimes found in a biopsy for another lump or when an unusual change is detected on a mammogram.
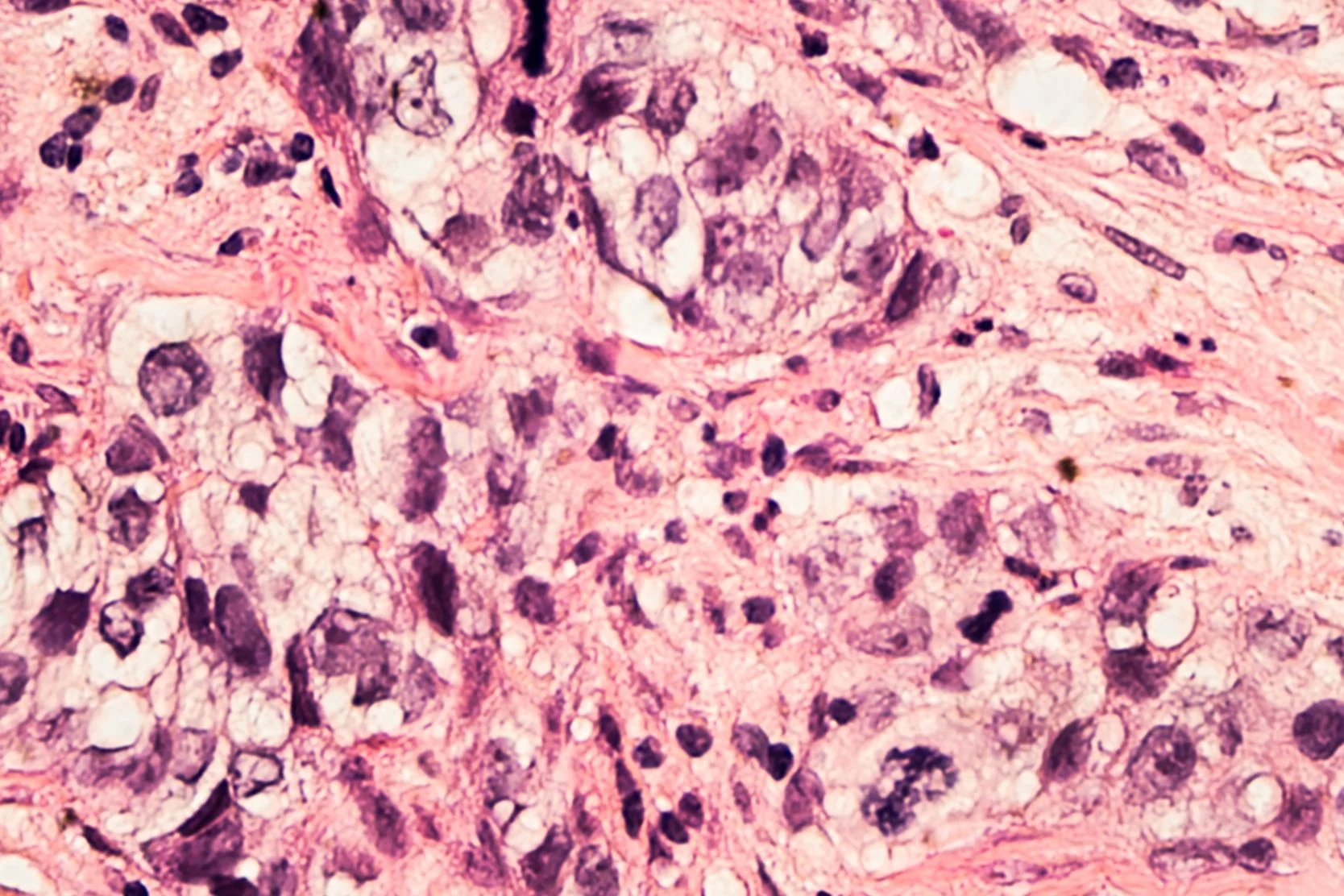
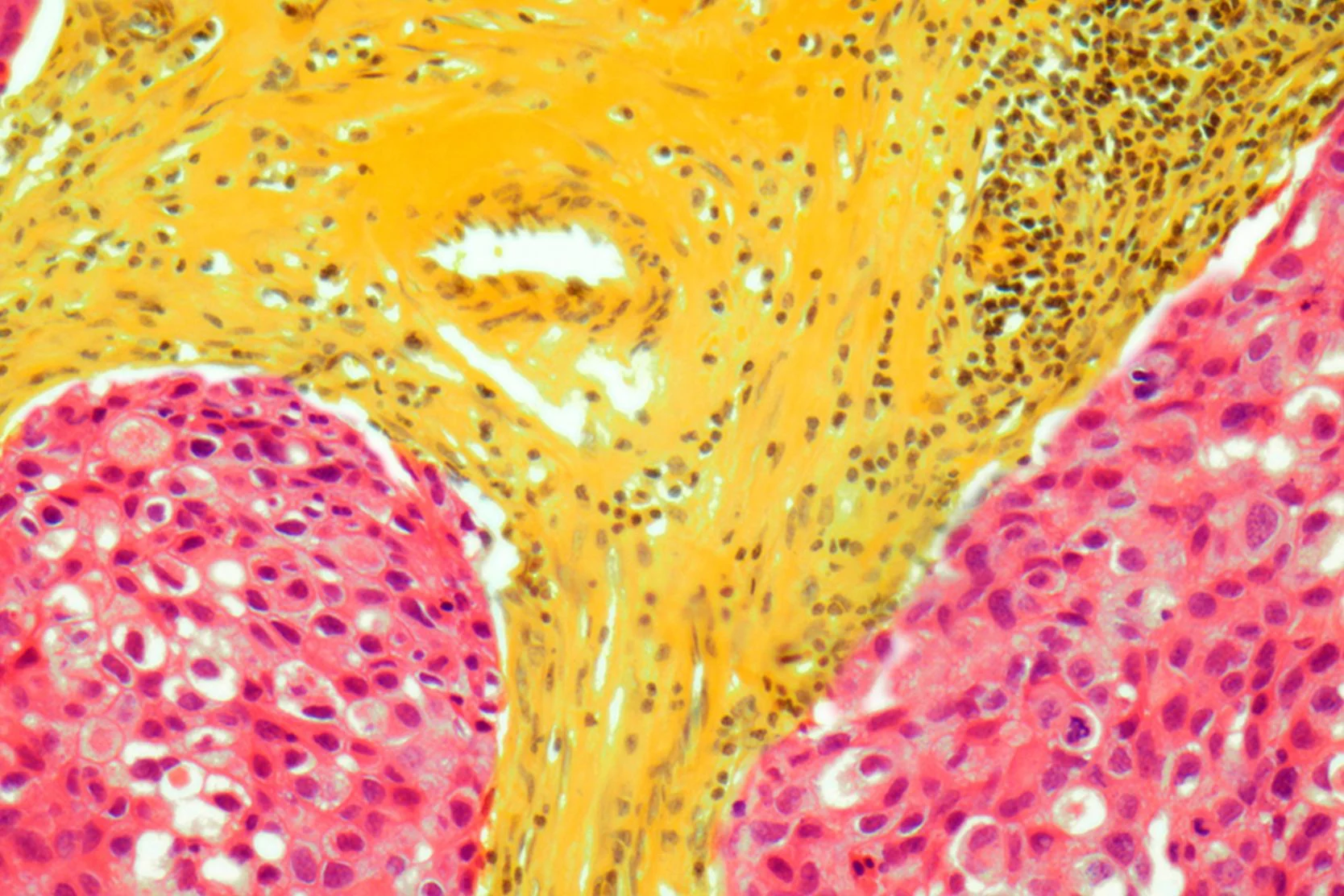
Invasive breast cancer
When cancer cells form in the ducts or milk lobules and spread to the breast tissue around them, the cancer is considered invasive. Tumors can be found during a breast exam or through screening tests, such as a mammogram. The severity of the cancer and best course of treatment depend on the tumor's size, what the cells look like under a microscope, and whether the cancer has spread to lymph nodes (small, bean-shaped structures that are part of the body's immune system).
Metastatic breast cancer
The cancer is metastatic when it has spread from the breast to other organ systems – usually the bones, lungs, liver and brain. The cancer travels to these organs through the bloodstream or lymphatic system. If metastatic cancer develops, it is usually months or years after the initial breast cancer diagnosis.
Inflammatory breast cancer
Inflammatory breast cancer is a rare but aggressive type. The breast may look red and feel warm. Ridges, welts or hives may appear on the breast, or its skin may look wrinkled. Inflammatory breast cancer is sometimes misdiagnosed as an infection.
Recurrent breast cancer
This is cancer that has come back (recurred) after treatment. It may reappear in the breast, develop in soft tissues of the chest or chest wall, or occur in another part of the body.
Symptoms of breast cancer
Early in the development of breast cancer, people don't usually experience pain. In fact, when breast cancer first appears, there may be no symptoms. But as the cancer grows, it may cause changes. Watch for differences in appearance or sensation, including:
- A lump or thickening in or near a breast or the underarm area
- A change in the breast's size or shape
- Nipple discharge or tenderness
- The nipple pulling inward (inverting)
- Ridges or pitting of a breast, making the skin look like the outside of an orange
- Any change in the look or feel of the skin of a breast, areola or nipple, such as warmth, swelling, redness or scaliness
Diagnosis of breast cancer
To diagnose breast cancer, your provider will usually perform a physical exam and order an imaging test, such as a mammogram or ultrasound. Depending on the results, you may also have a tissue biopsy (a procedure to take a sample for microscopic analysis).
If cancer is found in your breast, you'll undergo additional tests to determine the stage of the disease. Staging is a way of assessing whether the cancer has spread and, if so, to which parts of the body. Blood and imaging tests are typically used. Your treatment plan will depend on the results of these tests as well as your own needs and preferences. You can find more information on the staging of breast cancer in Basic Facts About Breast Health.
Imaging for breast cancer
Imaging tests are used to diagnose breast cancer and to evaluate its stage and extent. Based on the results, your provider may recommend further tests or therapy – or determine that no treatment is necessary.
Imaging tests may include:
- Screening mammogram. A mammogram is a low-dose X-ray of the breast. This is the best test to check for breast cancer in people without signs of it.
- Diagnostic mammogram. This type of mammogram is used to investigate suspicious changes in the breast, such as a new lump or breast pain or nipple discharge. It's also used to evaluate suspicious findings on a screening mammogram.
- Breast ultrasound. This test uses high-frequency sound waves to show whether a lump is solid or filled with fluid. It may be used along with diagnostic mammography or an MRI to answer questions about a specific area of the breast.
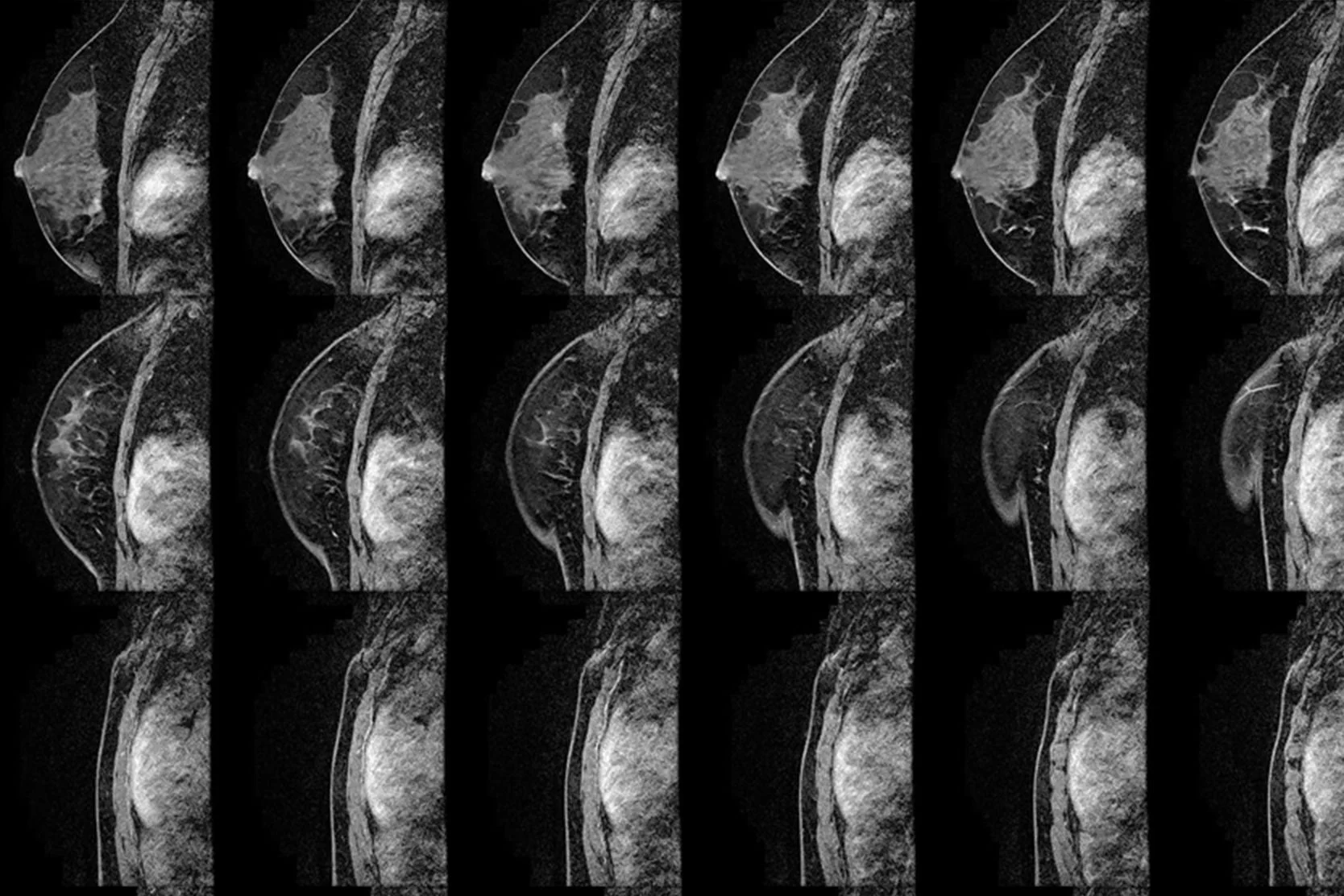
- Breast magnetic resonance imaging (MRI). This type of MRI scan can reveal abnormalities that aren't visible through mammography or ultrasound. Each scan produces hundreds of images.
The American Cancer Society recommends that certain women with an especially high risk of developing breast cancer have an MRI scan along with their yearly mammogram. A breast MRI is noninvasive, with no radiation exposure. But breast MRI is an evolving technology and shouldn't replace standard screening and diagnostic procedures, such as in-clinic exams during a regular checkup, self-exams, mammograms and biopsies.
Biopsy for breast cancer
A biopsy may be used to determine whether a breast lump or other abnormal tissue is cancer. During a biopsy, a surgeon, pathologist or radiologist removes a portion or all of the suspicious tissue. The tissue is then examined under a microscope by a pathologist, who checks for cancer cells and makes the diagnosis.
Types of biopsies include:
- Fine-needle aspiration (FNA) biopsy. Using a small, thin needle, the doctor takes two or three samples of tissue from the breast lump for examination.
- Stereotactic core biopsy. Using a biopsy needle, the doctor removes tissue from your breast while it’s pressed down to hold it in position, similar to what happens during a mammogram.
- Magseed or needle (wire) localization biopsy. Guided by imaging, doctors mark the location of the abnormal tissue by placing a tiny magnetic seed or wire. The tissue is then surgically removed and analyzed.
Decision-making consultation
If you're diagnosed with breast cancer, the Patient Support Corps at the UCSF Breast Care Center is here to help. The staff can offer information and guidance as you navigate conversations with your doctors and make decisions about your treatment.
Treating breast cancer
Treatment for breast cancer may include surgery as well as radiation, chemotherapy and hormone therapy. Local treatments, such as surgery and radiation therapy, remove, destroy or control cancer cells in specific areas. Systemic treatments, such as chemotherapy and hormone therapy, destroy or reduce cancer throughout the body.
Depending on your condition, you may receive one treatment, a combination of therapies at the same time or a series over time.
Surgery for breast cancer
For most types of breast cancer, surgery is the most common treatment. Mastectomy and lumpectomy are two main surgeries for removing tumors. Additional procedures may be done to check for cancer in your lymph nodes or to reconstruct your breast during or after removal.
Your doctor may discuss these procedures with you:
- Lumpectomy. A surgeon removes the cancer and some normal tissue around it, preserving as much healthy tissue as possible. Some lymph nodes from the armpit may also be removed to determine whether the cancer has spread. After a lumpectomy, most patients receive radiation therapy to destroy any remaining cancer cells.
- Mastectomy. A surgeon removes all the tissue of one or both breasts. Other nearby tissues, such as lymph nodes, may be removed at the same time to check whether the cancer has spread.
- Sentinel lymph node biopsy. A surgeon removes one or more sentinel lymph nodes for examination. Sentinel lymph nodes are the ones most likely to contain cancerous cells if the cancer has spread from the primary area.
- Breast reconstruction. A surgeon rebuilds the breast after a mastectomy, creating a breast that looks and feels as natural as possible. This procedure may be done using breast implants or the patient's own body tissue, although a variety of factors affect an individual's options.
Radiation therapy for breast cancer
Radiation therapy for breast cancer uses high-energy rays or particles to attack the disease. This treatment is delivered in effective, tolerable doses to kill tumor cells or inhibit their growth and division.
Radiation therapy is used, along with surgery, to treat early-stage breast cancer. It may also be used in more advanced breast cancer to control the disease or to relieve symptoms, such as pain.
Chemotherapy for breast cancer
Chemotherapy uses drugs to kill cancer cells. For breast cancer, the drugs are typically a combination given by mouth and injection. Chemotherapy enters the bloodstream and travels throughout your body.
Chemotherapy is most commonly used to:
- Decrease the chance of cancer recurring after surgery
- Shrink breast cancer after surgery when the tumor is large or inflammatory
- Control metastatic breast cancer that has spread to other organs
Hormone therapy for breast cancer
This therapy changes the hormonal environment in your body, affecting the growth and behavior of some breast cancers. If your breast cancer produces an estrogen receptor or progesterone receptor, hormone therapy can effectively treat it at early, metastatic or advanced stages. This therapy can also be used to prevent recurrence.
Awards & recognition

Best in California and No. 7 in the nation for cancer care

Designated comprehensive cancer center
Recommended reading
Related programs

UCSF Patient Support Corps
Receiving a breast cancer diagnosis is stressful. Get guidance, support and answers to your questions here as you consider your options and make decisions.
More treatment info
Helpful resources
Support services
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.